Yeast infections during pregnancy are very common, particularly during the second trimester. Increased estrogen alters the normal balance of bacteria and yeast in the vagina, causing an overgrowth of yeast. This leads to odd-smelling, white vaginal discharge.
Causes of Yeast Infections
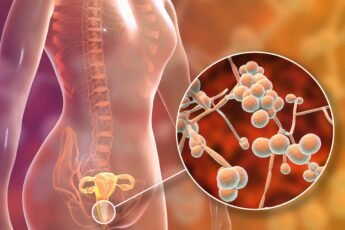
The vaginal fungus Candida albicans causes yeast infections. This fungus is otherwise completely normal. The vaginal imbalance is exacerbated by factors like excess moisture and moist regions are ripe grounds for fungal growth.
Data of the Centers for Disease Control and Prevention show 3 of 4 women have had a yeast infection at least once, and these incidences often occurred during pregnancy. While they cause discomfort, yeast infections do not harm your unborn or affect your pregnancy.
If you think you might have a yeast infection, see a medical professional for accurate diagnosis and treatment. Other infections can manifest with similar symptoms.
According to the National Institutes of Health, yeast infections (vulvovaginal candidiasis or VVC) occur at least twice in over 40% of women. Another factor behind the increased likelihood of VVC during pregnancy is higher glycogen content in vaginal secretions.
High blood sugar, hormonal changes that come with pregnancy, vaginal intercourse, blood, and semen can also contribute to the overgrowth of this fungus. Douching can cause a yeast infection or aggravate an existing one.
Symptoms of Yeast Infections
You may have one or more of the following symptoms of a yeast infection:
- Yellowish/greenish discharge with the thickness of cottage cheese. It might smell of beer or bread
- Whitish/yellowy discharge with the consistency of cottage cheese. It might also smell of beer or bread.
- An increase in discharge
- Burning sensation during sex or urination
- Irritation, redness, or itching of the lips and inside of the vagina
Could I Have Another Infection?
If a doctor has ruled out a yeast infection after doing tests, but you still have one or more of the above symptoms, you could have a sexual transmitted infection like gonorrhea, chlamydia, or trichomoniasis. To get tested for these, you need to go to a gynecologist, who will perform a swab and have the sample sent to a lab. Results usually come back within one or two days.
Not all medication is suitable during pregnancy, so the patient will discuss their individual situation with their doctor, including any possible effects of medication on the fetus.
The symptoms of a yeast infection are similar to those of a vaginal infection called bacterial vaginosis. More information about the difference between bacterial vaginosis and a yeast infection is available here.
Getting Tested and Treated for a Yeast Infection
Your doctor or clinician will use a painless swab to obtain a sample of your vaginal secretion and have it examined. Normally, yeast infections are treated using over-the-counter medications, and yeast infections during pregnancy are not an exception. These OTC medications are available as ointments, creams, or suppositories and include Miconazole (Monistat 3), Clotrimazole (Mycelex, Lotrimin AF), and Terconazole. They are safe to use during pregnancy and don’t carry a risk of complications or of harm to the unborn baby. It’s best to take these over one week. If you’re pregnant, oral medication isn’t recommended. Fluconazole and other commonly prescribed anti-fungals medications should be avoided, particularly early on in the pregnancy.
Should I Worry About Thrush?
If you don’t get your yeast infection treated, you can pass it to your baby during delivery. This is known as thrush, an imbalance of yeast usually occurring in the mouth. If this happens, the baby could develop white patches in its mouth. When you breastfeed them, they can pass the thrush back to you. To treat it, you can use antifungal cream for you and other mild antifungal medication for the child.
It can take up to two weeks to stop experiencing symptoms or completely clear up the yeast infection. It is recommended to use a starch-free drying powder after the infection has cleared up to prevent a recurring one.
Preventing Recurring Infections: Tips
Apart from drying powder, recurring infections can usually be avoided by eliminating contributing factors. Wearing tight pants and douching are two of the most notorious offenders. Always wear loose cotton clothes and underwear. After showering or washing your privates, use your blow dryer on cool and low to dry the outside area around your vagina. Use gentle, unscented soap. After using the bathroom, always wipe from front to back.
Do not use any feminine hygiene sprays, use perfumed soaps or take bubble baths, eat anything that contains “lactobacillus acidophilus”, or use colored or perfumed toilet paper. Lactobacillus acidophilus is a bacterium contained in some yogurt that can have an adverse effect on the fetus.
The bacteria causing yeast infections thrive in wet environments, so change as soon as possible after swimming or working out.
Sugar contributes to yeast growth. Those with a sweet tooth know how it can become a fang during pregnancy, so that’s going to be a struggle, but at least you know.
Finally, get plenty of rest. Pregnancy is trying on the body as it is, and if your workload isn’t getting any less, your immune system will be struggling against the infection.
Getting a Timely Diagnosis is Key
Getting an accurate and timely diagnosis is crucial because this will ensure the most effective treatment for your condition. Once you begin taking OTC medication, you should see some improvement within a few days. Contact your doctor again if you don’t or symptoms worsen – and don’t worry!
Dani Fogel. is a Communication Coordinator at Brandable, based in Los Angeles, CA. She works on the Queen V brand within the company’s Digital and Ecommerce department.
Sources
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2654841/
https://www.whattoexpect.com/pregnancy/yeast-infection/
https://www.medicalnewstoday.com/articles/322210.php
https://www.webmd.com/baby/yeast-infection
0 200

No Comments