Seretide accuhaler and evohaler both contain two active ingredients, fluticasone and salmeterol.
Several classes of medications are available for the treatment of asthma, and often they must be taken concurrently to achieve asthma control. Based on the understanding of asthma as an inflammatory disease, the National Heart Lung and Blood Institute guidelines provide a stepwise approach to pharmacologic therapy.
Corticosteroid therapy, principally inhaled corticosteroid (ICS) therapy, is considered the most effective anti-inflammatory treatment. In cases of moderate-to-severe persistent asthma, the addition of a second long-term control medication to ICS therapy is one recommended treatment option.
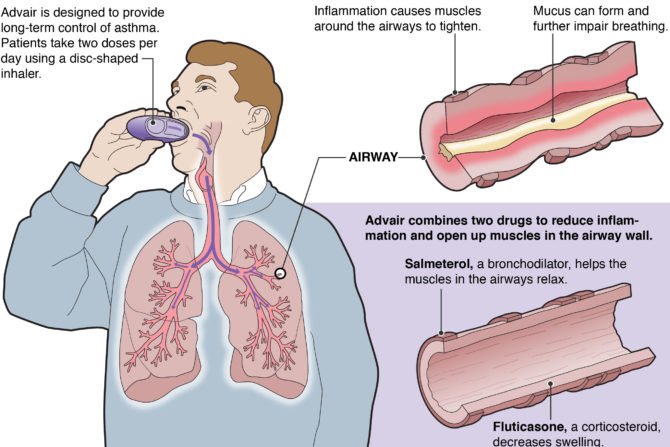
A combination-product inhaler (Advair, Seretide) was developed to treat both the inflammatory and bronchoconstrictive components of asthma by delivering a dose of the ICS, fluticasone propionate, and a dose of the long-acting beta2-adrenergic (LABA) bronchodilator, salmeterol.
The Advair Diskus is available in 3 strengths of fluticasone propionate (100, 250, and 500 microg) and a fixed dose (50 microg) of salmeterol. Combination treatment with both ICS and LABA provides greater asthma control than increasing the ICS dose alone, while at the same time reducing the frequency and perhaps the severity of exacerbations. Furthermore, salmeterol added to ICS therapy provides superior asthma control compared with the addition of leukotriene modifiers or theophylline.
The superior control is likely a consequence of the complementary actions of the drugs when taken together, including the activation of the glucocorticoid receptor by salmeterol. By combining anti-inflammatory treatment with a long-acting beta2-agonist in a single inhaler (1 inhalation twice daily), physicians can provide coverage for both the inflammatory and bronchoconstrictive aspects of asthma without introducing any new or unexpected adverse consequences.
The most common drug-related adverse events were those known to be attributable to the constituent medications (ICS therapy and/or LABA therapy). Although the benefits of combined ICS plus LABA therapy can be achieved with separate inhalers, the convenience of the combination product may improve patient adherence and may therefore reduce the morbidity of asthma.
This combination of medicines in Seretide is used for asthma that is not sufficiently controlled by using a regular steroid inhaler with a reliever inhaler (eg salbutamol) as required. Seretide should be used regularly, even when you have no asthma symptoms, to reduce the inflammation in the lungs and to help keep the airways open. You should still keep your reliever inhaler with you at all times in case you do have an asthma attack.
How does it work?
Seretide accuhaler and evohaler both contain two active ingredients, fluticasone and salmeterol.
Fluticasone is a type of medicine known as a corticosteroid. Corticosteroids are hormones that are produced naturally by the adrenal glands. They have many important functions, including control of inflammatory responses. Fluticasone is a synthetic corticosteroid and is used to decrease inflammation in the lungs. (NB. Corticosteroids are often simply called steroids, but it should be noted that they are very different from another group of steroids, called anabolic steroids, which have gained notoriety because of their abuse by some athletes and body builders.)
When fluticasone is inhaled into the lungs it is absorbed into the cells of the lungs and airways. Here it works by preventing the release of certain chemicals that are important in the immune system. These chemicals are normally involved in producing immune and allergic responses that result in inflammation. By decreasing the release of these chemicals in the lungs and airways, inflammation is reduced.
In asthma, the airways tighten due to inflammation and can also be blocked by mucus. This makes it difficult for air to get into and out of the lungs. By reducing the inflammation and excess mucus formation, fluticasone helps prevent asthma attacks.
Salmeterol is a type of medicine called a long-acting beta 2 agonist. It works by acting on receptors in the lungs called beta 2 receptors. When salmeterol stimulates these receptors it causes the muscles in the airways to relax. This allows the airways to open and makes it easier to breathe.
Salmeterol doesn’t open the airways as quickly as short-acting beta 2 agonists such as salbutamol or terbutaline, however, it does keep the airways open for much longer. The effects of salmeterol last for about 12 hours, whereas those of salbutamol or terbutaline last for about 3 to 5 hours. This means salmeterol is used to prevent asthma attacks, wheezing, chest tightness or shortness of breath, rather than to relieve them.
How is this medicine taken?
Fluticasone and salmeterol are taken using an inhaler device. Inhaling the medicine allows it to act directly in the lungs where it is needed most. It also reduces the potential for side effects in other parts of the body, as the amount absorbed into the blood through the lungs is lower than if the medicines were taken by mouth.
It is very important to learn how to use your inhaler correctly, as otherwise you won’t be breathing the right dose of medicine into your lungs. Instructions will be provided with your inhaler. However, your doctor, nurse or pharmacist can also show you how to use your inhaler and can check that you are using it correctly.
Seretide is available as two different types of inhaler device; the evohaler and the accuhaler.
- Seretide evohaler is a metered dose inhaler (sometimes called an MDI or aerosol inhaler) that delivers the medicine as a fine spray or mist. With this inhaler you have to co-ordinate pressing down the canister and breathing in the spray. Follow this link for general instructions on how to use a metered dose inhaler. Seretide evohaler can also be used with a spacer device such as the Volumatic or AeroChamber Plus. If you do use a spacer it is important that you always use the same make of spacer with Seretide evohaler, because changing makes can change the amount of medicine that is delivered to your lungs.
- Seretide accuhaler is a dry powder inhaler. It comes pre-loaded with blisters containing individual doses of the medicine as a powder. To take a dose you have to slide the lever on the inhaler. This opens a blister inside the inhaler, making a dose ready for you to inhale. You then breathe out fully, put the mouthpiece to your lips and breathe in steadily and deeply through your mouth. More detailed instructions are provided with the accuhaler.
- Inhaled corticosteroids can sometimes cause a fungal infection in the mouth called oral thrush. To minimise the chances of this you should rinse your mouth with water or clean your teeth after inhaling each dose. Using a spacer device can also help avoid this problem. Consult your doctor if you develop white patches in your mouth or throat, as these are symptoms of thrush and it may need to be treated.
- If you forget to take a dose, just take your next dose when it is due. Do not take a double dose to make up for a missed dose.
- Do not stop using your inhaler regularly, even if you don’t have any symptoms, unless advised to by your doctor.
Warning
- This medicine is known as a preventer and it should be taken regularly to prevent asthma attacks or wheezing. It should not be used to relieve an asthma attack or breathing difficulties, as it won’t work quickly enough. An asthma attack needs to be treated with a medicine that quickly opens the airways, such as salbutamol or terbutaline. These are known as relievers, and you should make sure you carry your reliever inhaler with you at all times to relieve an asthma attack if it happens.
- Consult your doctor if you need to use your reliever more frequently than normal, or if it becomes less effective at treating attacks, as this may indicate that your asthma is getting worse and your doctor may need to prescribe you another medicine.
- Do not exceed the dose of this medicine that your doctor has prescribed for you.
- Inhalers may cause an unexpected increase in wheezing and difficulty breathing (paradoxical bronchospasm) straight after using them. If this happens, don’t use the inhaler again, use your reliever inhaler to open your airways and consult your doctor.
- Inhaled corticosteroids have considerably fewer side effects than steroids taken by mouth. However, when taken for long periods of time at high doses, inhaled steroids do have the potential to cause side effects such as glaucoma, cataracts, thinning of the bones (osteoporosis), slowed growth in children and adolescents, Cushings syndrome, changes in mood or behaviour, and to suppress the functioning of the adrenal glands (glands that produce natural steroid hormones). For this reason your doctor will prescribe the lowest effective dose to control your symptoms, and monitor for these side effects. It is recommended that children receiving long-term treatment with corticosteroids have their growth monitored. If a child’s growth appears to be slowed your doctor may refer them to a specialist respiratory paediatrician. For further information talk to your doctor or pharmacist.
- If you need to take high doses of Seretide for a long time, your body may become temporarily reliant on the medicine. This is because long-term use of corticosteroids can cause the adrenal glands to stop producing natural steroids. For this reason treatment must not be suddenly stopped. If your doctor wants you to stop treatment your dose should be tapered down gradually, to allow the adrenal glands to start producing adequate amounts of natural steroids again. People taking high doses of Seretide for a long time may also need to take extra steroid medicines during times of physical stress, for example illnesses, serious accidents or surgery. This is because your adrenal glands would normally produce more steroid hormones to cope with these situations, however, if the action of your adrenal glands is suppressed, this increase in hormones won’t happen naturally. For more information talk to your doctor or pharmacist.
- People with severe asthma should have regular blood tests to monitor the amount of potassium in their blood. This is because low oxygen levels in the blood (hypoxia) and various asthma medicines, including this one, can lower blood potassium levels.
Use with caution in
- People with a history of tuberculosis infection in the lungs.
- Heart disease.
- Irregular heartbeats (arrhythmias).
- High blood pressure (hypertension).
- Overactive thyroid gland (hyperthyroidism).
- Diabetes.
- People with low levels of potassium in their blood (hypokalaemia).
Not to be used in
- People with known sensitivity or allergy to any ingredient.
- Seretide is not recommended for children under four years of age.
This medicine should not be used if you are allergic to one or any of its ingredients. Please inform your doctor or pharmacist if you have previously experienced such an allergy. If you feel you have experienced an allergic reaction, stop using this medicine and inform your doctor or pharmacist immediately.
Pregnancy and breastfeeding
Certain medicines should not be used during pregnancy or breastfeeding. However, other medicines may be safely used in pregnancy or breastfeeding providing the benefits to the mother outweigh the risks to the unborn baby. Always inform your doctor if you are pregnant or planning a pregnancy, before using any medicine.
- It is important that asthma is well controlled in pregnant women because severe asthma attacks can be dangerous to the pregnancy. Wherever possible, asthma medications should be taken by inhaler, as this minimises the amount of medicine that enters the bloodstream and crosses the placenta. The manufacturer states that Seretide should be used with caution during pregnancy. However, it is generally considered that asthma inhalers can be taken as usual during pregnancy. For further medical advice talk to your doctor or pharmacist.
- Salmeterol may pass into breast milk in small amounts. It is not known if fluticasone passes into breast milk. However, in general, asthma inhalers can be used as normal during breastfeeding, because the amount of medicine that passes into the breast milk after using an inhaler is negligable and unlikely to harm the baby. Seek further medical advice from your doctor.
Side effects
Medicines and their possible side effects can affect individual people in different ways. The following are some of the side effects that are known to be associated with this medicine. Just because a side effect is stated here, it does not mean that all people using this medicine will experience that or any side effect.
Very common (affect more than 1 in 10 people)
- Headache.
- Increased number of colds in people with COPD.
Common (affect between 1 in 10 and 1 in 100 people)
- Thrush infection of the mouth and throat (oral thrush). This can usually be avoided by rinsing the mouth out with water and spitting it out immediately after each time you use your inhaler. If you do get oral thrush your doctor can prescribe an antifungal medicine to treat it.
- Throat irritation.
- Hoarse voice.
- Muscle cramps.
- Pain in the muscles or joints.
- Sinusitis in people with COPD.
- Low level of potassium in the blood in people with COPD (hypokalaemia – see warning section above).
- Pneumonia and bronchitis in people with COPD.
- Bruising or bone fractures in people with COPD.
Uncommon (affect between 1 in 100 and 1 in 1000 people)
- Shaking, usually of the hands (tremor).
- Anxiety.
- Sleep disorders.
- Awareness of your heartbeat (palpitations).
- Increased heart rate (tachycardia).
- Chest pain.
- Cataracts.
Rare (affect between 1 in 1000 and 1 in 10,000 people)
- Unexpected narrowing of the airways (paradoxical bronchospasm – see warning section above).
- Abnormal heartbeats (arrhythmias).
- Glaucoma.
- Behavioural changes, including hyperactivity and irritability (mostly in children).
- Systemic steroid effects such as Cushing’s syndrome (moon-shaped face), suppression of the adrenal glands, slowed growth in children and adolescents or decreased bone mineral density may occur, usually only after taking high doses for prolonged periods of time – see warning section above.
The side effects listed above may not include all of the side effects reported by the medicine’s manufacturer.
For more information about any other possible risks associated with this medicine, please read the information provided with the medicine or consult your doctor or pharmacist.
How can this medicine affect other medicines?
It is important to tell your doctor or pharmacist what medicines you are already taking, including those bought without a prescription and herbal medicines, before you start treatment with this medicine. Similarly, check with your doctor or pharmacist before taking any new medicines while using this one, to make sure that the combination is safe.
People who are using salmeterol should not take medicines called beta-blockers, such as atenolol, propranolol or timolol. This is because beta-blockers have an opposite action to this medicine and can cause the airways to narrow. This can result in breathing difficulties for people with asthma or COPD. This problem has also sometimes been seen with eye drops containing beta-blockers, eg used for glaucoma.
Salmeterol and fluticasone can sometimes cause a serious decrease in the levels of potassium in the blood (hypokalaemia). This effect can be increased by the following medicines, which can also lower levels of potassium in the blood:
- diuretics, such as bendroflumethiazide and furosemide.
- other beta 2 agonists, such as salbutamol
- other corticosteroids, such as prednisolone
- xanthine derivates, such as theophylline or aminophylline.
Since a low blood potassium level can have serious adverse effects, people with severe asthma or COPD, who may be taking several of these medicines, should have their blood potassium levels monitored regularly.
The following medicines may increase the amount of salmeterol or fluticasone that is found in the bloodstream after inhaling this medicine:
- the azole antifungals ketoconazole, itraconazole or voriconazole
- the macrolide antibiotics clarithromycin or telithromycin
- protease inhibitors for HIV infection such as ritonavir
- telaprevir.
These medicines can therefore increase your exposure to fluticasone and salmeterol and so increase the risk of side effects on the rest of the body. Due to the risk of systemic steroid side effects, such as decreased production of natural steroid hormones by the adrenal glands (adrenal suppression) and Cushing’s syndrome, Seretide is not recommended for people who are taking ritonavir. The antifungals ketoconazole and itraconazole should be used with caution in people using Seretide. Long courses of treatment with these antifungals should be avoided where possible.
What are some things I need to know or do while I take Fluticasone and Salmeterol Inhaler?
- Tell all of your health care providers that you take this medicine. This includes your doctors, nurses, pharmacists, and dentists.
- It may take 1 week to see the full effect.
- If you have high blood sugar (diabetes), talk with your doctor. This medicine may raise blood sugar.
- Call your doctor right away if your breathing problems get worse, if your rescue inhaler does not work as well, or if you need to use your rescue inhaler more often.
- When changing from an oral steroid to another form of a steroid, there may be very bad and sometimes deadly side effects. Signs like weakness, feeling tired, dizziness, upset stomach, throwing up, not thinking clearly, or low blood sugar may happen. Call your doctor right away if you have any of these signs. If you have a bad injury, have surgery, or any type of infection, you may need extra doses of oral steroids. These extra steroids will help your body deal with these stresses. Carry a warning card saying that there may be times when you may need extra steroids.
- Long-term use may raise the chance of cataracts or glaucoma. Talk with the doctor.
- Have your eye pressure checked if you are on fluticasone and salmeterol inhaler for a long time. Talk with your doctor.
- This medicine may cause weak bones (osteoporosis) with long-term use. Talk with your doctor to see if you have a higher chance of weak bones or if you have any questions.
- Have a bone density test as you have been told by your doctor. Talk with your doctor.
- You may have more chance of getting an infection. Wash hands often. Stay away from people with infections, colds, or flu.
- Chickenpox and measles can be very bad or even deadly in some people taking steroid drugs like this medicine. Avoid being near anyone with chickenpox or measles if you have not had these health problems before. If you have been exposed to chickenpox or measles, talk with your doctor.
- Do not take more of fluticasone and salmeterol inhaler or use it more often than you have been told. Deaths have happened when too much of this type of drug has been taken. Talk with your doctor.
- If you are 65 or older, use this medicine with care. You could have more side effects.
- Use with care in children. Talk with the doctor.
- This medicine may affect growth in children and teens in some cases. They may need regular growth checks. Talk with the doctor.
- Tell your doctor if you are pregnant or plan on getting pregnant. You will need to talk about the benefits and risks of using fluticasone and salmeterol inhaler while you are pregnant.
- Tell your doctor if you are breast-feeding. You will need to talk about any risks to your baby.
How is this medicine best taken?
Use this medicine as ordered by your doctor. Read all information given to you. Follow all instructions closely.
- Follow how to use as you have been told by the doctor or read the package insert.
- To gain the most benefit, do not miss doses.
- Keep using fluticasone and salmeterol inhaler as you have been told by your doctor or other health care provider, even if you feel well.
- Use this medicine at the same time of day.
- For breathing in only.
- Shake well before use.
- Prepare puffer (inhaler) before first use, when puffer has not been used for more than 4 weeks, or if it is dropped. Spray 4 test sprays into the air. Shake well before each test spray.
- Put the cap back on after you are done using your dose.
- This medicine may catch on fire. Do not use near an open flame or while smoking.
- This puffer (inhaler) has a dose counter to keep track of how many doses are left. Throw the inhaler away when the dose counter has a 0 in it.
- Have your puffer (inhaler) use checked with your doctor at each visit. Read and follow facts on how to use the puffer. Make sure you use the puffer the right way.
- Rinse out mouth after each use. Do not swallow the rinse water. Spit it out.
- If using more than 1 type of puffer (inhaler), ask the doctor which puffer to use first.
What do I do if I miss a dose?
- Skip the missed dose and go back to your normal time.
- Do not take 2 doses at the same time or extra doses.
side effects
Even though it may be rare, some people may have very bad and sometimes deadly side effects when taking a drug. Tell your doctor or get medical help right away if you have any of the following signs or symptoms that may be related to a very bad side effect:
- Signs of an allergic reaction, like rash; hives; itching; red, swollen, blistered, or peeling skin with or without fever; wheezing; tightness in the chest or throat; trouble breathing or talking; unusual hoarseness; or swelling of the mouth, face, lips, tongue, or throat.
- Signs of infection like fever, chills, very bad sore throat, ear or sinus pain, cough, more sputum or change in color of sputum, pain with passing urine, mouth sores, or wound that will not heal.
- Signs of high blood sugar like confusion, feeling sleepy, more thirst, more hungry, passing urine more often, flushing, fast breathing, or breath that smells like fruit.
- Signs of low potassium levels like muscle pain or weakness, muscle cramps, or a heartbeat that does not feel normal.
- Signs of a weak adrenal gland like a very bad upset stomach or throwing up, very bad dizziness or passing out, muscle weakness, feeling very tired, mood changes, not hungry, or weight loss.
- Chest pain or pressure or a fast heartbeat.
- Feeling nervous and excitable.
- Shakiness.
- Change in how you act.
- Change in eyesight.
- A burning, numbness, or tingling feeling that is not normal.
- Choking.
- Change in voice.
- Seizures.
- Bone pain.
- Very bad dizziness.
- Very bad headache.
- Not able to sleep.
- Feeling very tired or weak.
- Vaginal itching or discharge.
- Weight gain.
- Mouth irritation or mouth sores.
- Redness or white patches in mouth or throat.
- This medicine can cause very bad breathing problems right after you take a dose. Sometimes, this may be life-threatening. If you have trouble breathing, breathing that is worse, wheezing, or coughing after using fluticasone and salmeterol inhaler, use a rescue inhaler and get medical help right away.
Fluticasone and Salmeterol Inhaler?
All drugs may cause side effects. However, many people have no side effects or only have minor side effects. Call your doctor or get medical help if any of these side effects or any other side effects bother you or do not go away:
- Headache.
- Upset stomach or throwing up.
- Throat irritation.
- Store at room temperature.
- Store with the mouthpiece down.
- Protect from heat or open flame. Do not puncture or burn even if it seems empty.
- Store in a dry place. Do not store in a bathroom.
- Keep all drugs in a safe place. Keep all drugs out of the reach of children and pets.
- Check with your pharmacist about how to throw out unused drugs.
Consumer Information Use and Disclaimer
- If your symptoms or health problems do not get better or if they become worse, call your doctor.
- Do not share your drugs with others and do not take anyone else’s drugs.
- Keep a list of all your drugs (prescription, natural products, vitamins, OTC) with you. Give this list to your doctor.
- Talk with the doctor before starting any new drug, including prescription or OTC, natural products, or vitamins.
- This medicine comes with an extra patient fact sheet called a Medication Guide. Read it with care. Read it again each time this medicine is refilled. If you have any questions about fluticasone and salmeterol inhaler, please talk with the doctor, pharmacist, or other health care provider.
- If you think there has been an overdose, call your poison control center or get medical care right away. Be ready to tell or show what was taken, how much, and when it happened.
This information should not be used to decide whether or not to take this medicine or any other medicine. Only the healthcare provider has the knowledge and training to decide which medicines are right for a specific patient. This information does not endorse any medicine as safe, effective, or approved for treating any patient or health condition. This is only a brief summary of general information about fluticasone and salmeterol inhaler. It does NOT include all information about the possible uses, directions, warnings, precautions, interactions, adverse effects, or risks that may apply to this medicine. This information is not specific medical advice and does not replace information you receive from the healthcare provider. You must talk with the healthcare provider for complete information about the risks and benefits of using fluticasone and salmeterol inhaler.
For more information visit us our website: https://www.healthinfi.com


Comments (2)