Allergy to Natural Rubber (Latex)And What is latex allergy?
Latex is natural rubber, a product made primarily from the rubber tree, Hevea brasiliensis. Some people develop allergic reactions after repeated contact with latex, especially latex gloves. Allergy to latex is an increasing health problem.
Natural rubber latex comes from the sap of the rubber tree, Hevea brasiliensis, found in Africa and Southeast Asia. Allergic reactions to products made with latex develop in persons who become allergic (or sensitized) to proteins contained in natural rubber latex. Natural rubber latex should not be confused with synthetic rubber made from chemicals. Synthetic rubber products, including “latex” house paints, are not made with natural latex and do not trigger allergic reactions in people who are allergic to products made with natural rubber latex.
Latex is a common component of many medical and dental supplies. These include disposable gloves, dental dams, airway and intravenous tubing, syringes, stethoscopes, catheters, dressings and bandages. Latex also is found in many consumer products. These include condoms, handbags, balloons, athletic shoes, tires, tools, underwear leg and waistbands, rubber toys, baby bottles, nipples and pacifiers.
Natural rubber latex (NRL) is a ubiquitous allergen as it is a component of > 40,000 products in everyday life. Latex allergy might be attributed to skin contact or inhalation of latex particles. Latex allergy is an IgE-mediated hypersensitivity to NRL, presenting a wide range of clinical symptoms such as angioedema, swelling, cough, asthma, and anaphylactic reactions. Until 1979, latex allergy appeared only as type IV delayed hypersensitivity; subsequently, the proportion of different allergy types drifted towards type IV contact allergy reactions.
Several risk factors for sensitization to NRL are already known and well documented. Some authors have established a positive correlation between a history of multiple surgical interventions, atopy, spina bifida malformation, and latex allergy incidence. We suspect an increase in latex allergy incidence in association with increased atopy and sensitivity to environmental allergens in the industrial population.

It is often postulated in literature that the groups of workers at risk for this allergy are essentially workers in the latex industry and healthcare professionals. In this population, direct internal and mucosal contact with NRL medical devices may be the route of sensitization as factors such as the number of procedures and use of NRL materials (catheters and tubes) were associated with increased risk of latex sensitization and allergy.
Allergies to latex rubber have only been recognised in the last few decades. The reasons are uncertain, although increased use of latex gloves in health care settings like hospitals and changes in manufacturing practices (due to increased demand) are probable contributors.
Latex is a milky fluid produced by rubber trees (Hevea brasiliensis). Using different methods, latex can be processed into a variety of products, such as gloves and balloons. During manufacturing, chemicals are added to increase the speed of curing (vulcanization) and to protect the rubber from oxygen in the air.
Products made from blends of natural rubber latex and other compounds are very common. In those with latex allergy, allergic reactions are most often triggered by dipped latex products. Products that commonly cause reactions can include gloves, balloons and condoms.
In rare instances, people who are allergic to latex may also react to rubber bands, erasers, rubber parts of toys, various rubber components in medical devices, rubber elastic in clothes, or feeding nipples and pacifiers. Products molded from hard, crepe rubber, such as soles of shoes, are unlikely to cause reactions. Almost all latex paints are not a problem since they do not contain natural rubber latex.
What are the symptoms?
Latex reactions can vary from minor to life-threatening, or they may progress from a less serious reaction to a more serious one. Examples include:
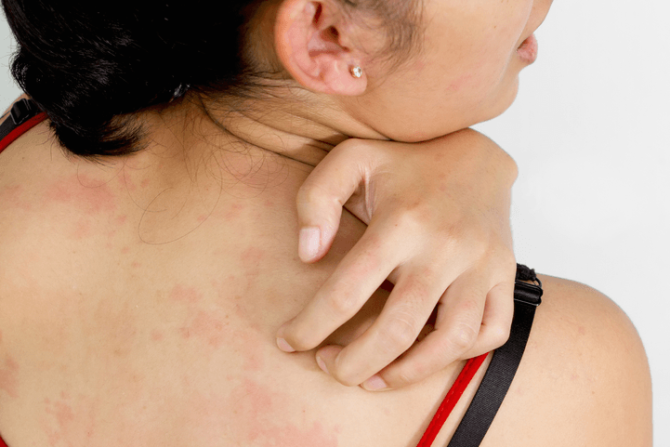
Skin reactions such as contact dermatitis, hives, or generalized itching.
- Respiratory reactions. A person who is having a mild respiratory reaction may sneeze, cough, or have a runny nose. A person who is having a severe respiratory reaction may develop shortness of breath from swelling of the throat (angioedema) or severe wheezing (allergic asthma).
- Life-threatening allergic reactions (anaphylaxis). For more information, see the Check Your Symptoms section of the topic Allergic Reaction.
In most cases, latex allergy develops after many previous exposures to latex. Latex allergy symptoms may include hives, itching, stuffy or runny nose. It can cause asthma symptoms of wheezing, chest tightness and difficulty breathing. Symptoms begin within minutes after exposure to latex containing products. The most severe latex allergy can result in anaphylaxis, a serious allergic reaction involving severe breathing difficulty and/or fall in blood pressure (shock).
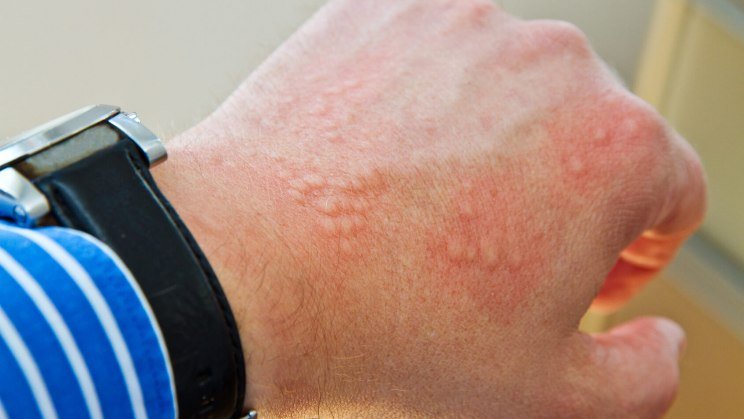
Allergic skin problems can occur following direct contact with allergic latex proteins in latex glove products. Symptoms may include immediate itching, redness and swelling of skin that touched the item containing latex. These and other latex allergic reactions are less common now. Many hospitals or doctors’ offices have switched to non-latex gloves or low protein latex gloves.
A second type of skin allergy called “allergic contact dermatitis” may be caused by chemicals used to manufacture rubber gloves. This dermatitis is recognized by the eczema and blisters on the back of the hands. It resembles a poison ivy rash, and begins 1 to 3 days after wearing rubber gloves.
Direct physical contact with latex products is not needed to trigger an allergic reaction. Anaphylaxis and severe asthmatic reactions have been caused by inhaling latex proteins in the air resulting from the powder in the latex glove.
Latex allergy often begins with a rash on the hands when using natural rubber latex gloves. Other allergic symptoms include hay fever type reactions such as itchy swollen eyes, runny nose, and sneezing. Some patients may develop asthma symptoms such as chest tightness, wheezing, coughing and shortness of breath.
However, people that have skin problems on their hands from glove use are not necessarily latex allergic.
Who is affected by latex allergy?
Latex allergy usually affects people who are routinely exposed to rubber products, such as health care workers and rubber industry workers, and people who have had multiple surgeries or multiple medical procedures in which latex equipment and supplies were used.
Other than healthcare workers, people at increased risk of developing latex allergy include those who have:
- A defect in their bone marrow cells
- A deformed bladder or urinary tract
- A history of multiple operations
- A urinary catheter, which has a rubber tip
- Allergy, asthma or eczema
- Food allergies to bananas, avocados, kiwi fruit or chestnuts
What increases the risk of latex allergy?
People who have allergies to foods, such as bananas, chestnuts, kiwifruit, avocados, and tomatoes, have an increased risk of developing latex allergy. People with latex allergies may develop allergies to these foods because the protein in these foods is similar to the protein in rubber. Latex allergies are also more common in people who have a history of atopic dermatitis, a skin condition that causes intense itching and a red, raised rash.
Most people who are allergic to latex have had frequent exposure to latex over many years. The majority are nurses, doctors, dentists, or patients who have had a number of operations, such as those with spina bifida. Many are also allergic to other substances such as grass pollen or dust mite proteins. In other words, they usually already have other allergic disease such as asthma, allergic rhinitis (hay fever) or eczema.
What foods are potential problems for people with latex allergy?
If you have latex allergy you also can have food allergies. The foods most likely to cause this problem include: apple, avocado, banana, carrot, celery, chestnut, kiwi, melons, papaya, raw potato and tomato.
How is latex allergy diagnosed?
A latex allergy is diagnosed in people who:
- Have experienced signs or symptoms of allergic reaction (skin rash, hives, watering eyes or irritation, wheezing, itching, difficulty breathing) when exposed to latex or natural rubber products.
- Do not have signs or symptoms of latex allergy but are known to be at risk of latex allergy and have a positive blood or skin test for latex allergy.
- Skin testing for latex allergy should only be done with the close supervision of an allergy specialist because of the risk of severe reactions.
Your doctor will normally ask a series of questions that may help to identify the cause of your problem. This will often be followed by allergy testing to help confirm or exclude the presence of sensitivity to natural latex proteins or chemical preservatives.
What happens during a latex reaction?
There are three types of latex reactions:
Irritant contact dermatitis – The least threatening type of latex reaction, classified as a non-allergenic skin reaction. It usually occurs as a result of repeated exposure to chemicals in latex gloves and results in dryness, itching, burning, scaling and lesions of the skin.
Allergic contact dermatitis – A delayed reaction to additives used in latex processing, which results in the same type of reactions as irritant contact dermatitis – dryness, itching, burning, scaling and lesions of the skin – but the reaction is more severe, spreads to more parts of the body and lasts longer.
Immediate allergic reaction (latex hypersensitivity) – The most serious reaction to latex, it can show up as rhinitis with hayfever-like symptoms, conjunctivitis, cramps, hives and severe itching. It is rare, but symptoms may progress to include a rapid heart rate, tremors, chest pain, difficulty breathing, low blood pressure, anaphylactic shock, and potentially, death.
If you experience severe symptoms, seek medical advice immediately, or go to the nearest Accident and Emergency department.
How do people get exposed?
Routes of exposure include:
- Through the skin – as may occur when latex gloves are worn
- Through mucous membranes such as the eyes, mouth, vagina, and rectum
- Through inhalation – rubber gloves contain a powder that can be inhaled
- Through the blood – as may occur when some medical devices containing rubber are used
What causes latex allergy?
The exact cause of latex allergy is unknown, but it is thought that repeated exposure to latex and rubber products may induce symptoms.
About 5% to 10% of healthcare workers have some form of allergy to latex.
Latex is used in a large number of products
Latex or natural rubber is the substance obtained from the sap of the Hevea brasiliensis tree. After the addition of preservatives and stabilisers, it is dipped into a mould, then heated and dried. During manufacturing, chemicals are added to render latex elastic and stable to heat by vulcanisation (heating in the presence of sulfur). Further chemicals are added for strength and durability, including mercaptobenzothiazole, thiurams and carbamates. Sometimes a dry powder lubricant (usually corn-starch) is added to the surface of the latex to prevent the rubber surfaces from sticking together.
Allergic reactions can occur to latex protein as well as the chemicals added to it, but not to cornstarch itself. However, when gloves are worn, latex protein can be leached from the glove and stick to the cornstarch particles. When gloves are changed, these particles can become airborne and spread latex allergen into the local environment.
Many commercial products contain natural rubber latex. These include bandages, baby bottle teats, baby dummies, rubber bands, clothing elastic, rubber toys, rubber grips and a wide range of medical equipment. Allergic reactions usually occur after exposure to dipped products like gloves, balloons and condoms. Products made from crepe rubber (like shoe soles) are unlikely to cause allergic reactions.
By contrast to natural latex rubber, synthetic rubber is produced from petrochemicals, and does not contain allergenic latex proteins. Products containing synthetic rubber (like most latex paints) do not cause allergic reactions.
Immediate allergic reactions to latex are most serious
Immediate allergic reactions (also known as Type 1 or IgE antibody mediated) are the most serious adverse reactions to latex. In people who have developed sensitivity to natural latex proteins, contact with latex releases the histamine into the tissues. The result is itching and hives (urticaria) with direct contact, like after wearing rubber gloves, or itchy swollen lips, face or tongue after blowing up balloons. Some people will develop irritation after wearing a condom, inserting a diaphragm for contraceptive purposes or after visiting the dentist or hairdresser and coming into contact with latex.
Reactions can also occur when latex is inhaled, resulting in allergic rhinitis (hay fever) or asthma like symptoms. This occurs most commonly in hospitals. The latex proteins can leach out of the gloves with sweaty hands and become attached to the powdered lubricant. In environments where gloves are being changed frequently, latex on these fine particles can become suspended in the air like pollen.
Anaphylaxis is the most serious allergic reaction to latex and typically occurs in very sensitive patients where latex protein is absorbed rapidly via moist surfaces such as the mouth, nose, throat, vagina, rectum or internally (such as during a surgical operation). Severe difficulty in breathing, a drop in blood pressure and anaphylactic shock may occur.
Irritant Dermatitis is the most common adverse reaction to latex
Most adverse reactions to latex are Irritant Dermatitis, which is not an immediate (true) allergic reaction and does not involve the immune system. It results in rough, dry and scaly skin, sometimes with weeping sores. It is made worse by sweating and friction under rubber gloves, but can also occur from frequent hand washing with harsh soaps.
Even though irritant dermatitis is not an allergic reaction, absorption of latex through damaged skin increases the risk of developing latex allergy with ongoing exposure. Recognition and treatment of this condition is therefore recommended to reduce the risk of developing latex allergy.
Allergic contact dermatitis is a common immune reaction to latex
Allergic Contact Dermatitis is the most common immune reaction to latex. The symptoms look similar to irritant dermatitis symptoms, but the cause is different. The rash is rough, dry and scaly, sometimes with weeping sores. It typically occurs 12-48 hours after contact with latex rubber. Contact Allergic Dermatitis is usually due to an inflammatory reaction to the chemicals added to rubber during manufacture, although there is now evidence that delayed contact dermatitis may also result from contact with latex protein as well.
Contact Allergic Dermatitis is annoying but not dangerous. As with irritant dermatitis, treatment is recommended to reduce the risk of developing more serious immediate allergic reactions to latex.
Measures should be taken if your job involves exposure to latex
If you are latex allergic and your job involves frequent exposure to latex, you should:
- Use latex free gloves yourself
- Request that non-powdered latex gloves be supplied to others in your area of work. This reduces airborne latex particle exposure, and has been shown to dramatically reduce the risk of developing latex allergy in occupational settings.
- Look after your hands and have any irritation or rash evaluated by a doctor. An intact skin barrier reduces the risk of developing latex allergy.
- It is important to note that avoiding any contact with latex is also an effective method of preventing latex allergy, particularly applicable for non-medical use such as food handlers and hairdressers.
Management of latex allergy involves careful avoidance
If you are latex allergic you should:
- Avoid latex in all its forms, and particularly avoid latex coming near your skin, face, eyes, nose or throat. Latex substitutes exist and can be used if required.
- Be aware that some condoms and diaphragms used for contraception contain latex and should be avoided. Latex-free condoms are now available from stores and websites.
- Wear a medical identifications bracelet, stating you are allergic to latex. If you are unconscious or confused and need emergency treatment, then the nurses and doctors will be made aware of this.
- Carry your own supply of non-latex gloves (such as vinyl or synthetic rubber), in case of an emergency.
- Advise doctors and dentists well in advance of any surgical operation, dental treatment, Pap smear, blood tests or x-ray to ensure that latex is not used.6. If it is necessary to wear gloves, use vinyl or synthetic rubber gloves.
- Avoid takeaway food which is prepared or served by food handlers wearing latex gloves.
- Consider avoiding occupations where latex is very difficult to avoid such as nursing, dentistry, medicine, veterinary science, hairdressing or food preparation.
Prevalence
Certain groups of individuals who are frequently exposed to latex are at high risk for developing immediate allergic reactions. Individuals with spina bifida (a congenital problem in the development of the back) and those with congenital urinary tract problems who need multiple surgeries seem to have a risk of nearly 50%. Health care workers and others whose jobs require wearing latex gloves or working around them have a risk of about 10%. Others who may be at increased risk are those who have had many medical or surgical procedures, resulting in repeated exposure to latex gloves. Rubber industry workers also are at increased risk. Even in normal adults, the risk of sensitization to latex may be as high as 6%.
People with latex allergy may also experience an allergic reaction to some foods that contain some of the same allergenic proteins as those in latex. This reaction, called cross-reactivity, can be triggered by bananas, avocados, kiwi fruit, and European chestnuts.
Evaluation and treatment
The first step in treating latex allergy is awareness of the problem. Visit your allergist/immunologist if you think you may have symptoms of latex allergy. After taking a detailed history and examining you, your doctor will decide whether additional diagnostic tests for latex allergy are needed. If you are allergic to latex, you should avoid contact with natural rubber latex products as much as possible. Inform your family, health care professionals, employer and school personnel about your allergy. Discuss with your physician whether you should wear a special bracelet or necklace that notifies others of your allergy. Your doctor will also determine whether you should carry injectable adrenalin (epinephrine) to provide immediate, emergency treatment in case you experience a severe allergic reaction.
If you have reactions to latex, see an allergist/immunologist. The 1990 Americans with Disabilities Act (ADA) covers people with severe allergies to substances such as latex. If you are otherwise qualified but can no longer work with latex in a job setting because of your allergy, work with your employer to determine other options and make reasonable accommodations. If you are allergic and need to wear gloves, or are in contact with persons wearing gloves, there are several options.
You may try substituting synthetic (vinyl or nitrile) gloves for latex gloves, although they may not work as well in some situations. These work in nearly all situations where latex gloves work, including surgery, but in some cases, they are more expensive. For individuals with contact dermatitis reactions to latex, latex gloves made without additional chemicals may work.
If you have significant latex allergy respiratory symptoms from inhaling latex particles, you need to avoid areas where powdered gloves are used frequently. Ideally, all high glove use areas should use powder-free gloves to avoid allergic reactions. Using latex condoms can be a severe problem for some latex-allergic people. One option is natural skin condoms. These do not contain latex and can prevent pregnancy, but they do not protect against viruses like HIV, which cause AIDS, or some other sexually-transmitted diseases (STDs). Synthetic rubber condoms, created to prevent both pregnancy and STDs, are now available.
Manufacturers are currently working to produce latex products that contain less latex allergen. As these products become more available, the risk of reactions in people sensitive to latex, as well as the risk of more people developing latex allergy, should decrease.
Your allergist/immunologist can provide you with more information on latex allergy.
Can a latex allergy be life-threatening?
While it is uncommon, some latex allergic individuals can suffer a potentially life-threatening allergic reaction when they come in contact with natural rubber latex.
This serious reaction is called anaphylactic shock. It occurs within minutes of exposure, and is characterized by generalized hives, breathing difficulties and low blood pressure. Anaphylactic shock may be fatal and must be promptly treated by adrenalin injection.
Anaphylactic shock is most likely to occur during direct tissue contact with natural rubber latex products. Direct contact occurs when the skin barrier which protects you has been broken, or the contact is across a mucous membrane. Mucous membrane contact can occur in the mouth (e.g. blowing up a balloon, dental surgery, anesthetic administration), vagina (condom use, vaginal examination), rectum and colon (examination or enema administration), or urethra (catheterization). Direct tissue contact occurs during surgery because surgeons normally wear natural rubber latex gloves when operating on a patient.
What precautions should allergic patients take?
Latex allergic patients take certain precautions to prevent future allergic reactions:
- Patients who are only mildly sensitive to latex products should observe the following precautions:
- Avoid contact with natural rubber latex products such as those listed in Table A Non-latex substitutes are available for most commonly used natural products.
- Before visiting doctors or dentists for any examination or procedure, warn them of your allergy to latex. Ask to be scheduled as the first patient in the day in order to minimize your exposure to airborne latex particles. Allergy causing latex dust is put into the air when staff put on and take off powdered natural rubber latex gloves. Dust from non-latex gloves will not cause an allergic reaction, since it is the latex (not the powder) which is allergenic.
- If you work in high latex exposure areas and have skin irritation, hay fever or asthma symptoms, you must advise the employee health department and consult a physician about your treatment. You may only be able to work in that environment if your symptoms are minimal or if your co-workers change to non-latex or powderless natural rubber latex gloves.
- You should consult with your physician about medicine you can take to reduce allergy symptoms.
- You should be aware that some latex allergic people also have certain food allergies. Foods so far associated with latex include bananas, avocados, and chestnuts. If any of these foods give you symptoms such as itching around the mouth, local swelling, hives or shortness of breath, you should avoid them.
- Patients who are very sensitive to latex – for example, react even when briefly in contact with a balloon or glove – should take the following additional precautions:
- Obtain and wear a Medic Alert bracelet printed with severe allergy to natural rubber latex.
When traveling to areas where medical supplies are limited, carry with you a variety of sizes of non-latex sterile gloves, in case you should need emergency medical or dental work. Non-latex sterile gloves are a specialty item that should be obtained in advance of traveling to these regions. Consult your doctor or hospital.
- Be familiar with the proper use of the self-administration of epinephrine (adrenalin). The indications and proper use of this should be explained by your physician.
- Prior to surgery you should consult your physician about the need for a latex-free operating environment.
For more information visit us our website: https://www.healthinfi.com
0 200
1 Comment