Anterior Cruciate Ligament (ACL) Tear
The bone structure of the knee joint is formed by the femur, the tibia, and the patella. The ACL is one of the four main ligaments within the knee that connect the femur to the tibia. The knee is essentially a hinged joint that is held together by the medial collateral (MCL), lateral collateral (LCL), anterior cruciate (ACL) and posterior cruciate (PCL) ligaments. The ACL runs diagonally in the middle of the knee, preventing the tibia from sliding out in front of the femur, as well as providing rotational stability to the knee.
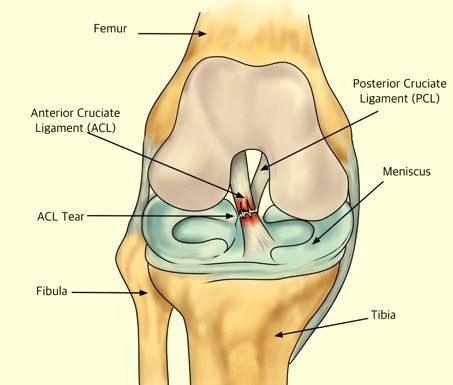
The weight-bearing surface of the knee is covered by a layer of articular cartilage. On either side of the joint, between the cartilage surfaces of the femur and tibia, are the medial meniscus and lateral meniscus. The menisci act as shock absorbers and work with the cartilage to reduce the stresses between the tibia and the femur.
One of the most common knee injuries is an anterior cruciate ligament sprain or tear.
Athletes who participate in high demand sports like soccer, football, and basketball are more likely to injure their anterior cruciate ligaments.
If you have injured your anterior cruciate ligament, you may require surgery to regain full function of your knee. This will depend on several factors, such as the severity of your injury and your activity level.
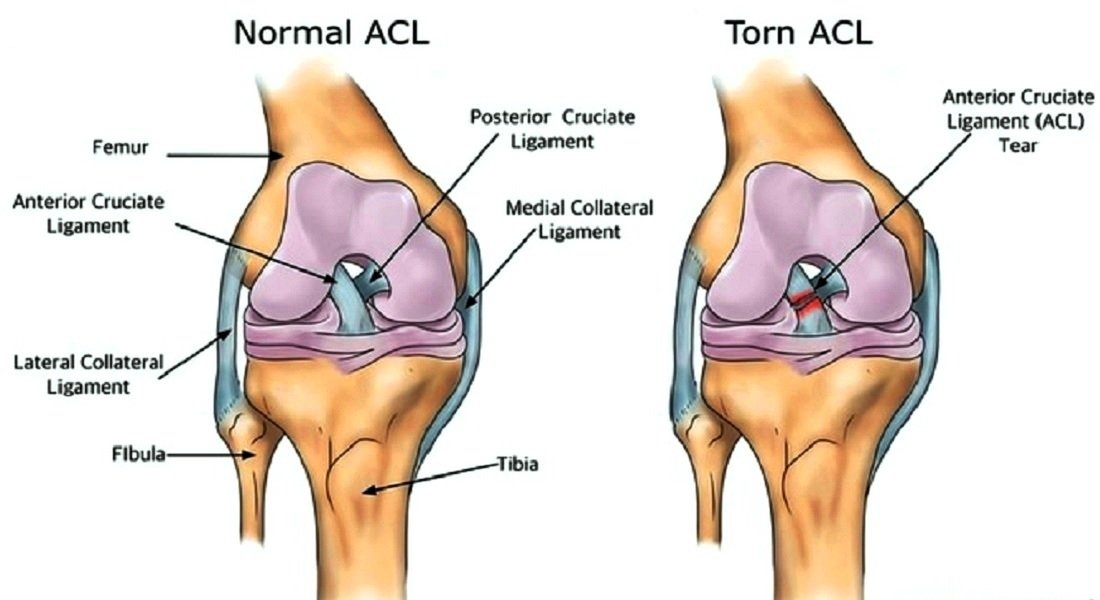
An ACL injury is the tearing of the anterior cruciate (KROO-she-ate) ligament (ACL) — one of the major ligaments in your knee. ACL injuries most commonly occur during sports that involve sudden stops, jumping or changes in direction — such as basketball, soccer, football, tennis, downhill skiing, volleyball and gymnastics.
Many people hear or feel a “pop” in the knee when an ACL injury occurs. Your knee may swell, feel unstable and become too painful to bear weight.
Depending on the severity of your ACL injury, treatment may include rest and rehabilitation exercises to help you regain strength and stability or surgery to replace the torn ligament followed by rehabilitation. A proper training program may help reduce the risk of an ACL injury.
One of the most common problems involving the knee joint is an anterior cruciate ligament injury or ACL tear. Of the four major knee ligaments of the knee, an ACL injury or rupture is the most debilitating knee ligament injury.
ACL injury usually occurs when the knee is hyperextended (straightened) and a pivot occurs simultaneously. The injury may occur with or without contact.
Women have an increased risk of ACL injury because of differences in anatomy, muscle mass, and training.
Symptoms of ACL tear include hearing a loud pop as the ligament tears, pain, knee swelling, and difficulty walking.
Diagnosis is made clinically by physical examination and usually confirmed by MRI.
Surgery with rehabilitation is the most commonly suggested treatment. In patients who are elderly, sedentary, or do little sports activity, a nonoperative treatment approach is a possibility.
Postoperative rehabilitation may take six to nine months to return to full activity.
A torn anterior cruciate ligament (ACL) is a second- or third-degree sprain of the ACL. The ACL arises from the front of the medial femoral condyle and passes through the middle of the knee to attach between the bony outcroppings (called the tibia spine) that are located between the tibia plateaus. It is a small structure, less than 1½ inches long and ½ inch wide. The anterior cruciate ligament is vital in preventing the thighbone (femur) from sliding backward on the tibia (or, from the other point of view, the tibia sliding forward under the femur). The ACL also stabilizes the knee from rotating, the motion that occurs when the foot is planted and the leg pivots.
Without a normal ACL, the knee becomes unstable and can buckle, especially when the leg is planted and attempts are made to stop or turn quickly.
Cause
It is estimated that the majority of ACL injuries occur through non-contact mechanisms, while a smaller percent result from direct contact with another player or object.
The mechanism of injury is often associated with deceleration coupled with cutting, pivoting or sidestepping maneuvers, awkward landings or “out of control” play.
Several studies have shown that female athletes have a higher incidence of ACL injury than male athletes in certain sports. It has been proposed that this is due to differences in physical conditioning, muscular strength, and neuromuscular control. Other hypothesized causes of this gender-related difference in ACL injury rates include pelvis and lower extremity (leg) alignment, increased ligamentous laxity, and the effects of estrogen on ligament properties.
Ligaments are strong bands of tissue that connect one bone to another. The ACL, one of two ligaments that cross in the middle of the knee, connects your thighbone (femur) to your shinbone (tibia) and helps stabilize your knee joint.
Most ACL injuries happen during sports and fitness activities that can put stress on the knee:
- Suddenly slowing down and changing direction (cutting)
- Pivoting with your foot firmly planted
- Landing from a jump incorrectly
- Stopping suddenly
- Receiving a direct blow to the knee or collision, such as a football tackle
- When the ligament is damaged, there is usually a partial or complete tear across the tissue. A mild injury may overextend the ligament but leave it intact.
- An ACL injury is usually a sports-related knee injury. About 80% of sports-related ACL tears are “non-contact” injuries. This means that the injury occurs without the contact of another player, such as a tackle in football.
- Most often ACL tears occur when pivoting or landing from a jump. Your knee gives out from under you once you tear your ACL.
Female athletes are known to have a higher risk of an ACL tear while participating in competitive sports. Unfortunately, understanding why women are more prone to ACL injury is unclear. There are some suggestions it is biomechanical, strength and hormonally related. In truth, it is probably a factor of all three.
Most anterior cruciate ligament injuries occur due to injury, usually in a sport or fitness activity. The ligament gets stretched or tears when the foot is firmly planted and the knee locks and twists or pivots at the same time. This commonly occurs in basketball, football, soccer, and gymnastics, where a sudden change in direction stresses and damages the ligament. These injuries are usually noncontact, occur at low speed, and occur as the body is decelerating.
ACL injuries may also occur when the tibia is pushed forward in relation to the femur. This is the mechanism of injury that occurs because of a fall when skiing, from a direct blow to the front of the knee (such as in football) when the foot is planted on the ground, or in a car accident.
Doctor Examination
Immediately after the injury, patients usually experience pain and swelling and the knee feels unstable. Within a few hours after a new ACL injury, patients often have a large amount of knee swelling, a loss of full range of motion, pain or tenderness along the joint line and discomfort while walking.
When a patient with an ACL injury is initially seen for evaluation in the clinic, the doctor may order x-rays to look for any possible fractures. He or she may also order a magnetic resonance imaging (MRI) scan to evaluate the ACL and to check for evidence of injury to other knee ligaments, meniscus cartilage, or articular cartilage.
In addition to performing special tests for identifying meniscus tears and injury to other ligaments of the knee, the physician will often perform the Lachman’s test to see if the ACL is intact.
If the ACL is torn, the examiner will feel increased forward (upward or anterior) movement of the tibia in relation to the femur (especially when compared to the normal leg) and a soft, mushy endpoint (because the ACL is torn) when this movement ends.
Natural History
What happens naturally with an ACL injury without surgical intervention varies from patient to patient and depends on the patient’s activity level, degree of injury and instability symptoms.
The prognosis for a partially torn ACL is often favorable, with the recovery and rehabilitation period usually at least 3 months. However, some patients with partial ACL tears may still have instability symptoms. Close clinical follow-up and a complete course of physical therapy helps identify those patients with unstable knees due to partial ACL tears.
Complete ACL ruptures have a much less favorable outcome without surgical intervention. After a complete ACL tear, some patients are unable to participate in cutting or pivoting-type sports, while others have instability during even normal activities, such as walking. There are some rare individuals who can participate in sports without any symptoms of instability. This variability is related to the severity of the original knee injury, as well as the physical demands of the patient.
About half of ACL injuries occur in combination with damage to the meniscus, articular cartilage or other ligaments. Secondary damage may occur in patients who have repeated episodes of instability due to ACL injury. With chronic instability, a large majority of patients will have meniscus damage when reassessed 10 or more years after the initial injury. Similarly, the prevalence of articular cartilage lesions increases in patients who have a 10-year-old ACL deficiency.
Symptoms
When you injure your anterior cruciate ligament, you might hear a “popping” noise and you may feel your knee give out from under you. Other typical symptoms include:
Pain with swelling. Within 24 hours, your knee will swell. If ignored, the swelling and pain may resolve on its own. However, if you attempt to return to sports, your knee will probably be unstable and you risk causing further damage to the cushioning cartilage (meniscus) of your knee.
- Loss of full range of motion
- Tenderness along the joint line
- Discomfort while walking
- A loud “pop” or a “popping” sensation in the knee
- Severe pain and inability to continue activity
- Swelling that begins within a few hours
- Loss of range of motion
- A feeling of instability or “giving way” with weight bearing
Risk factors for ACL injury in women
Women are more prone to ACL injuries than men. Women have slightly different anatomy that may put them at higher risk for ACL injuries:
The intercondylar notch at the end of the femur is narrower in women than men. When the knee moves, this narrower space can pinch and weaken the ACL.
Women have a wider pelvis than men, and this causes the femur to meet the tibia at a greater angle (called the Q angle). This increases the force that the ACL has to withstand with any twisting motion, increasing the risk of damage.
Genetic differences may put the female ACL at risk. Female muscles tend to be more elastic and decrease the protection that the hamstring muscles can provide to the ACL. Hormonal changes during menses may also affect elasticity. Moreover, female hamstrings react and contract a millisecond slower than in a male, increasing the risk of ACL damage when landing from a jump.
Women are more likely to have an ACL injury than are men who participate in the same sports. Studies have suggested some reasons for these differences in risk.
In general, women athletes exhibit a strength imbalance in their thighs with the muscles at the front of the thigh (quadriceps) being stronger than the muscles at the back (hamstrings). The hamstrings help prevent the shinbone from moving too far forward — movement that can overextend the ACL.
Studies comparing jumping and landing techniques among men and women athletes have shown that women athletes are more likely to land from a jump in a way that increases stress on their knees.
Research suggests that training to strengthen muscles of the legs, hips and lower torso — as well as training to improve jumping and landing techniques — may reduce the higher ACL injury risk associated with women athletes.
- infection,
- persistent instability and pain,
- knee stiffness, and
- difficulty returning to your previous level of activity.
Treatment
Treatment for an ACL tear will vary depending upon the patient’s individual needs. For example, the young athlete involved in agility sports will most likely require surgery to safely return to sports. The less active, usually older, individual may be able to return to a quieter lifestyle without surgery.
Nonsurgical Treatment
A torn ACL will not heal without surgery. But nonsurgical treatment may be effective for patients who are elderly or have a very low activity level. If the overall stability of the knee is intact, your doctor may recommend simple, nonsurgical options.
Bracing. Your doctor may recommend a brace to protect your knee from instability. To further protect your knee, you may be given crutches to keep you from putting weight on your leg.
Physical therapy. As the swelling goes down, a careful rehabilitation program is started. Specific exercises will restore function to your knee and strengthen the leg muscles that support it.
Surgical Treatment
Rebuilding the ligament. Most ACL tears cannot be sutured (stitched) back together. To surgically repair the ACL and restore knee stability, the ligament must be reconstructed. Your doctor will replace your torn ligament with a tissue graft. This graft acts as a scaffolding for a new ligament to grow on.
Grafts can be obtained from several sources. Often they are taken from the patellar tendon, which runs between the kneecap and the shinbone. Hamstring tendons at the back of the thigh are a common source of grafts. Sometimes a quadriceps tendon, which runs from the kneecap into the thigh, is used. Finally, cadaver graft (allograft) can be used.
There are advantages and disadvantages to all graft sources. You should discuss graft choices with your own orthopaedic surgeon to help determine which is best for you.
Because the regrowth takes time, it may be six months or more before an athlete can return to sports after surgery.
Procedure. Surgery to rebuild an anterior cruciate ligament is done with an arthroscope using small incisions. Arthroscopic surgery is less invasive. The benefits of less invasive techniques include less pain from surgery, less time spent in the hospital, and quicker recovery times.
Prevention
Proper training and exercise can help reduce the risk of ACL injury. A physical therapist, athletic trainer or other specialist in sports medicine can provide assessment, instruction and feedback that can help you reduce risks. Programs to reduce ACL injury include:
- Exercises that strengthen leg muscles, particularly hamstring exercises, to ensure an overall balance in leg muscle strength
- Exercises to strengthen the core: hips, pelvis and lower abdomen
- Training and exercise for proper techniques and knee position in jumping and landing
- Training to improve techniques for pivoting and cutting
What tests do health-care professionals use to diagnose a torn ACL?
The diagnosis of an ACL injury begins with the care provider taking a history of how the injury occurred. Often the patient can describe in detail their body and leg position and the sequence of events just before, during, and after the injury as well as the angle of any impact.
Physical examination
Physical examination of the knee usually follows a relatively standard pattern.
- The knee is examined for obvious swelling, bruising, and deformity.
- Areas of tenderness and subtle evidence of knee joint fluid (effusion) are noted.
Most importantly, with knee injury ligamentous, stability is assessed. Since there are four ligaments at risk for injury, the examiner may try to test each to determine which one(s) is (are) potentially damaged. It is important to remember that a knee ligament injury might be an isolated structure damaged or there may be more than one ligament and other structures in the knee that are hurt.
In the acute situation, with a painful, swollen joint, the initial examination may be difficult because both the pain and the fluid limit the patient’s ability to cooperate and relax the leg. Spasm of the quadriceps and hamstring muscles often can make it difficult to assess ACL stability.
A variety of maneuvers can be used to test the stability and strength of the ACL. These include the Lachman test, the pivot-shift test, and the anterior drawer test. Guidelines from the American Academy of Pediatrics suggest the Lachman test is best for assessing ACL tears.
The Bachmann test is performed as follows:
- The damaged knee is flexed to 20-30 degrees.
- The examiner grasps tibia and puts their thumb on the tibial tubercle (the bump of bone just below the knee where the patellar tendon attaches.
- The examiners other hand grasps the thigh just above the knee.
- The tibia is pulled forward and normally, there should be a firm stop if the ACL is intact. If the ligament is torn, the tibia will move forward and there will be no endpoint and it feels mushy.
- The unaffected knee may be examined to be used as comparison.
- It may be difficult to examine some patients when muscle strength or spasm can hide an injured ACL because of the knee stabilization that they can provide.
Knee imaging
Plain X-rays of the knee may be done looking for broken bones. Other injuries that may mimic a torn ACL include fractures of the tibial plateau or tibial spines, where the ACL attaches. This second situation is often seen in children with knee injuries, where the ligament fibers are stronger than the bones to which they are attached. In patients with an ACL tear, the X-rays are often normal.
Magnetic resonance imaging (MRI) has become the test of choice to image the knee looking for ligament injury. In addition to defining the injury, it can help the orthopedic surgeon help decide the best treatment options. However, MRI does not replace physical examination and many knee injuries do not require an MRI to confirm the diagnosis.
Gear
Wear footwear and padding that is appropriate for your sport to help prevent injury. If you downhill ski, make sure your ski bindings are adjusted correctly by a trained professional so that your skis will release appropriately when you fall.
Wearing a knee brace does not appear to prevent ACL injury or reduce the risk of recurring injury after surgery.
Return to Sports with an ACL Injury
Athletes often have particular difficulty returning to their sport once they have sustained an ACL injury, even if they are surgically reconstructed.
- Researchers have found that your best chance of returning to your sports post-ACL tear is to have undertaken both:
- ACL reconstruction surgery, and
- Intensive post-operative physiotherapy rehabilitation.
For more information visit us our website: https://www.healthinfi.com
0 200

No Comments