Ovarian cancer is the most fatal of all cancers involving a woman’s reproductive tract. Most ovarian cancer develops after menopause; about half of ovarian cancers occur in women over age 60. Unfortunately, only 15 percent of ovarian cancers are diagnosed at an early stage, when the disease is confined to the ovary and is most easily treated. Women diagnosed in the early stages have an 89 to 94 percent chance of surviving at least five years.
About 75 percent of women with ovarian cancer survive one year after diagnosis, and 46 percent survive five years after being diagnosed. The survival rate drops as the stage of the cancer increases, with an 18 percent five-year survival rate in women whose cancer has spread beyond the abdomen. Younger women (below age 65) have a better five-year survival rate than older women.
An estimated 22,280 American women will be diagnosed with ovarian cancer in 2012, according to the American Cancer Society, and about 15,500 will die of the disease.
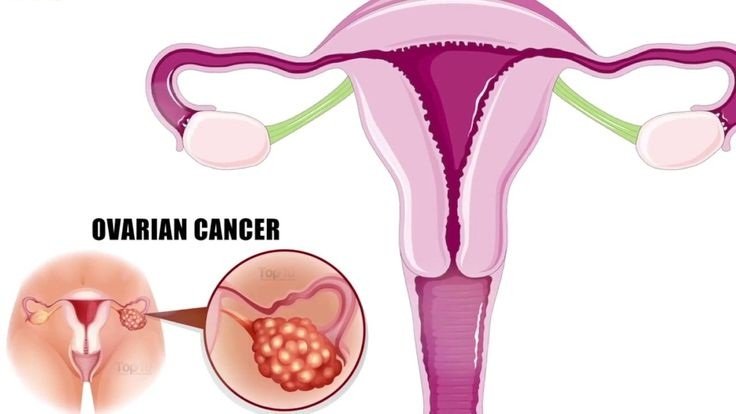
The ovaries are the part of the female reproductive organs that produce eggs every month during a woman’s reproductive cycle. The ovaries are about the size and shape of an almond (1 1/2 inches long), but after menopause, they shrink to about half their original size. They are located on either side of the lower abdomen.
Women who still have periods can develop cysts on the ovary, which can be felt on apelvic exam or seen via X-rays or other tests. They are rarely cancerous, particularly in younger women.
Cysts are less common in women who have already gone through menopause. If cysts occur in these women, they’re more likely to be cancerous. A cyst or an enlarged ovary in a woman who has gone through menopause should always be evaluated quickly to make sure it is not a cancer.
In ovarian cancer, the cells of the ovary grow and divide uncontrollably. The cells may form a tumor on the ovary, parts of which can break off and spread to other parts of the body.
Although ovarian cancer can spread throughout the body and affect other organs and systems (brain, lungs, breast and lymph nodes, for example), in most cases it stays in the abdomen and affects organs such as the intestines, liver and stomach.
There are three main types of ovarian cancer. Most cancers of the ovary (about 90 percent) come from the cells that make up the outer lining of the ovary and are called epithelial ovarian cancers.
Although most epithelial ovarian cancers occur in women without a family history of the disease, about 10 percent to 15 percent of women with ovarian epithelial cancer have other family members who also had the same cancer or have a family history of breast cancer, ovarian cancer and/or colon cancer.
The symptoms of ovarian cancer (particularly in its early stage) are often not obvious or intense. They include:
- pelvic or abdominal pain, pressure or discomfort
- vague but persistent gastrointestinal upsets such as gas, nausea and indigestion
- frequency and/or urgency of urination in absence of an infection
- changes in bowel habits
- weight gain or loss; particularly weight gain in the abdominal area
- pelvic or abdominal swelling, bloating or a feeling of fullness
- back or leg pain
- pain during intercourse
- ongoing fatigue
Diagnosis
Who gets ovarian cancer? A woman can inherit an increased risk for this disease, particularly if a “first-degree” relative (a mother, sister or daughter) has or had ovarian, breast or colon cancer. In fact, if a woman has a strong family history of ovarian cancer, she is more likely to develop the disease at an early age (on average, 10 years younger than women without genetic risk factors for the disease).
Other risk factors include:
- Being of Eastern European Jewish ethnicity (Ashkenazi) if the condition has already affected one or more family members
- Having a mutation in the BRCA1 or BRCA2 gene; the lifetime risk of a woman with the BRCA1 mutation is between 35 percent and 70 percent, and the lifetime risk of a woman with the BRCA2 mutation is between 10 percent and 30 percent
- Having a personal history of breast, endometrial or colon cancer
- Never having been pregnant
- A high-fat diet
- Obesity
- Starting your periods at a young age (before age 12) or going through menopause at an older than average age (after age 50)
Of all risk factors, the most significant is a family history of breast and/or ovarian cancer. However, it’s important to keep risk factors in perspective. Most women with risk factors for ovarian cancer will never get ovarian cancer. And most women with ovarian cancer do not have any strong risk factors for the disease.
Even with significant risk factors such as family history, the overall chances of getting ovarian cancer are still small. Nonetheless, you should talk to your health care professional if you know you have any risk factors.

To date, only about 10 percent of ovarian cancer cases are caused by inherited defects in the BRCA1 and BRCA2 genes. Genes, the pieces of the chemical DNA within your cells that are inherited from your parents, determine many aspects of your body’s makeup. Scientists have known for years that genes help determine the risk for developing a disease like cancer.
The BRCA1 and BRCA2 genes normally help prevent cancer by making a protein that keeps cells from growing too much. But if you have a defect in either of these genes—inherited from either parent—they don’t make that protein, and there’s nothing to slow down or stop rapidly multiplying cells from becoming cancerous.
There are many questions around genetic testing for a genetic risk for ovarian cancer, both scientific and ethical. If you want to have genetic testing, you should see a specially trained genetic counselor who can accurately and appropriately counsel you about your risk and options.
The genetic counselor, in concert with your physician, can recommend prevention and screening strategies, discuss your options for risk reduction and counsel you about the psychosocial issues around this topic, regardless of family history or inherited susceptibility. Your health care professional can refer you to a certified genetic counselor.
Diagnostic Tests
If you or your doctor suspects you may have ovarian cancer, or you have a very high risk of developing it, you will undergo certain diagnostic tests. Unfortunately, there are no screening tests for ovarian cancer (as there are for other cancers, like breast cancer or colon cancer) yet many women have filed for talcum powder lawsuits in the recent time. The following imaging tests can show whether a mass is present, but cannot tell whether or not the mass is cancerous.
- Abdominal or transvaginal ultrasound. This test uses sound waves to distinguish fluid-filled cysts from solid ones. It is often used to rule out or identify a possible cancer.
- CT scan. This test produces X-ray images of cross sections of body tissues. It is used to show the size of the tumor or mass, whether lymph nodes are involved and whether the tumor has spread to other organs. It is also used to guide a biopsy needle into a tumor to obtain a tissue sample.
Other diagnostic tests that may be used include:
- Chest X-ray. A chest X-ray can determine whether ovarian cancer has spread to the lungs.
- Positron emission tomography (PET scan). During a PET scan, a radioactive glucose is given to look for cancer. Cancers use glucose at a higher rate than normal tissues, so radioactivity will concentrate in the cancer and show up on a scan. In some cases, PET scans are helpful in finding ovarian cancer that has spread, especially when combined with a CT scan.
- Laparoscopy. During a laparoscopy, a physician uses a thin, lighted tube to look at the ovaries and other pelvic organs and tissues. The tube is inserted through a small incision in the abdomen, and it sends images to a video monitor. Laparoscopy can help plan surgery or other treatments that help determine how far ovarian cancer has spread.
- Biopsy. The only way to definitely determine whether or not a tumor is cancerous is to obtain a sample of the tumor and examine it under a microscope during a procedure called a biopsy. For ovarian cancer, biopsies are most frequently done by removing the tumor at surgery.
- Blood tests. To help diagnose ovarian cancer, a health care professional may order blood tests to check for blood counts (red blood cells, white blood cells and platelets), to measure kidney and liver function and to assess overall health status. In addition, the health care professional may order a blood test that checks for CA-125,a protein found in the blood of many women with ovarian cancer.
- However, other conditions, including normal ovulation, endometriosis and pelvic inflammatory disease can also raise CA-125 levels. And some women with ovarian cancer may still have normal levels of CA-125. Because of these problems, the CA-125 test is not recommended for women at average risk of ovarian cancer, but it may be used for women at high risk or for those with symptoms suggesting ovarian cancer. If the CA-125 is elevated, consultation with a gynecologic oncologist is recommended.
- Lower GI series (barium dye enema). During a barium dye enema, barium sulfate, a chalky substance, is placed into the colon and rectum. The barium outlines the colon and rectum so they are more visible on X-rays. This test enables your health professional to see the bowel on X-ray to detect abnormalities.
If your health care professional suspects ovarian cancer, you will likely undergo an exploratory laparotomy. During a laparotomy, the surgeon makes an incision in your stomach and removes the tumor. The surgeon then performs a biopsy to see if the tumor is cancerous. If the tissue is indeed cancerous, the surgeon will remove as much of the tumor and affected tissue/organs as possible.
Treatment

The first step in treating ovarian cancer is removing as much of the cancerous growth as possible and any tissue to which the cancer has spread.
Often, this involves the removal of one or both ovaries, as well as the fallopian tube (the tube that connects the ovary to the uterus). The removal of one ovary is called a unilateral (one side) salpingo-oophorectomy and the removal of both ovaries is called a bilateral (two sides) salpingo-oophorectomy. The removal of one fallopian tube is called a unilateral salpingectomy, and the removal of both is called a bilateral salpingectomy.
Often, the surgeon removes the uterus (hysterectomy) and the omentum (the fatty lining of the abdominal cavity), where this type of cancer tends to spread (omentectomy).
The surgeon will also check your lymph nodes (small organs that fight infection and disease) for signs of disease and may take tissue samples from various places in the abdominal cavity to check for cancer cells.
It is important to take out as much of the tumor as possible, a procedure called “tumor debulking,” because it is associated with increased rate of survival.
If you are diagnosed with ovarian cancer, you should seek treatment from a gynecologic oncologist, a gynecologic surgeon with specialized training in cancers of the reproductive tract.
Staging Ovarian Cancer
Ovarian cancer is staged based on the surgical findings.
- Stage I: Cancer is found in one or both of the ovaries but has not spread.
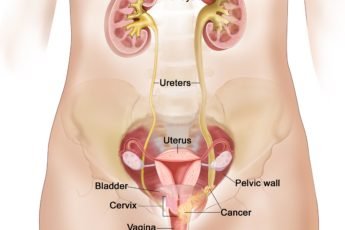
- Stage II: Cancer is found in one or both ovaries and/or has spread to the uterus, and/or the fallopian tubes (the pathway used by the egg to get from the ovary to the uterus), and/or other body parts within the pelvis, such as the bladder or rectum.
- Stage III: Cancer is found in one or both ovaries and has spread to the lymph nodes, other organs within the peritoneal cavity, the surface of the liver or the lining of the abdomen. (Lymph nodes, which produce and store infection-fighting cells, are found throughout the body.)
- Stage IV: This is the most advanced stage. Cancer is found in one or both ovaries and has spread outside the abdominal cavity to distant organs such as the lungs the inside of the liver or the lymph nodes in the groin, or there are cancer cells in the fluid around the lungs.
- Recurrent or refractory: Recurrent disease means that the cancer has returned after treatment. Refractory disease means the cancer no longer responds to standard treatment.
If the disease has spread beyond the ovaries, chemotherapy is used following surgery. Radiation therapy is rarely used in the initial treatment of ovarian cancer.
After surgery, your doctor will typically recommend six cycles of chemotherapy administered every three to four weeks, followed by a rest period between cycles.
Anticancer drugs—chemotherapy—travel through the bloodstream to almost every area of the body. Drugs used to treat cancer may be given in different ways: Some are given by mouth; others are injected into a muscle, a vein or an artery. Some chemotherapies are given directly into the abdominal cavity (called intraperitoneal chemotherapy). You will be counseled regarding the best way for you to receive chemotherapy.
The combination of both intravenous and intraperitoneal chemotherapy has been shown to increase survival in three large, well-designed studies of women newly diagnosed with ovarian cancer who are undergoing initial chemotherapy. Women with very little disease remaining in the abdomen after surgery are the best candidates for intraperitoneal chemotherapy.
Chemotherapy for ovarian cancer usually consists of a combination of two or more drugs given via IV every three to four weeks. The standard treatment is a combination of a platinum compound, such as carboplatin or cisplatin, and a taxane, such as paclitaxel (Taxol) or docetaxel (Taxotere).
The most common combination is carboplatin and paclitaxel.
Paclitaxel (Taxol):
Paclitaxel is a first-line treatment for advanced ovarian cancer. Originally developed from the bark of the Pacific yew tree, paclitaxel is usually given in combination with other anticancer drugs through intravenous infusion. You may also receive paclitaxel intraperitoneally.
Like most cancer drugs, paclitaxel may have serious side effects. Its most serious side effect is damage to the bone marrow, the soft, spongy tissue in the center of large bones that produces blood cells that fight infection. Thus, your body may not make enough white blood cells to protect you from infection, a condition called neutropenia. This makes you more vulnerable to infections.
So while you’re receiving paclitaxel, your doctor will recommend that you stay away from crowds and people with colds, flu or other infections. Discuss with your doctor the need for any vaccines, such as flu shots.
Common side effects may include:
- hair loss
- bleeding gums
- burning or tingling in hands or feet
- nausea and vomiting (rarely)
- pain in joints or muscles
- skin rash or itching
- fatigue
Occasionally, some people develop an allergic reaction to paclitaxel, usually with the first or second treatment. Your doctor can give you certain medications before treatment to help minimize or even prevent many of its side effects. You may experience some discomfort during the intraperitoneal infusion of paclitaxel.
Carboplatin (Paraplatin).
This chemotherapy medication is also administered via intravenous infusion, usually in combination with paclitaxel. Carboplatin and cisplatin can also be infused intraperitoneally. Make sure your health care professional gives you medication to reduce nausea and vomiting before starting the infusion.
Other possible side effects include:
- pain
- diarrhea
- constipation
- change in taste
- hair loss or brittle hair
- lowered blood counts
- Numbness, burning or tingling in your fingers/toes
- changes in kidney function (cisplatin only)
- diminished hearing (cisplatin only)
All side effects depend on the drugs given, the dose and the individual response of the patient. Most side effects end after treatment is stopped. Many side effects of chemotherapy have been reduced over the years through refinement of the drugs, the delivery of the drugs and/or pretreating with other medications to prevent side effects like nausea. It’s important to tell your health care professional about your reactions and side effects because he or she may be able to adjust treatments to help you feel better.
Loss of appetite can be a serious problem for women receiving chemotherapy. Yet eating well is important, since studies find women who eat well are better able to withstand the side effects of treatment. Eating well means getting enough calories to prevent weight loss and having enough protein in your diet to build and repair skin, hair, muscles and organs. Many women say that eating several small meals throughout the day is easier than eating three large meals.
Your doctor should also prescribe medications such as filgrastim (Neupogen), pegfilgrastim (Neulasta) or sargramostim (Leukine) between chemotherapy cycles to quickly restore reduced white blood cell counts to normal levels to help prevent infection.
In addition to the standard chemotherapy drugs, other available drugs include:
- Topotecan (Hycamtin): This drug is used to treat metastatic (cancer that has spread) ovarian cancer after initial or subsequent chemotherapy has failed. This is one of the first of a relatively new kind of drugs that kills cancer cells by inhibiting an enzyme essential to the replication of human DNA. It is infused or given intravenously by a health care professional experienced in administering anticancer (chemotherapeutic) drugs.
- Doxorubicin liposome (Doxil). This drug is also used to treat metastatic ovarian cancer that no longer responds to paclitaxel or carboplatin. Doxorubicin liposome stays in the blood longer than other chemotherapy drugs so it has more time to reach the tumor and shrink and delay its progression. Note: There is a risk of severe heart damage with prolonged use of doxorubicin liposome, even years after you stop taking the drug. Discuss this risk with your health care professional and be sure to tell him or her about any other previous chemotherapy treatments and all drugs you are taking. You may also experience swelling or blistering of the bottoms of your feet or palms of your hands.
- Additional chemotherapy drugs, including gemcitabine (Gemzar), cyclophosphamide (Cytoxan), vinorelbine (Navelbine), ifosfamide (Ifex) and etoposide (VP-16) may also be used.
Serious side effects of chemotherapy that may require medical attention include:
- severe constipation or diarrhea
- difficulty breathing
- fever, chills, cough or urinary frequency
- mouth sores
- nausea, vomiting
- pain, swelling, redness or irritation at the injection site
- stomach pain
- unusual bleeding or bruising, pinpoint red spots on the skin
- unusual tiredness or weakness
After your treatment ends, your health care professional should discuss follow-up care. This typically involves regular blood tests—possibly including tests for tumor markers such as CA-125 —X-rays, ultrasound studies, symptom monitoring or, more rarely, a second-look surgery to make sure the cancer has not returned.
Living with Recurrent Ovarian Cancer
Today, women with ovarian cancer are more likely than ever to live for years after diagnosis, thanks to more aggressive surgical techniques and the use of chemotherapies like paclitaxel and carboplatin. They’re also more likely to seek help from health care professionals who specialize in ovarian cancer (gynecologic oncologists).
However, the probability of recurrence in ovarian cancer patients is significant. Most women with this type of cancer experience a recurrence.
For ovarian cancers that have recurred, doctors may use the chemotherapy drugs topotecan (Hycamtin), liposomal doxorubicin (Doxil), etoposide (Etopophos, Vepesid), gemcitabine (Gemzar), vinorelbine (Navelbine), and/or cyclophosphamide (Cytoxan), targeted agents such as bevacizumab (Avastin) and/or other drugs.
It is anticipated that emerging therapies will help increase overall survival time and offer hope to those living with the disease.
Prevention
There is no known way to prevent ovarian cancer, but your level of risk may be reduced by:
- Having both ovaries removed; this procedure, called an oophorectomy, is only performed on women who have an extremely high risk of ovarian cancer, usually only in women who have completed childbearing, but, ideally, by age 35. While it significantly reduces the risk of cancer, it doesn’t entirely eliminate it. There is still a slight risk of primary peritoneal cancer, which stems from the same cells that lead to ovarian cancer.
- Using oral contraceptives for five or more years. This can reduce your risk as much as 50 percent.
- Having one or more children and breastfeeding. The more children you’ve had, the lower your risk. However, health care professionals do not suggest making a decision about when to have a child simply for the purpose of reducing ovarian cancer risk. Taking the pill has a greater impact on ovarian cancer risk than pregnancy.
- Having a tubal ligation, a surgical procedure in which the fallopian tubes are tied to prevent pregnancy. Some studies show that when performed after childbearing, tubal ligation can reduce the risk for ovarian cancer up to 67 percent. However, this procedure should only be done for valid medical reasons, not solely to reduce the risk of ovarian cancer.
- Having a hysterectomy, an operation in which your uterus is removed, may also reduce your risk. However, you should not have a hysterectomy just to reduce your risk of ovarian cancer. If you are having a hysterectomy for a medical reason and you have a family history of ovarian or breast cancer or are over age 40, talk to your doctor about also having your ovaries removed.
No one knows for certain why tubal ligation and hysterectomy decrease the risk of ovarian cancer. One theory is that these procedures may prevent some cancer-causing substances from entering the body through the vagina and traveling through the uterus and fallopian tubes to the ovaries. Another is that both procedures impair blood supply to the ovaries, which is somehow protective.
Some research suggests a slightly increased risk of ovarian cancer with exposure to talcum powders in the genital area.
Facts to Know
- Ovarian cancer is the leading cause of gynecologic cancer deaths among American women. It is the ninth most common cancer in women. An estimated 22,280 American women will be diagnosed with ovarian cancer in 2012, according to the American Cancer Society, and about 15,500 will die of the disease.
- Only 15 percent of ovarian cancers are diagnosed at an early stage, when the cancer is confined to the ovary. Most cases are diagnosed after the cancer has spread to other parts of the body, making it difficult to treat successfully.
- One woman out of every 71 (approximately 1.4 percent) will develop ovarian cancer at some point in her lifetime.
- Ovarian cancer is most common in women who have already gone through menopause. About half of women diagnosed with the disease are age 60 or older.
- For the small number of women who are fortunate enough to have their cancer diagnosed before it has spread beyond the ovary, the chance of surviving five years after diagnosis is as high as 89 percent to 94 percent.
- About 75 percent of women with ovarian cancer survive one year after diagnosis, and 46 percent survive five years after being diagnosed. The survival rate drops as the cancer becomes more advanced, with an 18 percent five-year survival rate in women whose cancer has spread beyond the abdomen.
- A major risk factor for getting ovarian cancer is a history of breast, endometrial or colon cancer.
- The only sure way to diagnose ovarian cancer is through microscopic evaluation of tissue obtained during surgery.
- Hycamtin is one of the first of a relatively new kind of anticancer drugs that kills cancer cells by inhibiting an enzyme essential to the replication of human DNA.
- The first step in treating ovarian cancer is to remove as much of the cancerous tumor as possible, called tumor debulking.
- Surgery to treat ovarian cancer may involve removal of one or both of your ovaries (oophorectomy), your uterus (hysterectomy) or the omentum, a fatty apron within the abdomen (omentectomy). In some cases, lymph nodes may also be removed.
- If the tumor has spread beyond the ovaries, chemotherapy and rarely, radiation, will also be used as part of treatment.
Key Q&A
- What is ovarian cancer?There are three main types of ovarian cancer tumors—germ cell tumors, stromal tumors and epithelial tumors. About 90 percent of ovarian cancer patients have an epithelial tumor, which begins in the surface tissue of the ovary (epithelium).
- What causes ovarian cancer?The specific cause of ovarian cancer is unknown. But there are some common risk factors, including your personal and family history and never having a pregnancy.
- What are the symptoms of ovarian cancer?Historically, ovarian cancer was referred to as the “silent killer” because symptoms are easily mistaken as other conditions; by the time they’re associated with ovarian cancer, the disease has already spread through a woman’s abdomen and beyond. Regardless, symptoms include: a feeling of being bloated, vague abdominal and pelvic discomfort, gastrointestinal symptoms such as gas and constipation, back pain and fatigue.
- What kinds of tests will my health care professional order?It depends on your health, age and history. Remember, sometimes diagnosing a disease is a matter of ruling other things out first, so you may have to go through a number of tests so your health care professional can make a firm diagnosis. One of the first might be a Pap smear. After that, you may have a CA-125 blood test, abdominal or transvaginal ultrasound, a CT scan or a lower GI series (barium enema).
- What are the treatment options for ovarian cancer?Treatments vary depending on the stage of disease, your age and your overall health condition. The primary treatments include surgery, chemotherapy and rarely, radiation.
- How can I find out if I have a mutation on the BRCA1 or BRCA2 genes and what if I do?First, realize that everyone has these genes. They are designed to help prevent the over-production of cells. Only about 10 percent of women with ovarian cancer have a mutation in one or both of these genes. If you have a defect in the BRCA1 or BRCA2 gene, it means that you may have an 18 percent to 62 percent chance of getting ovarian cancer. If you have a history of ovarian cancer in your family, you can seek the help of a qualified genetic counselor to conduct an extensive genetic/medical history and obtain advice about whether or not to proceed with the test. Finally, if either of these genes is defective, it doesn’t mean you’ll get cancer. Plus, you can take preventive steps such as having your ovaries removed to significantly reduce your risk. Seek advice from your health care professional on how to proceed.
- My father had colon cancer and I heard that, not only am I a candidate for the same disease, but that my chances for ovarian cancer are increased as well. Is that true?Yes. Hereditary nonpolyposis colon cancer is caused by a defect in certain genes. This defect reduces your body’s ability to repair damage to its DNA and results in very high risks for colon, endometrial (the lining of the uterus) and ovarian cancers. Again, if this form of cancer is in your family, you may want to consider genetic counseling and testing.
- Why am I supposed to avoid talcum powder?Some studies suggest that when women put talcum powder directly on the genital area, or even on sanitary napkins, it increases the risk of ovarian cancer. You might want to substitute a cornstarch-based product to be safe.
For more information visit us our website: https://www.healthinfi.com
0 200


No Comments