Alpha-1
Alpha-1 antitrypsin deficiency is an inherited disorder that may cause lung disease and liver disease. The signs and symptoms of the condition and the age at which they appear vary among individuals.
People with alpha-1 antitrypsin deficiency usually develop the first signs and symptoms of lung disease between ages 20 and 50. The earliest symptoms are shortness of breath following mild activity, reduced ability to exercise, and wheezing. Other signs and symptoms can include unintentional weight loss, recurring respiratory infections, fatigue, and rapid heartbeat upon standing.
Affected individuals often develop emphysema, which is a lung disease caused by damage to the small air sacs in the lungs (alveoli). Characteristic features of emphysema include difficulty breathing, a hacking cough, and a barrel-shaped chest. Smoking or exposure to tobacco smoke accelerates the appearance of emphysema symptoms and damage to the lungs.
About 10 percent of infants with alpha-1 antitrypsin deficiency develop liver disease, which often causes yellowing of the skin and whites of the eyes (jaundice). Approximately 15 percent of adults with alpha-1 antitrypsin deficiency develop liver damage (cirrhosis) due to the formation of scar tissue in the liver. Signs of cirrhosis include a swollen abdomen, swollen feet or legs, and jaundice. Individuals with alpha-1 antitrypsin deficiency are also at risk of developing a type of liver cancer called hepatocellular carcinoma.
In rare cases, people with alpha-1 antitrypsin deficiency develop a skin condition called panniculitis, which is characterized by hardened skin with painful lumps or patches. Panniculitis varies in severity and can occur at any age.
Alpha-1 Antitrypsin Deficiency (Alpha-1) is a genetic (inherited) condition – it is passed from parents to their children through their genes. Alpha-1 may result in serious lung disease in adults and/or liver disease at any age.
What Is Alpha-1 Antitrypsin Deficiency?
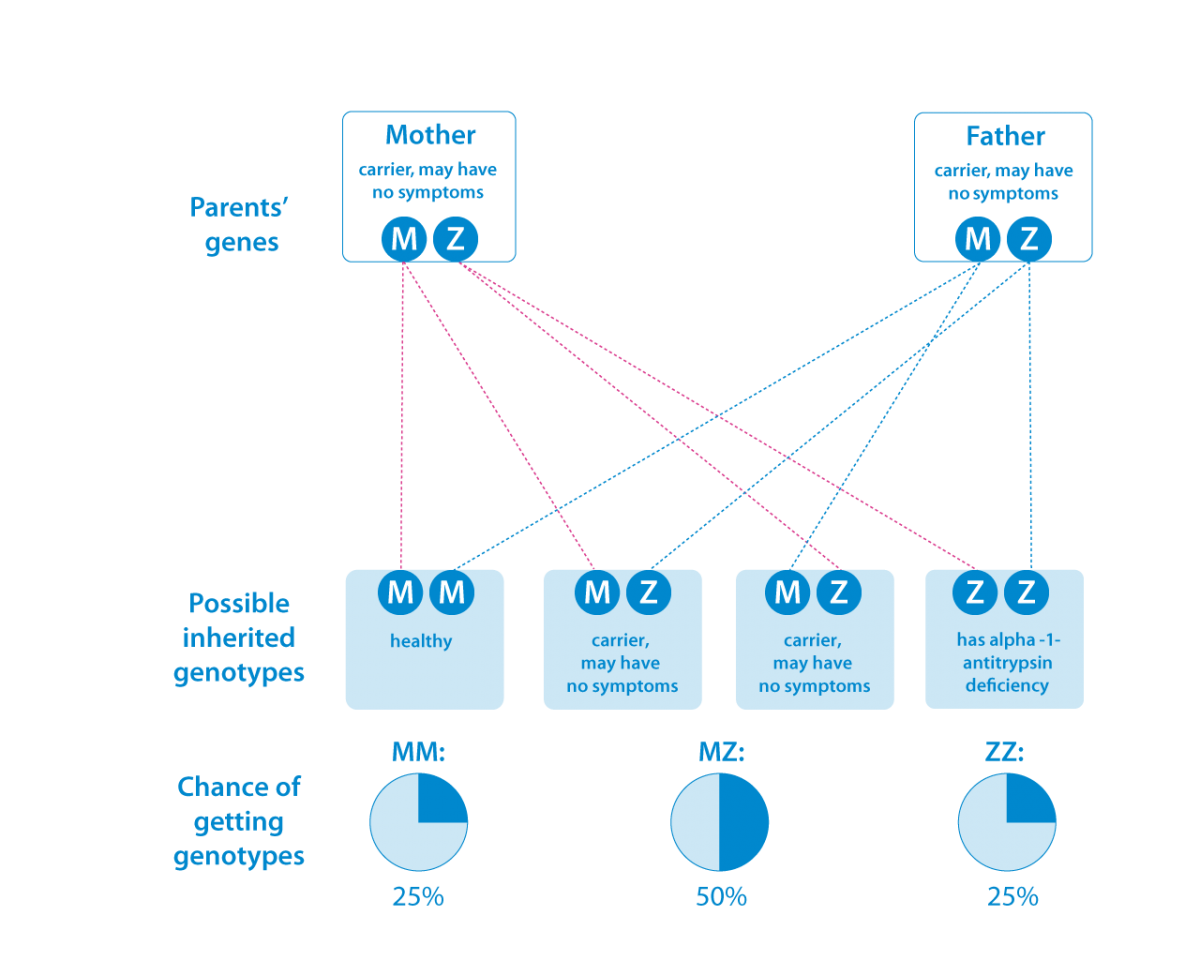
For each trait a person inherits, there are usually two genes; one gene comes from each parent. People with Alpha-1 have received two abnormal alpha-1 antitrypsin genes. One of these abnormal genes came from their mother and one from their father.
Also called AAT deficiency, alpha-1 antitrypsin deficiency is a genetic disease, which means it’s passed down from your parents. It can cause serious lung disease that makes it hard to breathe. It can also cause liver disease that leads to jaundice, which makes your skin look yellowish.
There’s no cure, but treatments can help you manage your liver and breathing problems.
You get the disease because your liver doesn’t make enough of a protein called alpha-1 antitrypsin, or AAT. You need AAT to protect your lungs from getting broken down. Without it, infections and other irritants, like tobacco smoke, break down parts of your lung even faster.
If you have AAT deficiency, you might not have any breathing symptoms until you’re in your 20s or 30s. But when they start, you could feel short of breath or wheeze when you breathe, just like someone who has asthma.
For some people, AAT deficiency can cause chronic pulmonary obstructive disease (COPD). When you have COPD, you often have symptoms of emphysema, a serious condition that makes it hard for you to push air out of your lungs. COPD can make you cough up mucus, make you wheeze or have trouble breathing, and make your chest feel tight.
You also might have chronic bronchitis, an irritation of your airways that makes you cough a lot and have trouble breathing.
You’ll probably need to take medicine through an inhaler that you carry around, like the type that people with asthma use. It’s something you’ll need to do throughout your life.
Keep in mind that no two cases of AAT deficiency are alike. Not everyone gets severe symptoms. With treatment, you’ll probably still be able to work, exercise, and enjoy many of your favorite hobbies.
Reach out to a circle of friends and family, and ask your doctor about support groups. It can help to talk to people who understand just what you’re going through.
Alpha-1 antitrypsin deficiency (Alpha-1) is a genetic (inherited) disorder which results in an absence or low levels of AAT protein in the blood. These low levels prevent AAT protecting the lungs from the destructive damage of neutrophil elastase resulting in lung tissue damage. Alpha-1 is not a rare disease but it is massively under-diagnosed. It classically presents with early-onset emphysema and liver disease in childhood and occasionally in adulthood. Both the ATS/ERS and WHO recommend Alpha-1 testing for the following patients:
- All COPD patients
- All non-responsive asthmatics (adults/adolescents)
- All patients with cryptogenic cirrhosis/liver disease
- All first degree relatives of patients and carriers with AAT deficiency
The National Alpha-1 Targeted Detection Programme was established in 2004 to provide testing free of charge to suspected individuals throughout Ireland.
Causes
Alpha-1 antitrypsin deficiency runs in families. If you have it, you got it from faulty genes that both your parents passed on to you.
Some people get the genes but don’t get any symptoms. Or they have the mild version of the disease.
The broken genes you get from your parents cause you to have a low level of AAT protein in your blood. It can build up in the liver instead of going into your bloodstream.
That buildup in your liver causes liver disease. The shortage of AAT protein in your bloodstream leads to lung disease.
Symptoms
You might not know you have the disease until you’re an adult, between the ages of 20 and 40. You may feel short of breath, especially when you try to exercise. You also may start to wheeze or have a whistling sound when you breathe.
You may also get a lot of lung infections. Other warning signs include:
- Feeling tired
- Your heart beats fast when you stand up
- Weight loss
If AAT deficiency causes problems with your liver, you might have symptoms like:
- Yellowish skin or eyes
- Swollen belly or legs
- Coughing up blood
A newborn baby might have jaundice, or a yellow coloring of the skin or eyes, very yellow urine, poor weight gain, an enlarged liver, and bleeding from the nose or umbilical stump.
In rare cases, a skin disease called panniculitis causes hardening of the skin with painful lumps or patches.
The gap between basic academic research and the marketing of new drugs, the principal impediment to drug development for rare diseases, can be bridged by a partnership between biotechnology companies and voluntary health advocacy (VHA) organizations. Venture philanthropy has emerged as the ideal model for this partnership by linking expertise in biotechnology with the resources of VHA’s including academic researchers, donors and patient populations for new drug testing.
Pathology
Alpha-1 antitrypsin is a protein that prevents enzymes such as elastase from degrading normal host tissue. Over 90% of the alpha-1 antitrypsin protein is produced in hepatocytes by codominant gene expression on chromosome 14. The alpha-1 antitrypsin protein inhibits neutrophil elastase. In patients with severe deficiency, the neutrophil elastase acts unopposed resulting in damage to the lower respiratory tract. This damage is predominantly basal because of the gravitational distribution of pulmonary blood flow.
- Associations
- asthma
- pancreatitis
- aneurysms, including intracranial aneurysms
- Complications
- cirrhosis with increased risk of hepatocellular carcinoma Radiographic features
Thoracic manifestations
Plain radiograph and CT
pan-lobular emphysema
the emphysema pattern was traditionally thought to be panlobular, although more recent studies have also suggested a variable pattern to the emphysema
basal predominance, in contradistinction to centrilobular emphysema, which shows apical predominance; the two conditions can coexist in smokers
- emphysema may develop in 75-85% of cases
- bronchiectasis: up to 40%
- frank bullae formation: non-specific feature
- bronchial wall thickening: non-specific feature
hepatopulmonary syndrome
AAT deficiency carriers are at 70-100% increased risk of lung cancer
Diagnosis
Your doctor may ask you questions such as:
- Do you feel short of breath?
- Have you been getting a lot of colds or lung infections?
- Have you lost weight lately?
- Have you noticed any yellowing of your skin or eyes?
Your doctor will also listen to your breathing with a stethoscope to check for wheezing or other signs that your lungs aren’t working right.
You need to get blood tests to confirm your diagnosis. These tests check to see if you have the broken genes that cause AAT deficiency. They also look to see how much of the protein you have in your bloodstream.
Your doctor will also order tests of your lungs and liver to see how much damage the condition has caused. For example, a chest X-ray shows signs of emphysema.
A special blood test checks the oxygen level in your arteries, a sign of how well your lungs work. You might breathe into a tube to see how much air you’re getting into your lungs.
Another blood test checks for problems with your liver. You may also get a liver biopsy, in which your doctor uses a very thin needle to take some cells from your liver and check for signs of damage.
Treatment
Although there’s no cure for AAT deficiency, you can raise the amount of AAT protein in your blood, which protects you against more lung damage. Doctors call this augmentation therapy. You may have this treatment if you get emphysema.
Augmentation therapy is also called “replacement therapy.” You get a new supply of AAT protein that comes from the blood of healthy human donors. You get the treatment once a week. The “replacement” alpha-1 gets into your body through an IV. You can have this done at home with the help of a technician, or you can go to a doctor’s office.
The goal of augmentation therapy is to slow or stop the damage in your lungs. It won’t reverse the disease or heal any damage you already have.
You will need these treatments throughout your life.
Depending on how you’re doing, you also may get medication that you breathe into your lungs with an inhaler. Doctors call this a bronchodilator, meaning that it opens your airways.
If your breathing trouble leads to low levels of oxygen in your blood, you might need to get extra oxygen through a mask or nosepiece. Your doctor will also give you a referral for pulmonary rehab to help you breathe better.
Taking Care of Yourself
Good habits are very important to help you stay healthy with this condition. You shouldn’t smoke, and you need to get a pneumonia vaccine and your annual flu shot.
Talk to your doctor about how to exercise safely, which strengthens your lungs.
Good nutrition — including supplements with vitamins E, D, and K — can help you keep your liver healthy. Avoid dust and smoke, and wash your hands often to prevent infection. Limit the alcohol you drink to protect your liver.
Babies with AAT deficiency may need a special milk formula or extra vitamins. It’s also important for them to have regular medical checkups to keep track of how well their lungs and liver are working.
upport from your loved ones, and from others who have the same condition, also makes a big difference, so you know there are people who understand what you’re going through.
What to Expect
AAT deficiency is different for everyone. Some people have severe problems, but others may have few or no symptoms.
In babies and children, the condition is more likely to cause liver damage than lung problems. Still, only about 10% of children with it have severe liver disease. Children with AAT deficiency also may have asthma.
You’ll be more sensitive to smoke and dust, and even the common cold can lead to breathing problems. About 30% to 40% of people with this condition will have liver problems at some point in their lives. Finding out if you have AAT deficiency is the first step toward the healthy habits and medical treatments that help control the disease.
Is alpha-1 antitrypsin deficiency inherited?
Alpha-1 antitrypsin deficiency is inherited in families in an autosomal codominant pattern. Codominant inheritance means that two different variants of the gene (alleles) may be expressed, and both versions contribute to the genetic trait.
The M gene is the most common allele of the alpha-1 gene. It produces normal levels of the alpha-1 antitrypsin protein.
The Z gene is the most common variant of the gene. It causes alpha-1 antitrypsin deficiency. The S allele is another, less common variant that causes ATTD.
If a person inherits one M gene and one Z gene or one S gene (‘type PiMZ’ or ‘type PiMS’), that person is a carrier of the disorder. While such a person may not have normal levels of alpha-1 antitrypsin, there should be enough to protect the lungs. However, carriers with the MZ alleles have an increased risk for lung disease, particularly if they smoke.
A person who inherits the Z gene from each parent is called ‘type PiZZ.’ This person has very low alpha-1 antitrypsin levels, allowing elastase – an enzyme especially of pancreatic juice that digests elastin – to damage the lungs. A person who inherits an altered version called S and Z is also likely to develop AATD.
Drug Therapy Development Pipeline
While currently available therapies may halt the progression of lung disease, there are currently no effective treatments for the liver disease and a cure for Alpha-1 remains elusive. Academic research, to a great extent supported by the Alpha-1 Foundation, has identified novel drug targets but is not in the business of drug development. Large pharmaceutical companies on the other hand have the means of introducing new drugs to the market but until now have been reluctant to invest in new drug development for rare diseases.
For more information visit us our website: https://www.healthinfi.com
3 500

No Comments