About Bean Syndrome
Blue rubber bleb nevus syndrome (or “BRBNS”, or “blue rubber bleb syndrome, or “blue rubber-bleb nevus”, or “Bean syndrome”) is a rare disorder that consists mainly of abnormal blood vessels affecting the gastrointestinal tract.
It was characterized by William Bean in 1958. BRBNS is caused by somatic mutations in the TEK (TIE2) gene.
Blue rubber bleb nevus syndrome is a condition in which the blood vessels do not develop properly in an area of the skin or other body organ (particularly the intestines). The malformed blood vessels appear as a spot or lesion called a nevus. The underlying blood vessel malformations are present from birth even though the nevus may not be visible until later in life.
The size, number, location, and severity of these malformations vary from person to person. Affected areas on the skin can be painful or tender to the touch and may be prone to sweating (hyperhidrosis). Nevi in the intestines can bleed spontaneously and cause anemia or more serious complications. Other symptoms vary depending on the organ affected. Treatment is tailored to the individual depending on the location and symptoms caused by the affected areas.
Blue rubber bleb nevus syndrome (BRBNS) is a rare condition that is characterized by numerous malformations of the venous system that significantly involve the skin and visceral organs. This condition was initially discovered in 1860 by Gascoyen. However, it was later made famous in 1958, by William Bennett Bean for which the disease has been termed “bean syndrome,” later referenced as blue rubber bleb nevus syndrome. BRBNS is an important condition due to the potential for significant bleeding which can be fatal.
Blue rubber bleb nevus syndrome (BRBNS) is a rare blood vessel (vascular) disorder that affects the skin and internal organs of the body. Multiple distinctive skin lesions are usually characteristic of this disorder and are often present at birth or present during early childhood. Lesions in the gastrointestinal tract frequently become apparent during childhood or early adulthood. The lesions are multifocal venous malformations, resulting from abnormal embryonic blood vessel development.
Blue rubber bleb nevus syndrome (BRBNS) also called Bean’s syndrome is a rare disorder characterized by multiple cutaneous venous malformations in association with visceral lesions, most commonly affecting the gastrointestinal tract. We report here, a 21-year-old woman patient, who presented with unilateral, blaschkoid distribution of cutaneous venous malformations along with blue rubber bleb nevus and recurrent episodes of hematochezia due to vascular lesions in the sigmoid colon; likely to be a case of BRBNS. The unusual unilateral, blaschkoid distribution of BRBNS prompted this present report.
Blue rubber bleb nevus syndrome (BRBNS) is an uncommon condition with multiple venous malformations of the skin, gastrointestinal tract, and other visceral sites including the liver, spleen, bladder, spinal cord, lungs, and bones. Clinically, the lesions are characteristically blue/purple soft compressible nodules with a rubbery feel.
They are dome shaped, almost nipple-like “rubber blebs,” which may coalesce to form large masses
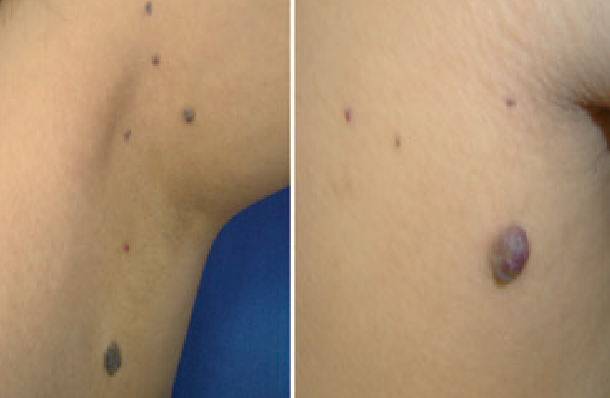
What Is Bean Syndrome?
. The gastrointestinal tract is the most common visceral site affected, and lesions share the same pathology as the cutaneous lesions. They are sessile or polypoid and affect all levels of the gastrointestinal tract, in particular, the small intestine. They are prone to bleeding and may cause a significant anemia requiring transfusion and iron replacement therapy.
Symptoms
Symptoms and severity of blue rubber bleb nevus syndrome varies greatly from person to person. In general, blue rubber bleb nevus syndrome is characterized by skin spots (nevi) that may be few to hundreds in number. Size tends varies from millimeters to several centimeters in length. These nevi are made of blood vessels and are spongy, meaning they can easily be pressed upon.
When pressure is released, they refill with blood and regain their original shape. They tend to be blue but can vary in color and shape. The surface of the nevi may be smooth or wrinkled and they often have a rubbery feel. They do not tend to bleed spontaneously, but are fragile and will bleed if injured. They may be tender to the touch. They may also be associated with increased sweating in the area of the skin legions. The number and size of legions may worsen with advancing age.
Nevi may also be found in the intestines (particularly the small intestine) in individuals with blue rubber bleb nevus syndrome. These nevi can bleed spontaneously causing anemia. Most bleeding from the gastrointestinal tract is slow; however, sudden quick bleeding (hemorrhage) is possible. Other serious complications of gastrointestinal legions may include intussusception, bowel infarction, and even death.
Blue rubber bleb nevus syndrome can affect other body organs as well. Nevi have been reported in the skull, central nervous system, thyroid, parotid, eyes, mouth, lungs, pleura, pericardium, musculoskeletal system, peritoneal cavity, mesentery, kidney, liver, spleen, penis, vulva, and bladder. Nevi may also put pressure on joints, bones, or feet, which may make walking difficult or limit range of motion.
This table lists symptoms that people with this disease may have. For most diseases, symptoms will vary from person to person. People with the same disease may not have all the symptoms listed. This information comes from a database called the Human Phenotype Ontology (HPO) . The HPO collects information on symptoms that have been described in medical resources. The HPO is updated regularly. Use the HPO ID to access more in-depth information about a symptom.
BRBNS is characterized by soft, elevated lesions on the skin or just under the skin that are dark blue, red, purple-red or black in color. The venous malformations may be tender, contain blood and be easily compressed and are usually located on the upper limbs, trunk and soles of the feet but can occur anywhere.
The lesions increase in size and become more apparent over time but have not been reported to become cancerous. The organ system most commonly affected by BRBNS is the gastrointestinal (GI) tract, particularly the small intestine. The lesions in the GI tract often bleed and can lead to mild or severe anemia. Iron replacement and/or frequent blood transfusions may be required. The GI lesions can also cause an obstruction or blockage (intussusception) of part of the bowel. Skeletal abnormalities and venous malformations in muscle are sometimes associated with BRBNS.
- Symptoms of blue rubber bleb nevus syndrome (BRBNS) are usually apparent at birth or by early childhood, but in some cases symptoms do not become apparent until adulthood.
- BRBNS involves a malformation of cutaneous (skin) and gastrointestinal (stomach and intestines) veins, which are blood vessels that carry blood to the heart. This causes patients with BRBNS to develop hemangiomas, which are lesions consisting of a buildup of dilated, or expanded, blood vessels. BRBNS patients may develop anywhere from a few lesions to hundreds of lesions. These skin lesions are usually benign, that is, they do not become cancerous and invade other tissues.
- Patients with BRBNS may develop hemangiomas on the skin. Skin hemangiomas are usually 1-2 centimeters in size and blue or purple in color. These lesions may be painful or tender when touched, and they may be either flat or elevated. They may appear anywhere on the body, but are most common on the upper limbs and trunk.
- Patients may also develop hemangiomas on internal organs, most commonly in the small intestine and on other parts of the gastrointestinal tract. Hemangiomas have also been reported on other internal organs, including the kidney, liver, spleen, and lungs, as well as on joints. Internal hemangiomas are more likely to bleed than those on the skin.
Cause
Currently the cause of blue rubber bleb syndrome is not known.
Blue rubber bleb nevus syndrome is sporadic. Although families have been described in which the condition follows autosomal dominant inheritance, these families actually have other multifocal venous malformations.
Diagnosis
BRBNS is diagnosed by physical examination and a procedure in which the GI tract is illuminated and visualized (endoscopy). Genetic testing for BRBNS is available on a research basis only.
- Blue rubber bleb nevus syndrome (BRBNS) is diagnosed based on the presence of hemangiomas on the skin and in the gastrointestinal tract.
- Visual exam: Hemangiomas on the skin are visible and may be assessed by a doctor during a clinical exam.
- Endoscopy: If hemangiomas are seen on the skin, doctors can perform an endoscopy to check for lesions in the gastrointestinal tract. In an endoscopy, a flexible tube with a light attached is inserted down a patient’s throat. The endoscope can transmit images of the patient’s gastrointestinal tract so that any lesions can be observed.
- Magnetic resonance imaging (MRI): MRI is a noninvasive imaging technique that may be used to check for the presence of internal lesions. MRI uses magnetic waves and radio waves to take an image of tissues within the body.
Treatment
Treatment of blue rubber bleb nevus syndrome varies depending on the severity and location of the affected areas. Skin spots do not usually require treatment, but some individuals with this condition may want treatment for cosmetic reasons or if the location of the nevus causes discomfort or affects normal function.
Bleeding in the intestines may be treated with iron supplements and blood transfusions when necessary. Surgery to remove an affected area of bowel may be recommended for repeated or severe bleeding (hemorrhage).
Iron therapy and blood transfusions are used to conservatively manage BRBNS. The skin lesions associated with BRBNS can be treated with laser therapy, injection of chemicals that collapse the lesion (sclerotherapy) or surgical removal.
Lesions in the gastrointestinal system are usually not removed unless bleeding leads to anemia and necessitates repeated blood transfusions. Gastrointestinal lesions can be safely removed surgically, but one or several lengthy operations may be required.
- Currently, there is no cure for blue rubber bleb nevus syndrome (BRBNS). If treated properly, however, most patients are able to live normal lives and have a normal lifespan.
- Diet: Due to internal bleeding, patients with BRBNS may have low iron (which is stored in red blood cells). It is recommended that patients take dietary iron supplements and/or consume foods that are high in iron (such as beef, pork, poultry, or legumes).
- Amputation: In severe cases of BRBNS, hemangiomas may cause the limbs to stop working properly due to enlargement and disfiguration. When this happens, amputation of the affected limbs may be necessary.
- Surgery: When a blood vessel bursts, or if internal bleeding becomes excessive, surgery may need to be performed to stop the bleeding. In some cases, the part of the gastrointestinal tract that is causing the bleeding may be surgically removed.
- Cosmetic surgery: Although the skin lesions that appear on patients with BRBNS are usually benign (they do not become cancerous and invade other tissues), patients may decide to have them removed for cosmetic or appearance reasons. Laser surgery may be performed to remove skin lesions. Laser surgery involves using a concentrated beam of light to cut and remove unwanted skin.
- Transfusion: Patients with BRBNS may lose significant amounts of blood due to internal bleeding and, as a result, may require regular blood transfusions. A blood transfusion is the transfer of additional blood into the body through an intravenous line.


No Comments