Granuloma annulare
Overview
Granuloma annulare is a skin condition that causes raised reddish or skin-colored bumps (lesions) in a ring pattern. The bumps are usually on the hands and feet.
Minor skin injuries and some drugs might trigger the condition. Different types affect adults and children.
The lesions usually disappear on their own within two years without treatment. But if you’re bothered by how your skin looks or feels, your doctor can prescribe medications that can speed the disappearance of the condition.
Granuloma annulare is a chronic degenerative skin disorder. The most common form is localized granuloma annulare, which is characterized by the presence of small, firm red or yellow colored bumps (nodules or papules) that appear arranged in a ring on the skin. In most cases, the sizes of the lesions range from one to five centimeters.
The most commonly affected sites include the feet, hands, and fingers. In addition to the localized form, there are four less common forms: generalized or disseminated, linear, perforating, and subcutaneous. The lesions associated with granuloma annulare usually disappear without treatment (spontaneous remission). However, the lesions often reappear. The exact cause of granuloma annulare is unknown.
What is granuloma annulare?
Granuloma annulare (GA) is a common inflammatory skin condition typified clinically by annular, smooth, discoloured papules and plaques, and necrobiotic granulomas on histology. Granuloma annulare is more correctly known as necrobiotic papulosis.
Granuloma annulare is seen most commonly on the skin of children, teenagers, or young adults. The generalized form is more likely to be found in older adults (mean age 50 years). There is a female predominance of 2:1 over males.
Symptoms
This skin condition rarely causes symptoms, such as pain or itch. Because there are different types, it can show up on the skin in various ways.
Five recognized forms or clinical variants of granuloma annulare have been identified. The most common form is localized granuloma annulare. The four other forms (i.e., generalized or disseminated, linear, perforating, and subcutaneous) occur less often than the localized form.
All forms of granuloma annulare are characterized by small, firm bumps (nodules or papules) arranged in a ring on the skin. These bumps are usually skin-colored or slightly red or yellow. Most cases of granuloma annulare clear up without treatment (spontaneous resolution). However, recurrences are common.
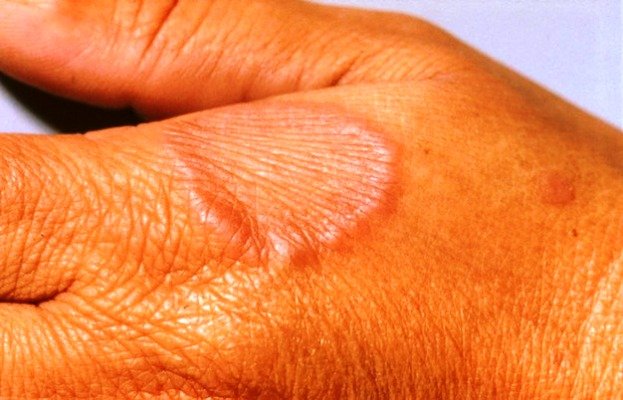
Localized GA presents with small, skin-colored or reddish firm bumps (erythematous papules) on the back of arms, wrists, ankles, hands, and feet. The bumps are usually, but not always, arranged in a circular or ring pattern. Involvement of the palms of the hands, face, scalp, and genitals is rare. Lesions of localized GA typically grow slowly, and in about 50% of the cases there is more than one lesion.
Generalized GA may present as widespread bumps (papules), multiple ring shaped, raised patches (plaques), and/or large discolored, oddly shaped plaques. The color of the papules and plaques may be skin color, yellow, reddish pink, or violet and may cause itching. The sizes of the plaques may range from millimeters to several centimeters in diameter. The lesions of generalized GA can form anywhere on the body, but are most common on the trunk, arms, and legs. Generalized GA can affect the neck, face, scalp, soles of feet, and palms of hands.
Granuloma annulare may affect any area of the body. The fingers, hands, and feet are the areas most often affected. In most cases, both sides of the body are affected (symmetrical). Other commonly affected areas include the forehead, neck, and abdomen. Localized granuloma annulare normally affects one specific area of the body.
Generalized or disseminated granuloma annulare may affect several areas of the body at one time. The bumps associated with this form of GA are usually smaller and more numerous than those associated with the localized form. These bumps may also be itchy (pruritic).
Subcutaneous granuloma annulare may present as a solitary, painless mass or nodule underneath the skin (subcutaneous). The scalp, arms, and legs are most often affected. Children are affected more often than adults.
Perforating granuloma annulare is characterized by bumps or pustules that develop a yellow center. These lesions may leak a clear fluid, become crusted and eventually leave a scar. These lesions may come together (coalesce) to form larger plaques.
Linear granuloma is an extremely rare form of granuloma annulare that most often affects the fingers.
These pictures of granuloma annulare show what you may see on your skin. Some people develop more than one type, so they have a few of these signs.
The signs and symptoms of granuloma annulare can vary, depending on the variety:
- Localized. This is the most common type of granuloma annulare. The bump (lesion) borders are circular or semicircular, with a diameter up to 2 inches (5 centimeters). The reddish or skin-colored bumps occur most commonly on the hands, feet, wrists and ankles of young adults.
- Generalized. Less commonly, adults experience this type, which causes itchy, reddish or skin-colored bumps on most of the body, including the trunk, arms and legs.
- Under the skin. A type that usually affects young children is called subcutaneous granuloma annulare. It produces small, firm lumps under the skin, instead of a rash. The lumps form on the hands, shins, and scalp.
How is granuloma annulare diagnosed?
Diagnosis and Management of Granuloma Annulare
Granuloma annulare is usually diagnosed clinically because of its characteristic appearance. But sometimes the diagnosis is not obvious, and other conditions may be considered. Skin biopsy usually shows necrobiotic degeneration of dermal collagen surrounded by an inflammatory reaction. See granuloma annulare pathology.
Granuloma annulare is often initially misdiagnosed as tinea because of the annular appearance; the lack of surface scale should lead away from this and other scaly rashes such as discoid eczema or psoriasis. Actinic granuloma is considered by some to be a photo-aggravated variant of granuloma annulare, and by others to be a distinct entity.
Granuloma annulare is a benign, asymptomatic, self-limited papular eruption found in patients of all ages. The primary skin lesion usually is grouped papules in an enlarging annular shape, with color ranging from flesh-colored to erythematous.
The two most common types of granuloma annulare are localized, which typically is found on the lateral or dorsal surfaces of the hands and feet; and disseminated, which is widespread. Localized disease generally is self-limited and resolves within one to two years, whereas disseminated disease lasts longer. Because localized granuloma annulare is self-limited, no treatment other than reassurance may be necessary.
There are no well-designed randomized controlled trials of the treatment of granuloma annulare. Treatment recommendations are based on the patho-physiology of the disease, expert opinion, and case reports only. Liquid nitrogen, injected steroids, or topical steroids under occlusion have been recommended for treatment of localized disease.
Disseminated granuloma annulare may be treated with one of several systemic therapies such as dapsone, retinoids, niacinamide, antimalarials, psoralen plus ultraviolet A therapy, fumaric acid esters, tacrolimus, and pimecrolimus. Consultation with a dermatologist is recommended because of the possible toxicities of these agents.
Granuloma annulare is a benign skin condition that typically consists of grouped papules in an enlarging annular shape. Their appearance ranges from flesh colored to erythematous. The etiology is unknown, but the disease usually is self-limited. Despite the dramatic appearance of this cutaneous eruption, it generally is asymptomatic; however, there may be some mild pruritus. The eruption can occur anywhere on the body, but it occurs least often on the face and most often on the lateral or dorsal surfaces of the hands and feet
Differential Diagnosis
Granuloma annulare can be mistaken for other common annular skin conditions such as tinea corporis, pityriasis rosea, nummular eczema, psoriasis, or erythema migrans of Lyme disease. The lack of any surface changes to the skin is the key feature that distinguishes granuloma annulare from these other skin conditions.
Specifically, there is no scale or associated vesicles or pustules with granuloma annulare; the skin surface is smooth. Less common annular skin conditions (e.g., subacute cutaneous lupus erythematosus, erythema annulare centrifugum) have associated scaling and can be ruled out. Urticaria also can present as annular plaques, but it is distinguished easily from granuloma annulare by its evanescent nature.
A less common annular skin condition, sarcoidosis, may present with reddish-brown to purplish infiltrated papules and plaques that commonly are found on the face. Hansen’s disease (leprosy) also has erythematous annular plaques with associated scaling, alopecia, and anesthesia.
Often, a diagnosis can be made without a punch biopsy, but in clinically confusing situations it may be helpful, especially with the subcutaneous variant of granuloma annulare. The presence of epithelioid histiocytes palisading around an anuclear dermis with mucin deposition is characteristic of granuloma annulare.
This granulomatous appearance of the biopsy and the annular clinical appearance combine to form the descriptive term “granuloma annulare.” If a biopsy is performed, the results typically will show focal degeneration of collagen with reactive inflammation and fibrosis. The epidermis is normal.
Epidemiology
Granuloma annulare affects patients of all ages. Most cases of localized granuloma annulare are diagnosed in patients before 30 years of age. Incidence is highest in women, with a ratio of 2.3 to 1.0 over men. approximately 15 percent of all patients with granuloma annulare will have more than 10 lesions (i.e., disseminated granuloma annulare).
These patients are usually children younger than 10 years or adults older than 40 years. Although uncommon, cases of granuloma annulare occurring in siblings, twins, and successive generations have been reported. Seasonal peaks of granuloma annulare in the spring and fall also have been described.
The duration of the skin eruption varies. In more than one-half of patients, it resolves spontaneously within two months to two years. However, cases of disseminated granuloma annulare may last three to four years or as long as 10 years. The eruption may recur as well, with 40 percent of children having recurrent lesions.
Etiology
The cause of granuloma annulare is unknown, but it has been reported to follow trauma, malignancy, viral infections (including human immunodeficiency virus [HIV], Epstein-Barr virus, and herpes zoster), insect bites, and tuberculosis skin tests. A delayed-type hypersensitivity reaction and cell-mediated immune response are hypothesized. In one retrospective study, 12 percent of patients with granuloma annulare had diabetes mellitus. This study did not have a comparison group, so it is not clear whether the prevalence of diabetes mellitus was higher or lower than in the general population.
Patients with diabetes mellitus had a higher incidence of chronic relapsing granuloma annulare than patients without diabetes. A case-control study that included patients with and without diabetes failed to reveal any statistically significant correlation between granuloma annulare and type 2 diabetes. Some isolated cases of granuloma annulare found in association with malignant neoplasm have been reported. In these cases, the malignant neoplasms were primarily lymphoma, but some were prostate cancer. Granuloma annulare has occurred in all stages of HIV infection as well.
Clinical Presentation
The four main clinical variants of granuloma annulare are: localized, disseminated, subcutaneous, and perforating.
The localized form of granuloma annulare composes 75 percent of cases.11 Localized granuloma annulare starts as a ring of small, firm, flesh-colored or red papules. As the condition progresses, there is some central involution, and the ring of papules slowly increases from 0.5 to 5.0 cm in diameter. The lesions may be isolated or coalesce into plaques. More than 50 percent of these patients will have spontaneous resolution within two years.
Disseminated or generalized
Disseminated or generalized granuloma annulare is similar to the localized variant but is more widespread, having the papules may fuse to form annular lesions on the extremities, trunk, and neck. In contrast to the localized form, these lesions may persist for three to four years or longer.
Causes
Granuloma annulare may be a delayed hypersensitivity reaction to a component of the dermis or a reaction pattern to numerous triggers. Reported triggering events have included many skin infections and infestations, and types of skin trauma. Inflammation is mediated by tumour necrosis factor alpha (TNFα). The reason this occurs is unknown.
The exact cause of granuloma annulare is unknown (idiopathic). Numerous theories exist linking the cause to trauma, sun exposure, thyroid disease, tuberculosis, and various viral infections. However, no definitive proof has been shown for any of these theories.
The disseminated type of the disorder, which affects large areas of the body, may be associated with diabetes mellitus. Granuloma annulare may also be a complication of pseudo rheumatoid nodules or shingles (herpes zoster). Some forms of GA tend to run in families (familial), but the exact mode of inheritance has not yet been determined.
There have also been a number of associations reported with systemic conditions including autoimmune thyroiditis, diabetes mellitus, hyperlipidaemia, and rarely with lymphoma, HIV infection and solid tumours.
It’s not clear what causes granuloma annulare. Sometimes it’s triggered by:
- Animal or insect bites
- Infections, such as hepatitis
- Tuberculin skin tests
- Vaccinations
- Sun exposure
- Minor skin injuries
- Drugs
Who gets granuloma annulare?
Medical records indicate that this skin condition is more common in females than males. It also seems that the perforating type of granuloma annulare develops most often in people who live in Hawaii. Otherwise, this disease seems to occur about equally in people of different races and parts of the world.
Most people who get this skin condition are otherwise healthy. Some studies, however, have found that people with certain diseases, such as an HIV infection, may be more likely to develop granuloma annulare.
Children tend to get the localized and subcutaneous types of granuloma annulare. The generalized and perforating types are more common in older adults.
Infants rarely get this skin condition.
Some types of this skin condition develop almost exclusively in children, while other types tend to appear in older adults.
What causes granuloma annulare?
It’s still unclear what causes this skin condition. Through studying granuloma annulare, scientists have learned that many things can trigger it. People often develop granuloma annulare after they:
- Injure their skin
- Take certain medications
- Develop another disease
It may be that granuloma annulare is a reaction that occurs in the skin. It may require a trigger, such as injuring your skin. Granuloma annulare often appears after people injure their skin.
Because this skin condition doesn’t develop in everyone who injures their skin, it’s possible that the people who develop it are especially sensitive to whatever injured their skin. For example, people have developed this skin condition after getting bit by an octopus, stung by a bee, or inked by a tattoo artist.
Granuloma annulare may also be more common if someone has a disease, such as the human immunodeficiency virus (HIV), thyroid disease, or diabetes. Not everyone who has one of these diseases will develop granuloma annulare. Again, it’s possible that the skin is reacting to what’s going on inside the body.
Before we know for sure what causes granuloma annulare, more research is needed.
Risk factors
Although granuloma annulare can occur in people of any race and at any age, it is most commonly seen in children and young adults. Females are slightly more likely than males to develop granuloma annulare.
Granuloma annulare is occasionally associated with diabetes or thyroid disease, most often when lesions are numerous or widespread. It may, rarely, be related to cancer, especially in older people whose granuloma annulare is severe, doesn’t respond to treatment, or returns after cancer treatment.
What are the types of granuloma annulare?
There are five main types of granuloma annulare. It is possible to develop more than one type of granuloma annulare at the same time.
-
Localized granuloma annulare:
The most common form of the condition, localized granuloma annulare causes a circular rash on the skin that may begin as small circles that later merge together.
You may notice several small bumps on your skin before developing a rash. The areas are usually
The localized granuloma annulare appears in just 1 or 2 areas, tends to affect children and young adults, and usually gets better on its own after a few months.
Pink, purple or skin-coloured patches typically appear on the fingers, backs of the hands, feet, ankles or elbows.
They, form rings that grow slowly until they’re about 2.5-5cm across. As the rings get bigger, they become flatter and more purple in colour before eventually fading.
In localised granuloma annulare, the top of the skin feels smooth and, unlike in other skin conditions, such as pityriasis versicolor, ringworm or eczema, it is not rough, dry or scaly.
The affected skin also feels firm as a result of inflammation in the middle layer of skin (dermis). There’s no change in the outermost layer of skin (epidermis).
-
Generalized granuloma annulare:
Bumps develop over a larger area, like the whole forearm, instead of in a smaller, more concentrated rash. The bumps eventually join to form large, discolored areas.
-
Subcutaneous granuloma annulare:
This type of granuloma annulare causes lumps to form under your skin. The lumps are usually firm and round. They are not painful. In most cases, lumps stay small, but they can grow quickly. Lumps are red, pink, or skin-colored.
-
Perforating granuloma annulare:
Small, painful, scaly bumps form on the hands and fingers. In some cases, bumps are itchy or painful, and they leak fluid. Some people develop widespread bumps that connect and then form larger rashes.
Granuloma annulare under the skin usually affects children. One or more firm, rubbery lumps develop under the skin.
They can range from 5mm-4cm in size. They can appear on the shins, ankles, feet, buttocks, hands, scalp and eyelids.
-
Patch granuloma annulare:
Red, reddish-brown, or purple flat areas of rash form on the skin. People may develop one or more areas of skin like this.
Treatment
Granuloma Annulare Natural Treatment
Medical literature contains limited reliable information on the treatment of granuloma annulare. The only double-blind, placebo-controlled crossover study concerning the treatment of disseminated granuloma annulare involved the use of oral potassium iodide. In this series of eight patients, there was no advantage of high-dose potassium iodide over placebo.
Most medical literature on treatment of granuloma annulare is limited to individual case reports and small series of patients treated without a control group. Such studies cannot establish treatment effectiveness, particularly with a self-limited disease.
Because localized granuloma annulare is self-limited and asymptomatic, treatment usually is not necessary. Nevertheless, many patients remain troubled by the appearance and persist in seeking treatment. For patients insisting on treatment, options include intraregional corticosteroid injection with 2.5 to 5.0 mg per mL triamcinolone (Aristocort) into the elevated border, topical corticosteroids under occlusion, cryotherapy, and electrodessication. Patients should be warned that all of these treatments could cause scarring and atrophy.
One uncontrolled study of 31 patients with localized granuloma annulare showed 81 percent resolution after one treatment with liquid nitrogen or nitrous oxide. Systemic therapy is required for disseminated granuloma annulare, and many different treatments have been proposed (Table 117, 19–37). The possible benefit of treatment, which is unclear given the lack of clinical trials, must be balanced against the significant toxicities of most of these treatments. Therefore, the family physician must proceed with caution and should consider consultation with a dermatologist.
Dapsone is an antibiotic commonly used for dermatitis herpetiformis or Hansen’s disease. It has been reported to be effective in managing disseminated granuloma annulare. Isotretinoin (Accutane) is better known for treating severe acne, but it has been shown to be effective in treating granuloma annulare in numerous case reports. Serious adverse effects such as elevated triglyceride levels, elevated liver enzyme levels, and teratogenicity can occur. Two isotretinoin treatment failures also have been published. Etretinate, another retinoid (not available in the U.S.), also has been reported to be effective.
Antimalarial agents, including hydroxychloroquine (Plaquenil) and chloroquine (Aralen), have been used in the treatment of granuloma annulare. They have been presumed effective because of their immunosuppressive and anti-inflammatory properties. Serious side effects are possible, including retinopathy, aplastic anemia, and liver toxicity. Effective use of cyclosporine (Sandimmune) has been reported in individual patients. Close monitoring of serum creatinine levels and blood pressure is needed with this drug.
Niacinamide has been used and is reasonably safe, even at high doses. Nevertheless, liver toxicity is an important adverse effect, and hepatic transaminase levels should be monitored during treatment. Oral psoralen (e.g., anthralin [Anthra-Derm]) and psoralen plus ultraviolet A (PUVA) therapy has been reported to be effective in two uncontrolled studies with a total of six patients. However, long-term PUVA therapy carries a risk of increased incidence of nonmelanoma skin cancer. Vitamin E combined with a 5-lipoxygenase inhibitor (e.g., zileuton [Zyflo]) has been tried and was successful, but only in a series of three patients.
Fumaric acid esters, which also are used to manage psoriasis, were found to have some benefit in a recent study treating eight patients. One half of the study participants discontinued therapy because of gastrointestinal side effects.
In recent case reports, topical tacrolimus and pimecrolimus had positive outcomes. The incidence of side effects is very low.
Infliximab (Remicade), a tumor necrosis factor B inhibitor, demonstrated a positive outcome in a patient with recalcitrant disseminated granuloma annulare. Granuloma annulare is difficult to treat clinically; reassurance that the condition will self-resolve may be the best option. Clearly, well-designed clinical trials are needed to better direct treatment.
What treatment is available for granuloma annulare?
In most cases granuloma annulare does not require treatment because the patches disappear by themselves in a few months, leaving no trace. However, sometimes they persist for years. Treatment is not curative but may help individual lesions.
Local therapy
Options to consider include:
- Topical corticosteroid ointment under occlusion
- Intralesional steroid injections
- Destruction by cryotherapy or laser ablation
- Imiquimod cream
- Topical calcineurin inhibitors (tacrolimus and pimecrolimus).
Systemic therapy
Systemic therapy may be considered in widespread granuloma annulare. The following treatments have been reported to help at least some cases of disseminated granuloma annulare. None of these can be relied upon to clear it, and there are potential adverse effects.
- Systemic steroids
- Isotretinoin
- Methotrexate
- Potassium iodide
- Dapsone
- Hydroxychloroquine
- Pentoxifylline
- Allopurinol (note: allopurinol has also be cited as a cause of disseminated granuloma annulare)
- Combination of antibiotics once monthly: rifampicin, ofloxacin, minocycline
- Photochemotherapy (PUVA)
- UVA1 phototherapy (not available in New Zealand)
- Photodynamic therapy
- Ciclosporin
- Biologics particularly TNFα inhibitors such as adalimumab and infliximab
- Experimentally, oral and topical Janus kinase (JAK) inhibitors including tofacitinib
What is the outlook for granuloma annulare?
Individual lesions of localised granuloma annulare tend to clear within a few months or years, although they may recur even at the same site. Generalised and atypical variants are more persistent, sometimes lasting decades.
Prevention
Can granuloma annulare be prevented?
There is no way to prevent granuloma annulare.
Outlook & Prognosis
Prognosis
For most people, granuloma annulare (GA) goes away within a few years. It tends to last longer if it has spread to more parts of the body (generalized form) than if it is found in just one location (localized form). The generalized form may follow a pattern of spontaneously healing only to develop months or years later. About 25% of cases of generalized GA last for more than five years and for some it may last longer than 10 years
What is the prognosis (outlook) for people with granuloma annulare?
In most cases, granuloma annulare clears up on its own without treatment, leaving no trace behind. Most areas of rash disappear within two years.
However, because granuloma annulare is a chronic disease, lesions often return. Rashes usually return in the same place. Recurring problem areas often disappear faster than first-time rashes.
When should I call my doctor?
If you notice a rash or deep lump developing on or under your skin, contact your doctor for a thorough evaluation. It is also important to contact your doctor if you notice skin rashes that bleed, get larger, are itchy or painful, or change appearance in any way.
0 200


1 Comment