Overview
Breast Augmentation and Reduction is a novel concept in breast enhancement and only recently has it been described in the plastic surgery literature. For over a decade, however, I have been perfecting this alternative procedure, performing over 300 cases with great success and high patient satisfaction.
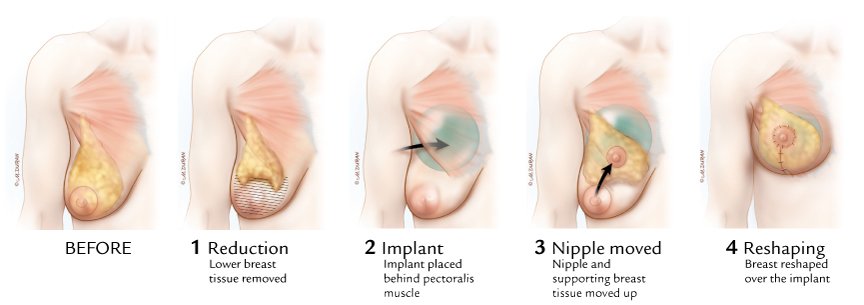
Breast augmentation today is one of the most frequently performed plastic surgery procedures, while breast reduction is commonly offered to women with overly large breasts that cause patient discomfort. In essence, the BAR procedure combines the best of these two procedures, removing saggy breast tissue at the bottom of the breast and adding volume to the upper breast with the implant.
The nipple-areola complex is moved to the ideal place on the face of the new breast. Compared to a breast reduction, the BAR procedure offers great benefits in terms of breast shape and location on the chest. It truly is the best of both worlds.
A mastopexy, or breast lift, does not require removal of breast tissue, but instead, reshapes the tissue and moves the nipple-areola complex to an improved location. This “lifting” procedure results in an improved shape but, again, the shape may not be particularly “youthful” and will not hold up over time; the breast will sag again within four months. A breast lift without an implant does not add superior breast fullness and if anyone tells you otherwise, I suggest you consult another surgeon.
According to the American Society of Aesthetic Plastic Surgery, in 2012, more than 10 million cosmetic surgical procedures were performed in the United States. Breast augmentation surgery remained the number one cosmetic procedure for women, followed by liposuction.
As breast aesthetic surgery becomes more common, past stereotypes and stigmas are changing. In a HealthyWomen survey, 53 percent of women said they were more accepting of breast augmentation than they used to be. Women surveyed described other women who have undergone breast augmentation surgery as confident (60 percent) and feminine (61 percent).
On the opposite end of the spectrum of breast aesthetic surgery is breast reduction. This procedure, which may be considered a cosmetic surgical procedure, is often performed to relieve significant physical and emotional problems resulting from overly large and/or heavy breasts. According to the American Society of Plastic Surgeons, in 2012, a total of 110,438 breast reductions were performed (including both reconstructive and cosmetic procedures).
Whether you choose to have your breasts increased, lifted or reduced, it’s important that you understand not only the benefits of the procedures, but the risks, costs and various surgical options available to you.
It’s also important that you choose the right plastic surgeon. Your surgeon should be board certified by the American Society of Plastic Surgeons, have privileges at a local hospital and be trained in the technique you’ve chosen. Always ask about your surgeon’s experience, complication rates and why he or she recommends a particular procedure. And don’t be afraid to get a second opinion—if your insurance is paying for the procedure, it will usually cover the cost of a second opinion Also ask to speak to several former patients about their experiences, whether they were happy with the surgeon and how they feel about their breasts today.
Diagnosis
Most women opting for any of the three breast procedures are young and healthy; however, a full medical evaluation is still required. For instance, if you smoke or are overweight, your health care professional may counsel you to quit smoking and/or lose weight, both of which reduce the risk of complications from surgery. Other things to tell your surgeon include:
- Other surgeries you’ve had on your breast or chest wall
- Medications you’re taking, including over-the-counter drugs, herbal and nutritional supplements and vitamins
- Any family history of breast cancer. While it is safe and recommended to have a mammogram with breast implants, you should ask your physician to direct you to a screening facility that offers a specialized technique that has been shown to improve the accuracy of mammograms in women with breast implants.
- Additionally, if you’re having breast reduction surgery, it’s a good idea to ask your surgeon to have the breast tissue evaluated by a pathologist. This evaluation could pick up early signs of breast cancer or cellular changes that signify an increased risk of developing breast cancer.
- Your expectations. Be very honest with yourself and your surgeon. What do you expect your breasts to look like after surgery? How long do you expect the recovery to take? What is your understanding of the risks and limitations? Do you expect the breast implants to last forever?
At the same time, you need to ask your surgeon for a realistic description of what the surgery will entail, how long recovery will take and what complications might arise.
Additionally, your surgeon should explain what type of anesthesia will be used, where the surgery will be performed (typically in a hospital operating room, outpatient surgical center or office operating suite), and how much the procedure costs. Very few insurance companies cover breast augmentation or lift for cosmetic reasons.
The national average for breast augmentation surgery is $3,543, and the national average for a breast lift is $4,280. You’ll also have to pay for the operating room, postsurgical hospital stay, anesthesia, and other costs.
Breast Augmentation
The decision to have breast augmentation is a personal one, often driven by a woman’s individual motivations to look as good as she feels. Women choose breast augmentation for many reasons: to restore and reshape, to increase the size and shape of their breasts and to enhance their bodies.
A Women survey found that of those women motivated to improve their appearance, nearly half (45 percent) said they would consider plastic surgery to do so. More than half of women (53 percent) said they are more accepting of breast augmentation surgery than they used to be, and 91 percent of women cited the desire to reshape their breasts following a major physical change, like weight loss or childbirth, as the primary reason for considering breast aesthetic surgery.
Some women have very small breasts, called macromastia. For these women especially, breast augmentation can significantly improve their overall self-confidence, self-perception and sense of attractiveness.
Make sure you ask your physician about the long-term implications of living with breast implants. For instance, when you have a mammogram, your mammography technician should use a specialized technique that has been shown to improve the accuracy of mammograms in women with breast implants.
This technique involves shifting the implant so the compression paddles compress and examine only breast tissue. Similar to some other medical devices, breast implants—saline or silicone—are not lifetime devices. It is likely that at some point they may need to be removed or replaced, and you should talk to your surgeon about this prior to surgery. According to the U.S. Food and Drug Administration, up to 20 percent of women who have breast augmentation surgery require removal of their implants within 8 to 10 years.
Also consider the costs of the procedure. The national average cost for breast augmentation is $3,543 for the surgeon’s fee alone. You’ll also have to pay for the operating room, postsurgical hospital stay, anesthesia and other costs. If your breast implants need to be removed or replaced at some point, this will involve additional costs. However, some breast implant manufacturers offer financing plans, which allow you to pay overtime and extended warranty plans (free and for a small charge) that cover all or part of future replacement costs.
Breast Lift
Gravity, pregnancy, nursing and age all contribute to the drooping and sagging of a woman’s breasts over time. As the skin stretches and the breasts begin to sag, some women turn to a procedure called mastopexy, or breast lift, to restore their breasts to a perkier, more youthful appearance.
Sometimes mastopexy is performed together with a breast implant, particularly if a woman’s breasts have shrunk after pregnancy. Women considering this combined procedure should have a thorough discussion with their surgeon about the risks and benefits. The American Society of Plastic Surgeons (ASPS) says the best candidates for mastopexy are healthy, emotionally stable women with realistic expectations of what the procedure will accomplish, particularly women with small, sagging breasts.
If you haven’t finished childbearing, the ASPS recommends you wait; another pregnancy and breastfeeding may stretch your breasts again, although the procedure doesn’t affect your ability to breastfeed. Also keep in mind that the results aren’t permanent; gravity and age may eventually take their toll once again.
Breast Reduction
For some women, extremely large breasts can cause numerous problems beyond potential dissatisfaction with their appearance. These include neck and back pain, shoulder pain, chafing or rash, significant limitation in your activities and unhappiness with your appearance. Other problems include chronic headaches and even nerve damage.
Psychological issues include depression and stigmatization and poor self-esteem and anxiety. You may also have problems finding clothing that fits. Extremely large breasts, especially in adolescents, can significantly affect a woman’s body image.
The significant emotional and physical repercussions of extremely large breasts mean that some health insurance companies are willing to pay for breast reduction surgery, also called reduction mammaplasty, but some may require that a certain amount of breast tissue be removed. Check your policy, including whether your surgeon needs to write a “predetermination letter.” Although considered “cosmetic” in nature, reduction mammaplasty has functional benefits for the majority of women.
The surgery is considered one of the most rewarding breast operations, with profoundly positive effects on the physical and mental health of women who have unusually large breasts (also called hypermastia). One study found a significant improvement in a woman’s sexual satisfaction if she was satisfied with the results of her surgery.
The procedure is performed on women of all ages, including adolescents whose psychological health is threatened because they are teased about their breast size or are unable to wear typical teenage clothing. Adolescents should be aware that a breast reduction can affect the sensation of the nipple and the areola, and it may impact their ability to breastfeed in the future.
Before deciding on breast reduction, you should undergo a full medical evaluation. If you smoke, your doctor will likely ask you to quit, since smoking can interfere with the healing process. You should also stop taking any herbal supplements and should undergo a mammogram before the procedure.
If you’re overweight, your doctor may recommend that you lose weight before the procedure. There are two reasons losing weight is important before the surgery: the risk of surgical complications increases if you’re obese, and the surgery itself is easier to perform if you’re at your ideal weight. Additionally, excess weight may be contributing to the size of your breasts.
If you want to have breast reduction surgery and plan to breastfeed in the future, talk to your surgeon. In most cases, breast reduction is not recommended for women who intend to breastfeed.
Treatment
Breast Augmentation
The majority of breast augmentations are performed using breast implants, silicone shells filled with saline (sterile saltwater), or cohesive silicone gel.
Silicone gel-filled implants are thought to provide a more natural appearance and are less likely to cause rippling than saline implants. One advantage to saline implants, however, is that the size of some implants can be adjusted during or after surgery by adding saline to the implant.
In 1992, concerned about reports of leaking silicone and possible health implications, the U.S. Food and Drug Administration (FDA) restricted the use of silicone breast implants to controlled clinical studies for women with breast cancer, those whose previous breast implants failed and those with congenital disorders. They were not permitted for women seeking breast augmentation.
Since then, numerous studies have been conducted on the safety and effectiveness of silicone gel-filled breast implants in the United States and around the world and found no increased risk of connective tissue diseases (like scleroderma), autoimmune-related disorders (like lupus and rheumatoid arthritis) or breast or other cancers or neurological disorders in women who have silicone gel-filled breast implants. In late 2006, the FDA approved the use of silicone gel-filled breast implants for cosmetic augmentation.
Silicone gel-filled breast implants are currently approved for breast reconstructive surgery (surgery to rebuild a breast following a mastectomy) in women of all ages and for breast augmentation in women ages 22 and over.
Today’s silicone gel-filled breast implants benefit from improved manufacturing technology and more stringent tolerance specifications, resulting in a more consistent manufacturing process that significantly reduces manufacturing errors. Major changes include thicker shells and more cohesive gel to reduce the risk of rupture and the likelihood that gel will leak into the body if the breast implants do rupture.
In addition, shaped silicone gel implants are now available and may be appropriate for some women. Women considering breast augmentation should discuss the implant options with their board-certified plastic surgeon. Questions remain, however, about silicone gel-filled breast implant rupture rates. To better understand the long-term safety of breast implants, the FDA has required the manufacturers of silicone gel-filled implants to conduct ongoing safety studies.
If you are considering silicone breast implants, discuss the benefits and potential risks with your plastic surgeon.
Surgical procedure for breast implants
During the surgery, breast implants are placed either behind the breast tissue (sub glandular) or behind the chest muscles (submuscular or subpectoral). The former is primarily used in women with enough breast tissue to cover the implant and in athletic women; the latter in women with smaller breasts. The decision regarding optimal placement of the implant is made by the surgeon with patient input. The surgery is performed under general or local anesthesia combined with a sedative in a hospital, office or outpatient surgical setting. In many instances, you can go home that same day.
Several surgical approaches are available:
- Inframammary. The surgeon makes the incision in the fold underneath the breast. This is the most common incision used in augmentation and is ideal for women whose breasts sag a bit since the natural droop of the breast hides the incision.
- Trans-axillary. The incision is made in the armpit, enabling the physician to place the implant behind the chest muscle. It is more commonly used in patients who have not had a pregnancy or whose areolas are small. However, the scar is visible under the arms and may even be seen when wearing sleeveless clothing.
- Trans-umbilical breast augmentation (TUBA). This is the newest form of breast augmentation incision. The incision is made through your belly button. Then the surgeon “tunnels” up through your chest area to a pocket under the breast or under your chest muscle with the deflated implant. Once the implant is placed, it is inflated with the saline solution. This procedure has a faster recovery time and less scarring, although there is a greater risk of damage to the implant itself. Because prefilled silicone implants are too large to fit through the navel, TUBA can only be used with saline implants.
- Peri-areolar. The surgeon inserts the implant through an incision around the nipple. Although this form can interfere with your ability to breastfeed, recent studies find that nipple sensation is typically not affected.
Breast Implant Complications
A 2013 study published in the journal of the American Society of Plastic Surgeons, called Plastic and Reconstructive Surgery, found that 10 percent of women who underwent breast augmentation surgery suffered complications. One of the most common complications is when scar tissue forms around the implant, causing it to thicken and contract.
This process is known as capsular contracture and can sometimes lead to rupture or deflation of the implant and requires additional surgery. The risk of capsular contracture, however, is lower when the breast implant is placed in the submuscular position. It is important that you understand that, similar to other medical devices, breast implants are not lifetime devices, and it is likely that at some point they may need to be removed or replaced.
Other possible complications include:
- Deflation. This risk is specific to saline breast implants and is greatest for breast implants placed under the muscle.
- Rupture. This risk is rare, but breast implants can rupture in some cases. A large number of studies have concluded that a ruptured implant (saline and/or silicone gel-filled) has no long-term impact on a woman’s health.
- Infection
- Changes in nipple/breast sensation
- Breast pain
- Hematoma, a collection of blood in the breast that must be drained
- Displacement or migration. This may occur over time as the implant space may sometimes expand.
Many of these complications can be prevented with the method of insertion and by using antibiotics before, during and after the surgery, even infusing them into the breast cavity with the breast implant. If you suspect any of these complications, you should consult your plastic surgeon.
Despite the risk of complications and additional surgeries, most women who get breast augmentation are happy with the outcome. The 2013 study published in Plastic and Reconstructive Surgery found that 98 percent of women who had undergone breast augmentation surgery said the procedure met or exceeded their expectations.
After Breast Implant Surgery
Breast augmentation surgery includes a recovery period of about 24 to 48 hours, as well as a few days of reduced activity. After your surgery, you will wear a special bra to prevent the breast implants from moving. You’ll likely experience more pain with a subpectoral placement than a sub glandular placement and may need a week or more off of work to recover. You will be able to resume exercise and normal activities at the direction of your surgeon. Expect to return to all of your normal activities within a month to six weeks.
Mastopexy (Breast Lift)
A mastopexy, or breast lift, is a less intensive operation than a full breast augmentation. Most are performed in an outpatient setting, either in a hospital, your plastic surgeon’s in-office operating suite or a freestanding outpatient surgery facility, usually under general anesthesia. The procedure itself usually takes less than two hours. In some women, a mastopexy can be performed at the same time as an augmentation. Combining the procedures may pose additional risk, and those risks must be understood.
There are several surgical procedures your plastic surgeon may choose from for your mastopexy, but all involve the same major components: removing excess skin, repositioning the nipple and areola (the dark part of the breast surrounding the nipple) and ensuring a minimum of scarring. Scars may be located around the nipple-areolar complex and/or at the base of the areola extending to the lower breast fold.
Complications of Breast Lift Surgery
Complications include bleeding and infection and problems related to the anesthesia, although these are relatively rare. You will also have permanent scars, although they will be covered by your bra or bathing suit. You may find that your nipples are unevenly placed, and you may lose some sensation in your nipples or breasts.
After Surgery
After mastopexy, you’ll need to wear an elastic bandage or surgical bra over gauze dressings as your breasts heal. They’ll be bruised, swollen and sore for a few days. The stitches are usually dissolvable but, if they are not, they will be removed after a week or two. After that, you can wear a soft support bra over a layer of gauze for several weeks. You may experience some loss of sensation around your nipple area, but that usually fades over time.
Breast Reduction Surgery (Reduction Mammoplasty)
Several surgical procedures can be used for breast reduction surgery. The one that’s best for you depends on several factors, including your medical history, size and shape of your breasts, desire to breastfeed and your surgeon’s skill.
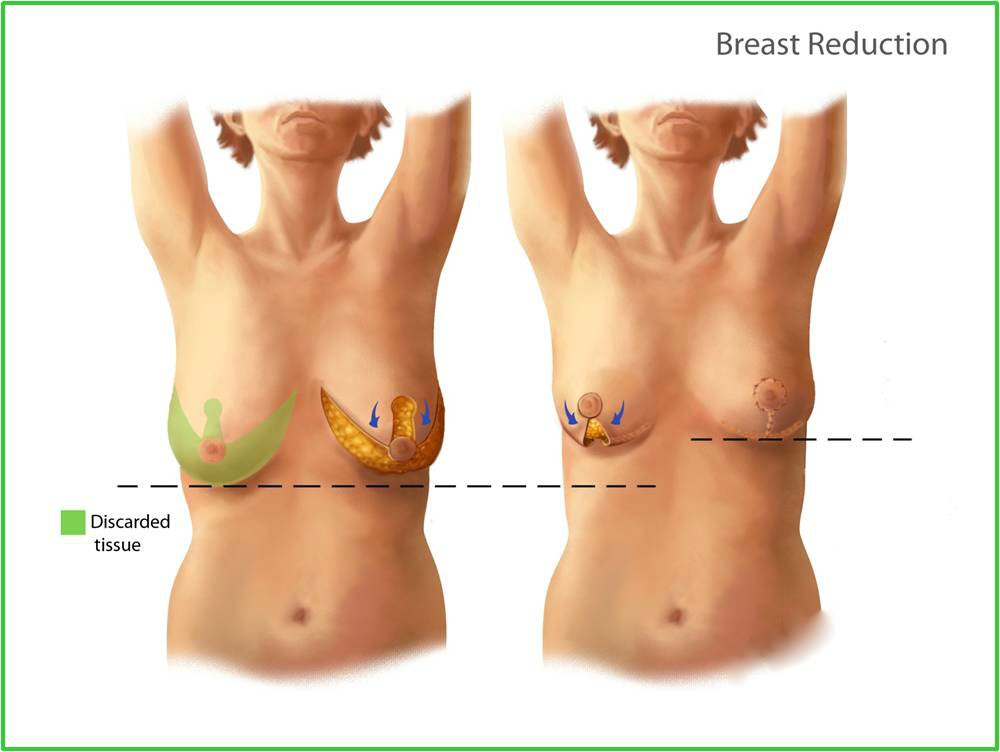
The most common procedure, according to the American Society for Aesthetic Plastic Surgery (ASAPS), is one in which the plastic surgeon makes an anchor-shaped incision around the areola downward, following the natural curve of the crease beneath the breast. The doctor then removes excess fat and tissues, repositions the nipple and areola higher, and reshapes the breast. The major disadvantage of this procedure is scarring.
For women who need only moderate reduction, a vertical or short scar technique may be used. With this technique the horizontal or inframammary scar is avoided. The scars are located only around the areola and down the vertical midline.
For some women who require only a small reduction or a redo of a breast reduction, liposuction may be considered. In this procedure, the surgeon uses a special tool to remove the fat and tissue from the breast without cutting and stitching, leaving minimal scars. Most breast reduction surgery is performed under general anesthesia in a hospital or office-based surgical unit. You can usually go home the same day or, at the most, may require an overnight hospital stay.
Ask your doctor to examine the removed breast tissue for any abnormalities. Examining the removed tissue may help identify any cancerous or precancerous changes.
Complications
While breast reduction surgery is a common and relatively safe procedure, there are some risks and possible complications. The primary risks include bleeding and infection. Most plastic surgeons will insert a drain tube for a couple of days and will prescribe antibiotics for a few days. Some women may experience changes in the sensitivity of their breasts and nipples. If the blood supply is reduced, the nipple area or other areas of skin may slough off. Other complications include fat necrosis or lumpiness in the breast.
Breast reduction may also be associated with an inability to breastfeed because some of the ducts leading to the nipple may be cut during the operation. There may be delayed healing or minor differences between breasts following the operation. One way to reduce your risk of complications is to quit smoking. One study found the risk of complications after breast reduction surgery was three times higher in smokers than nonsmokers. Although revisions are not common, they may be necessary in some women following breast reduction surgery.
After Surgery
After the surgery, you usually wear a postsurgical bra over gauze dressings for four weeks and shouldn’t lift anything heavy during that time. You may also have some drainage tubes in your breasts for several days or even weeks. While it may take up to six months for your breasts to return to normal, you will probably be able to resume your normal activities within several weeks.
1. Implants don’t last forever.
Breast augmentation isn’t one-and-done. It’s the first thing that plastic surgeon Nolan S. Karp, MD, tells women who come to him for implants.
“Most companies guarantee their implants for 10 years, though they hardly ever need to be replaced that often,” Karp says. “I tell my patients that implants usually last at least 15 years. So depending on your age, you usually have to anticipate a couple more surgeries.”
Plan to schedule a yearly exam with your plastic surgeon to make sure your implants are strong and intact.
2. But breast reduction usually does last.
How long your results hold up depends on your breasts.
There are three types of breast tissue: fatty, fibrous, and glandular. It’s really unlikely that you would develop more fibrous or glandular tissue after surgery.
“I’ve probably done more than 2,000 breast-reduction surgeries, and 99% of the time, the tissue doesn’t grow back,” Karp says.
There’s a big exception. If you gain weight after the surgery, you could develop more fatty tissue in your breasts. That’s why it’s ideal to get breast reduction surgery when your weight is steady, Hansen says.
3. There are different types of breast implants.
Some women still get saline ones, which your surgeon puts into your breast empty and then fills with sterile salt water. But many others now get silicone implants, which come prefilled with silicone gel.
There are also different types of silicone implants. Some are soft. Others are “form-stable.” Some people call those “gummy bear” implants because they keep their shape even if the spell is broken. Form-stable implants are fuller at the bottom, which may look more natural. But unlike round ones, they can distort the breast’s natural shape if they rotate.
Which type should you choose? “Your surgeon will look at your anatomy and help you decide which type is right for you,” Karp says.
4. There are different techniques.
To insert the implant, your surgeon will make a single cut in one of three places:
- In the crease under your breast
- Under your arm
- Around your nipple
The type of cut you choose depends on the type of implant you get, your anatomy, and your personal preference. Afterward, the surgeon will close the cut with stitches and bandage it.
“You’ll have scarring with all three incisions, but we try to hide the scars underneath the breast, in the fold of the armpit, or right where the dark-colored skin around your nipple meets the skin of your breast [the areola] so it won’t be as visible,” Karp says.
With breast reduction, the surgeon usually makes a cut around the areola in a circular, keyhole, or upside-down T-shaped pattern. Though the cut lines are permanent, they’ll fade over time.
5. Qualifications count.
“It’s really important that your surgeon is board-certified in plastic surgery,” Hansen says. “A lot of doctors want to get into breast surgery even though that’s not their specialty.”
If you decide to set up a consultation, ask the doctor if they’re certified by the American Board of Plastic Surgery. That requires at least 5 years of training as a surgeon, including at least 3 years devoted to plastic surgery specifically.
Also ask how many years of plastic surgery training the surgeon has gotten.
6. Your life should go back to normal pretty quickly.
If you get breast augmentation, you can usually go home the same day.
“It’s really rare for an implant procedure done for cosmetic purposes to require an overnight stay,” Hansen says.
Plan ahead for someone to drive you home after the operation and stay with you for at least 1 night. Your breasts might feel stiff or sore for up to 5 days, and you should skip physical activity for a few weeks.
After breast reduction surgery, your doctor may ask you to wear an elastic bandage or special bra to minimize swelling. She may also place a temporary tube under your skin to drain blood or fluid.
Should you choose to breastfeed after breast enlargement surgery, “there’s no reason why you couldn’t,” Hansen says. But breast reduction may affect your ability to breastfeed, so talk to your doctor if you plan to nurse.
Facts to Know
- According to the American Society for Aesthetic Plastic Surgery in 2012 more than 10 million cosmetic surgical procedures were performed in the United States.
- In 2012, a total of 110,438 breast reductions were performed (including both reconstructive and cosmetic procedures), according to the American Society of Plastic Surgeons.
- Whether you choose to have your breasts increased in size, lifted or reduced in size, it’s important that you choose the right plastic surgeon. Your plastic surgeon should be board certified by the American Society of Plastic Surgeons, have privileges at a local hospital and be trained in the technique you’ve chosen.
- Most women opting for breast surgery are young and healthy; however, a full medical evaluation is still required. For instance, if you smoke or are overweight, your health care professional may counsel you to quit smoking and/or lose weight, both of which reduce the risk of complications from surgery.
- Very few insurance companies cover breast augmentation or breast lift for cosmetic reasons, and national average costs for the surgeon’s fee alone are $3,543. You’ll also have to pay for the operating room, postsurgical hospital stay, anesthesia and related costs. However, the significant emotional and physical repercussions of large breasts mean that many health insurance companies are willing to pay for breast reduction surgery even though it’s still considered a “cosmetic” surgery. Check your policy, including whether or not your plastic surgeon needs to write a “predetermination letter.”
- There are two types of breast implants, silicone shells filled with saline or sterile salt water or silicone gel. Silicone gel-filled breast implants are thought to provide a more natural appearance, and they’re less likely to deflate.
- During breast augmentation surgery, the breast implants are placed behind the breast tissue (called subglandular), primarily in women who have enough underlying fat to cover the implant, or behind the chest muscles (called submuscular).
- Breast implants carry a relatively low risk of complications early on but with time, complications may increase.
- Similar to other medical devices, breast implants—saline or silicone—are not lifetime devices. It is likely that at some point they may need to be removed or replaced. If your breast implants need to be replaced or removed, you’ll be responsible for covering the costs of the surgery.
- The American Society of Plastic Surgeons notes that the best candidates for mastopexy (“breast lifts”—surgery that lifts sagging breasts) are healthy, emotionally stable women with realistic expectations of what the procedure will accomplish, particularly women with small, sagging breasts. If you haven’t finished childbearing, the ASPS recommends you wait. Another pregnancy and breastfeeding may stretch your breasts again, although the procedure doesn’t affect your ability to breastfeed.
Key Q&A
- What are the three major types of cosmetic breast surgery?
- Breast augmentation, in which a silicone shell implant filled with either silicone gel or sterile saline solution is used to make the breast larger
- Breast lift, or mastopexy, in which implants and/or surgery are used to remove the droopiness and sagging of the breasts
- Breast reduction, in which fat and tissue are removed to make large, heavy breasts smaller
- Will health insurance cover the costs of breast surgery? Health insurance only covers the cost of breast reconstructive surgery after mastectomy to prevent or treat breast cancer or to correct a deformity or the cost of breast reduction if you can demonstrate health-related problems because of your large breasts. (Many factors determine your eligibility for coverage, including specific terms of your health care policy and the amount of breast tissue that will be removed.) Otherwise, you are responsible for all costs. Breast implant manufacturers and cosmetic surgeons may offer credit plans that allow you to pay for the procedure over time.
- Who is the best candidate for breast surgery?A healthy woman who doesn’t smoke and isn’t overweight and who understands the pros and cons of the procedure. All surgical procedures have risks—even in the hands of a very good surgeon. Additionally, you should have realistic expectations. Your breasts may not be perfectly even, there may be scarring and additional surgeries may be required.
- Can I still breastfeed after breast surgery?In most instances you can. However, if you’re planning to have a child and want a breast lift, you should wait until after you’ve finished having children and breastfeeding, because pregnancy and nursing may make the breasts sag again much quicker than the passage of time alone. Also, breast reduction is not recommended for women who intend to breastfeed.
- Will implants affect my mammograms in the future? While it is safe and recommended to have a mammogram with breast implants, you should ask your physician to direct you to a screening facility that offers a specialized technique that has been shown to improve the accuracy of mammograms in women with breast implants.
For more information visit us our website: https://www.healthinfi.com
0 200

Fantastic Site. Very much enjoyed reading.