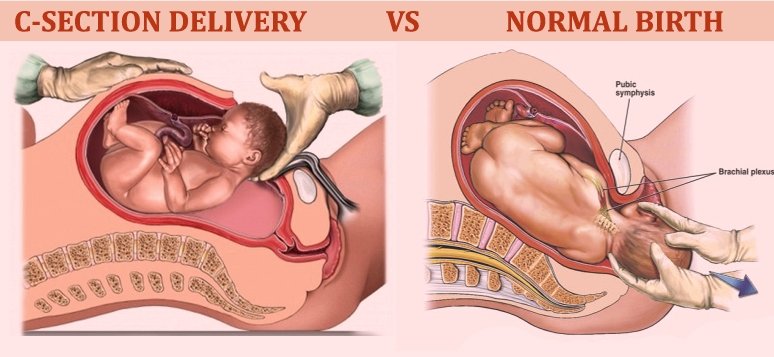
Vaginal Birth vs. C-Section
While in most cases vaginal delivery is the most natural and uncomplicated way to deliver a baby, more and more women are opting for Cesarean Sections.
Today C-sections make up about 30% of all births. Since every woman can choose how they would like their delivery, it is important to understand the risks and advantages of both options. Here are the pros and cons for natural birthing and c-section deliveries.
Why bother going through the process of giving birth vaginally when you can have a planned caesarean section? Increasing numbers of women today appear to be subscribing to this view. Maternal request for delivery by caesarean section is reportedly on the increase and has been blamed, in part, for the continuing rise in the caesarean section rate.
The level of maternal request is a controversial issue. The National Sentinel Caesarean Section Audit report notes that studies report rates of maternal request ranging from 1.5% to 48%. Much of the variation is due to unclear definitions of ‘maternal request’ and whether there was also a supporting clinical indication.
But the use of ‘maternal request’ as a reason for carrying out surgery is a non-sense, since it simply indicates who instigated the decision. Clinical indications are not, after all, lumped together under ‘obstetric preference’. Until audits standardise the terminology and sub-divide ‘maternal request’ into the underlying reasons why women prefer to undergo surgery, serious debate of the issue will be hampered.
Regardless as to the actual level of maternal request and the methods used to quantify it, there is no denying it is very much an issue of our time.
The amount of media coverage and the frequency with which ‘maternal request’ is cited as a barrier to the reduction of caesarean rates, demonstrate that this issue is of concern to a great many, both in the childbirth world and our society as a whole.
Why Has Caesarean Section Apparently Become More Popular? Since the dawn of time labour and birth through the vaginal passage have been an inevitable consequence of pregnancy, a journey through to life.
There was no alternative to vaginal birth, except death. In this new millennium, women do have an alternative, one that has been provided by the wonders of modern technology – women today have choice, something that women in ages past did not have.
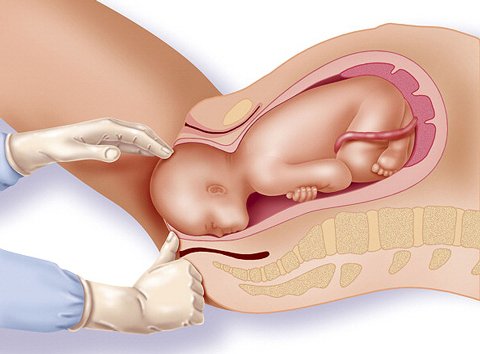
Vaginal Delivery Pros
- This is the more natural way to give birth. Your body is naturally equipped to give birth vaginally without medical intervention. Labor starts with your cervix dilating, and it ends with a newborn baby.
- Women have a sense of empowerment and accomplishment after a vaginal birth. They are active participants in the childbirth experience. They must push to help move their baby through the birth canal and into the world.
- Shorter hospital stay after a vaginal birth. (You are in the hospital for 24 to 48 hours after delivery).
- You have a quicker recovery time with a vaginal birth, and you will have less postpartum pain.
- Your baby is less likely to have certain respiratory problems, including transient tachypnea of the neonate, or TTN, (fluid in the newborn’s lungs). TTN is not serious and it clears up within 2 to 3 days of treatment. It is more common in premature babies and full-term infants born via c-section.
- Vaginal deliveries reduce the likelihood of TTN, because the pressure of going through the birth canal helps squeeze this extra fluid from your baby’s lungs. Also, natural labor triggers the release of the hormone epinephrine, which clears fluids from the lungs.
- Infants born vaginally are also at decreased risk of persistent pulmonary hypertension – a condition in which your baby’s organs are deprived of oxygen because blood is not flowing into the lungs like it should.
- Infants born vaginally are less likely to develop asthma, food allergies, and lactose intolerance later in life. This may be due to being exposed to beneficial bacteria in the birth canal.
- In future pregnancies, labor may be shorter and move along quicker.
- Mothers who deliver vaginally are able to breastfeed immediately and more effectively, than women with c-sections.
- After a vaginal birth, it may be easier to bond with your infant because you can have immediate contact with him or her.
- You are at a decreased risk of maternal hemorrhage, blood clots, and damage to your internal organs.
Vaginal Delivery Cons
- Fear of childbirth may cause anxiety and emotional turmoil for some women.
- Though most vaginal births are uncomplicated, unforeseen complications can occur during labor and delivery, including maternal hemorrhaging (bleeding).
- You are at risk for perineum tearing from a vaginal delivery. This can range from mild tears to fourth-degree lacerations that tear into your rectum. This can add to your healing time.
- Your baby faces the risk of oxygen deprivation, if there are cord compression or other problems during labor and delivery.
- Your baby may experience physical trauma while passing through the birth canal, including bruising, swelling, and in rare cases broken bones. The risk of physical trauma increases in an assisted vaginal delivery (forceps or vacuum extraction).
- Vaginal deliveries may increase your likelihood of pelvic organ prolapse after delivery (one of your pelvic organs drops from its original location and protrudes into your vaginal canal).
- In very rare cases, uterine inversion can occur after a vaginal birth. This is a life threatening complication that occurs when the top of your uterus turns inside out. If not treated immediately, this can lead to severe hemorrhage (bleeding) and shock and it may result in death of the mother.
- If you experienced a tear or episiotomy, you may have pain after intercourse for the first three months following your baby’s birth.
- You can sometimes injure your tailbone during childbirth. These injuries are uncommon, but you are more likely to bruise, dislocate, or fracture your tailbone if you have a narrow or unusually shaped pelvis and if you are delivering a large baby.
- Women with vaginal deliveries have higher rates of urinary incontinence (urine leaks) than women with c-sections. Having an assisted vaginal delivery, prolonged pushing stage, and having a large baby increases your risk.
Cesarean Section
A cesarean section is a common surgical procedure performed on pregnant women who cannot safely give birth the natural way. These can be planned in advance or become necessary due to complications during labor.
If the baby has a fetal illness, an abnormality, a large fetus, or is in non-vertex fetal position, a cesarean section may be required. Other complications that could necessitate a cesarean section include displaced placenta, mother or child distress, halted labor, non-dilated cervix, compressed umbilical cord, and oxygen cutoff to the baby.
The procedure involves making a horizontal incision in the lower abdomen through which the baby is lifted out. The umbilical cord is cut and the fetal membranes are removed. The surgeon will then stitch the uterus and abdominal wall closed. In most cases, Dr. Ayalon will use spinal anesthesia, which will cause the patient to not feel any pain. If the situation is an emergency, general anesthesia may be used.
Those that have received a cesarean section usually need to spend additional time in the hospital to recover. It’s important to stay active, but lifting should be kept to a minimum.
Planned Cesarean Section Pros
- Planned cesarean sections (c-section) may be more convenient for women. Because the baby’s delivery date is usually scheduled ahead of time, mom may have less stress and anxiety about labor.
- Women may feel more in control, because they know when their baby will be born and they can better plan for work leave, their baby’s nursery, etc.
- You can avoid post term pregnancies with a planned c-section. Most c-sections are typically scheduled between 39 or 40 weeks of gestation.
- When compared to a vaginal delivery and an unplanned c-section, scheduled cesareans have a reduced risk of postpartum hemorrhage. Uterine atony (the uterus does not contract normally after the baby and placenta are delivered), which is the most common cause of postpartum hemorrhage, is minimized in a planned c-section.
- Compared to emergency c-sections, a planned cesarean has slightly lower risks of complications, including infection, accidental injury to abdominal organs, lacerations to the baby, and anesthesia-related problems.
- If you have an STD or infection (such as herpes, HIV, hepatitis, and HPV), your risk of infecting your baby is greatly reduced with a cesarean section.
- You are at lower risk of birth trauma that occurs in a vaginal birth, such as swelling or bruising.
- You may be at decreased risk for pelvic floor injury. Women with planned cesareans have fewer cases of urinary incontinence (inability to hold urine) in the weeks following birth. However, the urinary continence two and five years after delivery was not different between the two groups.
Planned Cesarean Section Cons
- A c-section is a major abdominal surgery that comes with surgical risks and complications from anesthesia. Anesthesia side effects may include severe headache, nausea, and vomiting. Anesthesia may also affect the baby, causing him or her to be sluggish or inactive when born.
- Women with planned cesarean sections have longer hospital stays and a longer postpartum recovery period than women with vaginal deliveries
- In a planned cesarean delivery, you face possible pre-term delivery if your estimated due date was not correct.
- In a complicated c-section, you face a risk of the surgeon accidentally cutting your bowels or bladder.
- You lose more blood in a cesarean section than a vaginal delivery. Two to three percent of women who undergo c-sections require a blood transfusion. You lose approximately 1,000 mL (or 1 liter) of blood with a c-section.
- You may have decreased bowel function after a cesarean.
- Respiratory problems are more common in babies delivered via c-section. Problems include transient tachypnea of the neonate (TTN) and respiratory distress syndrome.
- Some research has indicated that the odds of neonatal death (your baby dies in the first 28 days of life) are higher in a planned c-section than with a vaginal birth.
- If you plan on having a larger family, you may want to think twice about a planned cesarean section. After one or more c-sections, in future pregnancies, you are at increased risk for developing placenta previa (your placenta grows low in your uterus and covers either partially or fully the opening of the cervix) and placenta accreta (the placenta embeds itself too deeply into the wall of your uterus).
- Having a previous cesarean increases your risk of uterine rupture (a tear in the wall of uterus, which commonly occurs at the site of the c-section incision).
- Breastfeeding is more difficult after a cesarean delivery. Women are uncomfortable after surgery, and they do not have immediate contact with their baby.
- Occasionally, your baby may be nicked or cut by the doctor’s scalpel during a cesarean section. Most often, these are very mild cuts.
- C-section babies are at higher risk for persistent pulmonary hypertension.
- Your baby faces a risk of having a lower Apgar score (a test that is designed to evaluate your baby’s physical condition immediately after delivery).
- An elective cesarean is more expensive than a vaginal birth. Not all insurance carriers cover planned c-sections.
- Heart attacks
- Wound hematoma – mass of clotted blood underneath the site of the c-section incision
- Puerperal endometritis infection – inflammation of the tissue lining your uterus that is caused by a bacteria infection
- Blood clots in the veins
- Hemorrhage (bleeding) that requires a hysterectomy (surgical removal of the uterus)
- Opening of the wound
- Numbness or pain in the area around the scar
- Postpartum infection
For more information visit us our website: https://www.healthinfi.com



No Comments