Doctors regularly implore women over age 50 to take more calcium to reduce their risk of osteoporosis and hip fractures. But they might not need as much as they think. And taking too much calcium can actually cause other health problems.
A huge study in the British Medical Journal, which followed 61,000 Swedish women for 19 years, found that their bones got no benefit when they consumed more than 750 milligrams of calcium a day.”It’s good news for women who are trying really hard to get a lot of calcium a day,” says Eva Warensjo, an epidemiologist at Uppsala University in Sweden, who was lead author on the study.
But doctors in the United States have been saying pretty much the same thing for years. In 2006, a study done as part of the ongoing Women’s Health Initiative found only slight increases in bone mass and no significant differences in the number of broken hips in women taking 1,000 milligrams of calcium a day, compared to women who did not take supplements.
“More is not necessarily better,” says JoAnn Manson, a researcher at Harvard University and Brigham and Women’s Hospital in Boston, and a principal investigator in the WHI. “Moderate intake may be optimal there may be a threshold effect where once you get to a moderate level of intake there’s no further benefit.”
In fact, taking more calcium could be worse than just worthless. It could cause other health problems, such as kidney stones. Recent research has suggested a link between excess calcium and cardiovascular problems.
Last year, the Institute of Medicine recommended that women over 50 should aim for 1,200 milligrams a day, whether or not they have signs of bone loss. That is higher than the amount recommended in Sweden and other European countries. Manson helped write that report, and she’s not ready to say that number is too high.
Still, that doesn’t mean that women need 1,200 milligrams from supplements, Manson says. “On average, 700 milligrams a day would come from diet.” That’s also about what the Swedish women, who are big consumers of sour milk and other dairy products, get from food.
So, most American women are getting as much as the Swedish study recommended without taking any calcium supplements. But many people haven’t gotten that message. John Tongue is an orthopedic surgeon in Portland, Ore. who’s also the first vice president of the American Academy of Orthopedic Surgeons.
He’s been operating on women with hip fractures caused by osteoporosis for more than 30 years, so he knows how devastating a broken hip can be. When this new study came out, he asked his wife how many calcium supplements she’s taking. He found out that she was taking 1,400 milligrams in supplements.
But she’s also exercising, which Tongue thinks is more important than calcium for keeping bones strong. “A brisk walk for 20 to 40 minutes a day would do much more to improve people’s general health and reduce people’s risk of injury than taking vitamins or supplements, which are so common,” says Tongue.
The Supplement Situation
I’ve tried taking calcium supplements, but I prefer to get my nutrients through my diet. Studies show that high levels of calcium from supplements can increase risk of kidney stones (ouch!), while dietary calcium may offer some protection against stones. Even scarier, one study of postmenopausal women showed that women who took 1,000 milligrams of calcium a day had an increased heart attack risk.
Studies also show that calcium isn’t properly utilized by the body unless we get ample vitamin D. And, vitamin D can be tricky to get through diet alone. The current daily recommendation for vitamin D is 600 IU (800 IU for people over 70).
Some foods, like milk, are fortified with vitamin D, but the best source is sunlight. However, unless you live where it’s sunny year-round and you get out and expose your skin to sunlight for about 20 minutes a day (without sunscreen), then you may come up short. To make things tougher, our skin’s ability to convert sunlight to vitamin D gets worse with age (what doesn’t?).
Alternative Recommendation
That’s why the recommendation from Harvard University’s Dr. Walter Willett comes as good news to me. Willett, chair of the Department of Nutrition at Harvard T.H. Chan School of public health, says we may only need about half as much calcium as current guidelines recommend for healthy bones.
He suggests 500 to 700 milligrams of calcium a day, in line with the World Health Organization’s recommendation of 500 milligrams and the United Kingdom’s goal of 700 milligrams. Willett maintains that most women could get at least half of that through diet and, if necessary, could supplement with a low-dose calcium supplement.
In the Health Watch article, he summarizes the scant evidence on which the current U.S. recommendation is based and cites recent studies that show that calcium and vitamin D supplements don’t prevent fractures and that calcium (from diet or pills) doesn’t reduce risk of hip fractures. Along with the decrease in calcium requirements, Willett suggests an increase in vitamin D intake to 800 to 1,000 IU a day.
As with calcium, the debate continues about proper levels of vitamin D. A recent University of Wisconsin School of Medicine study showed little value from high-dose vitamin D supplements. In that study, the groups of women who received high-dose or lose-dose vitamin D showed no advantage over women who received no supplements when it came to spine health, total bone mineral density, overall muscle mass, physical mobility or overall fall risk.
With so many conflicting studies, clearly more research is needed.
Even though the government recommendations have not changed, I feel some relief in knowing that my diet may be providing enough calcium hopefully just the right amount for strong bones and no stones.
Why the 1,200-mg recommendation?
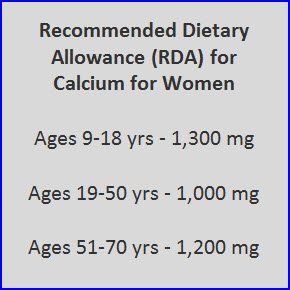
Adequate calcium is necessary for good health, and not just because it’s a major component of our bones. It also plays a vital role in keeping our organs and skeletal muscles working properly. The body gets the calcium it needs for basic functions by releasing the calcium stored in our bones into the blood through bone remodeling—the process by which bone is constantly broken down and rebuilt.
Because bone density drops when bone breakdown outpaces bone formation, scientists reasoned that maintaining an adequate level of calcium in the blood could keep the body from drawing it out of the bones. In the late 1970s, a couple of brief studies indicated that consuming 1,200 mg of calcium a day could preserve a postmenopausal woman’s calcium balance.
Based on those studies, in 1997 an Institute of Medicine panel raised the recommendation for calcium intake from 800 mg to 1,200 mg a day for women over 50.
That wasn’t a sound decision, Dr. Willett says: “The recommendation was based on calcium balance studies that lasted just a few weeks. In fact, calcium balance is determined over the course of years.” Moreover, there wasn’t any evidence that consuming that much calcium actually prevented fractures. Nonetheless, the recommendation has been carried forward since then.
What recent research has found
In the past two decades, several clinical trials involving thousands of postmenopausal women have sought to determine how calcium intake affects the risk of hip fractures. In each study, women were randomly assigned to one of two groups one to receive calcium and supplements of vitamin D (to aid calcium absorption) and the other to get placebo pills. After several years, the researchers looked at the number of hip fractures in each group. Here’s what they found:
Calcium and vitamin D supplements don’t prevent fractures.
That finding came from two British studies reported in 2005. It was substantiated by a 2006 report from the Women’s Health Initiative, which showed that 18,000 postmenopausal women who took a supplement containing 1,000 mg of calcium and 400 international units (IU) of vitamin D were no less likely to break their hips than an equal number who took a placebo pill, although the density of their hip bones increased slightly. Even that small change might have been due to the vitamin D rather than the calcium.
High calcium intake—from either food or pills—doesn’t reduce hip fracture risk.
This was the conclusion of a 2007 report by Swiss and American scientists who conducted an analysis of more than a dozen studies of calcium.
| 25 sources of dietary calcium | ||
| Produce | Serving size | Estimated calcium in milligrams |
| Collard greens, frozen | 8 oz | 360 |
| Broccoli rabe | 8 oz | 200 |
| Kale, frozen | 8 oz | 180 |
| Soy Beans, green, boiled | 8 oz | 175 |
| Bok Choy, cooked, boiled | 8 oz | 160 |
| Figs, dried | 2 figs | 65 |
| Broccoli, fresh, cooked | 8 oz | 60 |
| Oranges | 1 whole | 55 |
| Seafood | Serving size | Estimated calcium |
| Sardines, canned with bones | 3 oz | 325 |
| Salmon, canned with bones | 3 oz | 180 |
| Shrimp, canned | 3 oz | 125 |
| Dairy | Serving size | Estimated calcium |
| Ricotta, part-skim | 4 oz | 335 |
| Yogurt, plain, low-fat | 6 oz | 310 |
| Milk, skim, low-fat, whole | 8 oz | 300 |
| Yogurt with fruit, low-fat | 6 oz | 260 |
| Mozzarella, part-skim | 1 oz | 210 |
| Cheddar | 1 oz | 205 |
| Greek yogurt | 6 oz | 200 |
| American cheese | 1 oz | 195 |
| Feta cheese | 4 oz | 140 |
| Cottage cheese | 4 oz | 125 |
| Fortified food | Serving Size | Estimated calcium |
| Almond milk, rice milk or soy milk, fortified | 8 oz | 300 |
| Tofu, prepared with calcium | 4 oz | 205 |
| Orange juice fortified with calcium | 4 oz | 150 |
| Cereal, fortified | 8 oz | 100-1,000 |
| Source: International Osteoporosis Foundation | ||
The downside of calcium supplements
The studies also revealed a couple of downsides to high levels of calcium supplementation, but not to calcium obtained through a regular diet:
An increased risk of kidney stones.
In the Woman’s Health Initiative, women taking the calcium–vitamin D combination had a higher risk of developing kidney stones than those who got the placebo. Although high levels of dietary calcium are thought to offer some protection against kidney stones, high doses of calcium from supplements may promote stone formation by increasing the amount of calcium that is eliminated in the urine.
An increased risk of heart attack.
In a randomized study of 1,471 postmenopausal women conducted in New Zealand, 21 of 732 women who took 1,000 mg of calcium a day had heart attacks, compared with 10 of 736 who received a placebo. A 2010 analysis of 15 randomized controlled trials also linked calcium supplementation with an increased risk of heart attack. Some researchers have speculated that calcium supplements may contribute to heart disease by increasing blood levels of calcium, which can cause arteries to stiffen and blood pressure to rise.
Vitamin D is important, too
Vitamin D is also essential for healthy bones. In fact, the daily vitamin D requirement was first introduced to help prevent rickets a condition in which developing bones are soft and can become bowed in children.
Vitamin D is made in the skin through exposure to ultraviolet radiation in sunlight. However, the amount produced varies widely from person to person. People with darker skin produce less vitamin D than lighter-skinned people, and in all populations, the skin’s ability to convert sunlight to vitamin D declines with age.
Plus, if you follow the advice to reduce your risk of skin cancer by keeping covered and wearing sunscreen, you’re also cutting your vitamin D production. Such variability has made it difficult for researchers to tell how much vitamin D people make in addition to the amount they consume in supplements. Evidence from studies that have measured blood levels of vitamin D indicates that levels in the high-normal range are optimal for building bone. To reach those levels may require taking 800 to 1,000 IU of vitamin D a day.
What’s the bottom line?
One thing the studies have taught us is that both calcium and vitamin D are essential in building bone. The question is how much of each. Dr. Willett recommends going lower on calcium and higher on vitamin D than the guidelines suggest 500 to 700 mg a day of calcium and 800 to 1,000 IU of vitamin D.
At that rate, you can probably get all or most of your calcium from food, especially if you have a serving or two of dairy products daily. If you can’t tolerate dairy, you should still be able to get 300 mg a day in your diet and can take a low-dose calcium supplement to make up the rest. By keeping your supplement consumption to 500 mg or less a day, you should avoid the possible risk of heart disease and kidney stones suggested by the studies.
Although vitamin D is added to milk and some other foods, you’ll probably need a supplement to be sure you’re getting enough. A capsule containing 800 to 1,000 IU should do the trick.
More Questions
Q-1: What’s the real deal on calcium? How much do I need? Are soy, coconut, or almond milk just as good sources of calcium as skim milk?
A-1:
Calcium’s main role in the body is in the building and maintaining strong bones. Calcium also plays an important role in many processes in your body, such as muscle contractions, blood clotting, and nerve signaling. Several years ago there was a lot of buzz surrounding calcium and weight loss, but in the end, eating more calcium did not turn out to be a key factor in accelerating fat loss.
How much to you need? 1000 mg per day. Women older than 50 need a little more (1200 mg per day).
When most Americans think of calcium, they think of milk and dairy products. Either due to a intolerance to lactose (a sugar in milk), an allergy to casein (a milk protein), or just a dietary choice not to consume dairy products, achieving the daily recommended calcium intake through milk and dairy products isn’t possible for many people. There are other dietary sources of calcium, but how do they stack up? Here’s a table to show you:
Q-2: “How much extra calcium should I be taking?”
A-2:
It’s a question I get several times a day from women of all ages, but mostly from those in menopause or nearing menopause.
The answer I almost always give is “less than you think.” And for most women, probably none.
It’s not that I don’t think calcium is important.
It is. Adequate calcium and vitamin D are critical for building and maintaining a healthy bone mass.
But most women, with the exception of those who can’t tolerate dairy, are already getting a significant amount of calcium in their diet. So much so that taking calcium supplements adds little to their overall health.
In fact, the U.S. Preventive Services Task Force recently recommended against routine calcium and vitamin D supplements for healthy postmenopausal women.
What harm can a little extra calcium do me?
More than you might think. Too much calcium can lead to:
-
Kidney stones
-
Constipation (If constipation is a problem for you, try taking calcium with magnesium)
-
Trouble absorbing iron and zinc
You may also have heard that taking calcium supplements can lead to heart disease. It’s still an open question. Some studies suggest up to a 20% increase in heart disease in men and women who take calcium supplements, but other studies do not find this risk, or find it only in men and not women.
Q-3: How much calcium do women really need?
Does it change as we get older? Will it really help build strong bones and prevent fractures? Are supplements helpful? I’ve wrestled for many years with these and other questions related to calcium and vitamin D, the vitamin that aids calcium absorption. And I’ve worried that I wasn’t getting enough of either.
That’s why I was glad to read Harvard Women’s Health Watch report titled,
A-3:
The answer, according to that report, is: Not as much as we may think and not as much as current U.S. guidelines call for. The minimum daily calcium requirement for women 50 and younger is 1,000 milligrams a day and for women over 50 it’s 1,200 milligrams.
For those of us in midlife, we’d need to drink four 8-ounce glasses of skim milk a day to get the recommended amount. If, like me, you’re not a milk drinker, it becomes really difficult to consume 1,200 milligrams a day, without also taking in a whole lot of calories and saturated fat in dairy products.
Some vegetables and fruits also contain calcium, but who really eats four helpings of collard greens a day? And that’s the vegetable with the MOST calcium. If you want to get all your calcium from oranges, you’ll need to eat 22 oranges a day and that’s just not happening. If you want to try the seafood route, you’ll be eating sardines or salmon for breakfast, lunch and dinner. Again, not happening.
Some foods are fortified with calcium, such as orange juice and cereal, but you still probably need to consume more than you want to get the recommended calcium.Of course, no one tries to get all the calcium we need from one food we get a little here and a little there. But, if you’re like me, you don’t get 1,200 milligrams most days.
Like many women, you may have memorized the minimum daily calcium requirement 1,000 milligrams (mg) a day for women ages 50 and younger and 1,200 mg for women over 50 and followed it faithfully in an effort to preserve your bones. You’ll probably be surprised to learn that many health authorities don’t agree with that recommendation. Dr. Walter Willett, chair of the Department of Nutrition at Harvard T.H. Chan School of Public Health, thinks you’re likely to do just as well on half as much calcium.
“Essentially, I think that adults do not need 1,200 mg of calcium a day. The World Health Organization’s recommendation of 500 mg is probably about right. The United Kingdom sets the goal at 700 mg, which is fine, too.
For more information visit us our website: https://www.healthinfi.com
0 200



No Comments