Polycystic Ovary Syndrome (PCOS)
Polycystic Ovary Syndrome (PCOS) is a condition that affects a woman’s hormone levels. Women with PCOS produce higher-than-normal amounts of male hormones. This hormone imbalance causes them to skip menstrual periods and makes it harder for them to get pregnant.
PCOS also causes hair growth on the face and body, and baldness. And it can contribute to long-term health problems like diabetes and heart disease. Birth control pills and diabetes drugs can help fix the hormone imbalance and improve symptoms.
What is PCOS?
PCOS is a problem with hormones that affects women during their childbearing years (ages 15 to 44). Between 2.2 and 26.7 percent of women in this age group have PCOS.
Many women have PCOS but don’t know it. In one study, up to 70 percent of women with PCOS hadn’t been diagnosed.
PCOS affects a woman’s ovaries, the reproductive organs that produce estrogen and progesterone hormones that regulate the menstrual cycle. The ovaries also produce a small amount of male hormones called androgens.
The ovaries release eggs to be fertilized by a man’s sperm. The release of an egg each month is called ovulation.
Follicle-stimulating hormone (FSH) and luteinizing hormone (LH) control ovulation. FSH stimulates the ovary to produce a follicle a sac that contains an egg and then LH triggers the ovary to release a mature egg.
PCOS is a “syndrome,” or group of symptoms that affects the ovaries and ovulation.
Its three main features are:
- cysts in the ovaries
- high levels of male hormones
- irregular or skipped periods
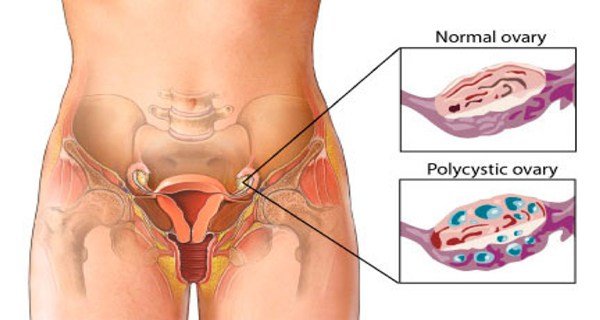
In PCOS, many small, fluid-filled sacs grow inside the ovaries. The word “polycystic” means “many cysts.”
These sacs are actually follicles, each one containing an immature egg. The eggs never mature enough to trigger ovulation.
The lack of ovulation alters levels of estrogen, progesterone, FSH, and LH. Estrogen and progesterone levels are lower than usual, while androgen levels are higher than usual.
Extra male hormones disrupt the menstrual cycle, so women with PCOS get fewer periods than usual.
PCOS isn’t a new condition. Italian physician Antonio Vallisneri first described its symptoms in 1721.
Common symptoms of PCOS
Some women start seeing symptoms around the time of their first period. Others only discover they have PCOS after they’ve gained a lot of weight or they’ve had trouble getting pregnant.
The most common PCOS symptoms are:
Irregular periods: A lack of ovulation prevents the uterine lining from shedding every month. Some women with PCOS get fewer than eight periods a year .
Heavy bleeding: The uterine lining builds up for a longer period of time, so the periods you do get can be heavier than normal.
Hair growth: More than 70 percent of women with this condition grow hair on their face and body including on their back, belly, and chest . Excess hair growth is called hirsutism.
Acne: Male hormones can make the skin oilier than usual and cause breakouts on areas like the face, chest, and upper back.
Weight gain: Up to 80 percent of women with PCOS are overweight or obese .
Male-pattern baldness: Hair on the scalp get thinner and fall out.
Darkening of the skin: Dark patches of skin can form in body creases like those on the neck, in the groin, and under the breasts.
Headaches: Hormone changes can trigger headaches in some women.
Signs and symptoms of PCOS vary.
A diagnosis of PCOS is made when you experience at least two of these signs:
Irregular periods. Infrequent, irregular or prolonged menstrual cycles are the most common sign of PCOS. For example, you might have fewer than nine periods a year, more than 35 days between periods and abnormally heavy periods.
Excess androgen. Elevated levels of male hormone may result in physical signs, such as excess facial and body hair (hirsutism), and occasionally severe acne and male-pattern baldness.
Polycystic ovaries. Your ovaries might be enlarged and contain follicles that surround the eggs. As a result, the ovaries might fail to function regularly.
Common signs and symptoms of PCOS include the following:
Menstrual disorders: PCOS mostly produces oligomenorrhea (fewer than nine menstrual periods in a year) or amenorrhea (no menstrual periods for three or more consecutive months), but other types of menstrual disorders may also occur.
Infertility:This generally results directly from chronic anovulation (lack of ovulation).
High levels of masculinizing hormones: Known as hyperandrogenism, the most common signs are acne and hirsutism (male pattern of hair growth, such as on the chin or chest), but it may produce hypermenorrhea (heavy and prolonged menstrual periods), androgenic alopecia (increased hair thinning or diffuse hair loss), or other symptoms. Approximately three-quarters of women with PCOS (by the diagnostic criteria of NIH/NICHD 1990) have evidence of hyperandrogenemia.
Metabolic syndrome: This appears as a tendency towards central obesity and other symptoms associated with insulin resistance. Serum insulin, insulin resistance, and homocysteine levels are higher in women with PCOS.
What are the symptoms and problems of polycystic ovary syndrome?
Symptoms that occur if you do not ovulate
Period problems occur in about 7 in 10 women with PCOS. You may have irregular or light periods, or no periods at all.
Fertility problems – you need to ovulate to become pregnant. You may not ovulate each month. Some women with PCOS do not ovulate at all. PCOS is one of the most common causes of not being able to get pregnant (infertility).
Symptoms that can occur if you make too much male hormone testosterone
Excess hair growth (hirsutism) occurs in more than half of women with PCOS. It is mainly on the face, lower tummy (abdomen) and chest. In other words, it tends to be male-pattern hair. This does not happen to all women with PCOS.
Acne may persist beyond the normal teenage years.
Thinning of scalp hair (similar to male pattern baldness) occurs in some cases.
Other symptoms
Weight gain – women with PCOS are more at risk of becoming overweight or obese.
Depression or poor self-esteem may develop as a result of the other symptoms.
Symptoms typically begin in the late teens or early 20s. Not all symptoms occur in all women with PCOS. For example, some women with PCOS have some excess hair growth but have normal periods and fertility.
Symptoms can vary from mild to severe. For example, mild unwanted hair is normal, and it can be difficult to say when it becomes abnormal in women with mild PCOS. At the other extreme, women with severe PCOS can have marked hair growth, infertility and obesity.
Symptoms may also change over the years. For example, acne may become less of a problem in middle age but hair growth may become more noticeable.
Cause
PCOS is a heterogeneous disorder of uncertain cause.There is some evidence that it is a genetic disease. Such evidence includes the familial clustering of cases, greater concordance in monozygotic compared with dizygotic twins and heritability of endocrine and metabolic features of PCOS.
There is some evidence that exposure to higher than typical levels of androgens in utero increases the risk of developing PCOS in later life.
The genetic component appears to be inherited in an autosomal dominant fashion with high genetic penetrance but variable expressivity in females; this means that each child has a 50% chance of inheriting the predisposing genetic variant(s) from a parent, and, if a daughter receives the variant(s), the daughter will have the disease to some extent.
The genetic variant(s) can be inherited from either the father or the mother, and can be passed along to both sons (who may be asymptomatic carriers or may have symptoms such as early baldness and/or excessive hair) and daughters, who will show signs of PCOS.
The phenotype appears to manifest itself at least partially via heightened androgen levels secreted by ovarian follicle theca cells from women with the allele.The exact gene affected has not yet been identified. In rare instances, single-gene mutations can give rise to the phenotype of the syndrome.Current understanding of the pathogenesis of the syndrome suggests, however, that it is a complex multigenic disorder.
The severity of PCOS symptoms appears to be largely determined by factors such as obesity.
PCOS has some aspects of a metabolic disorder, since its symptoms are partly reversible. Even though considered as a gynecological problem, PCOS consists of 28 clinical symptoms.
Risk factors
PCOS is thought to have a genetic component. People who have a mother or sister with PCOS are more likely to develop PCOS than someone whose relatives do not have the condition. This family link is the main risk factor.
Sugar is the body’s primary source of energy, and it is regulated in the body by insulin, which is secreted by the pancreas. A person with insulin resistance is unable to use insulin efficiently. This causes the pancreas to go into overdrive secreting additional insulin to meet the body’s glucose needs.
Excess insulin is thought to affect a woman’s ability to ovulate because of its effect on androgen production. Research has shown that women with PCOS have low-grade inflammation that stimulates polycystic ovaries to produce androgens.
Associated health risks
There are several health risks associated with PCOS.
These Include:
- type 2 diabetes
- infertility
- high cholesterol
- elevated lipids
- sleep apnea
- liver disease
- abnormal uterine bleeding
- high blood pressure
- obesity possibly leading to issues with low self-esteem and depression
- metabolic syndrome
- nonalcoholic fatty liver (steatohepatitis)
- depression and anxiety
Also, there is an increased risk of endometrial cancer, gestational diabetes, pregnancy-induced high blood pressure, heart attacks, and miscarriage.
Diagnosed
The first step in diagnosing PCOS is to have a complete history and physical examination performed by a trained health care provider.
A careful history and physical examination can detect whether androgen excess is causing male-pattern hair growth (hirsutism), acne or hair loss and whether ovulation is occurring normally.
Physical examination also can detect high blood pressure and increased abdominal obesity as risk factors for diabetes and cardiovascular disease in individuals who are overweight.
Blood tests then can be performed to determine whether the ovaries are functioning normally or producing excess amounts of androgen. An ovarian ultrasound also can be done to measure the size of the ovaries and determine whether they have a polycystic appearance.
At the same time, other conditions resembling PCOS, including pituitary, thyroid and adrenal abnormalities and other rare tumors, can be identified. Fasting blood levels of glucose, triglyceride and cholesterol also can be measured, along with another glucose determination obtained 2 hours after ingesting a glucose solution (2-hour oral glucose tolerance test), to predict the risk for developing diabetes and cardiovascular disease.
Treatment
There is no cure for PCOS, but treatment aims to manage the symptoms that affect an individual.
This will depend on whether the individual wants to become pregnant and aims to reduce the risk of secondary medical conditions, such as heart disease and diabetes.
There are several recommended treatment options, including:
Birth control pills: These can help regulate hormones and menstruation.
Diabetes medications: These help manage diabetes, if necessary.
Fertility medications: If pregnancy is desired, these include the use of clomiphene (Clomid), a combination of clomiphene and metformin, or injectable gonadotropins, such as follicle-stimulating hormone (FSH) and luteinizing hormone (LH) medications. In certain situations, letrozole (Femara) may be recommended.
Fertility treatments: These include in-vitro fertilization (IVF) or inseminations.
Excessive hair growth may be reduced with the drug spironolactone (Aldactone) or eflornithine (Vaniqa). Finasteride (Propecia) may also be recommended, but it should not be handled by women who may become pregnant.
Anyone using spironolactone should use birth control, due to the risk of birth defects if taken while pregnant. Breast-feeding on this medication is not recommended.
Other possible options to manage hair growth is laser hair removal, electrolysis, hormonal treatments, or vitamin and mineral use.
Diet
Where PCOS is associated with overweight or obesity, successful weight loss is the most effective method of restoring normal ovulation/menstruation, but many women find it very difficult to achieve and sustain significant weight loss.
A scientific review in 2013 found similar decreases in weight and body composition and improvements in pregnancy rate, menstrual regularity, ovulation, hyperandrogenism, insulin resistance, lipids, and quality of life to occur with weight loss independent of diet composition.
Still, a low GI diet, in which a significant part of total carbohydrates are obtained from fruit, vegetables, and whole-grain sources, has resulted in greater menstrual regularity than a macronutrient-matched healthy diet.
Vitamin D deficiency may play some role in the development of the metabolic syndrome, so treatment of any such deficiency is indicated. However, a systematic review of 2015 found no evidence that vitamin D supplementation reduced or mitigated metabolic and hormonal dysregulations in PCOS.
As of 2012, interventions using dietary supplements to correct metabolic deficiencies in people with PCOS had been tested in small, uncontrolled and nonrandomized clinical trials; the resulting data is insufficient to recommend their use.
Surgical options include:
Ovarian drilling: Tiny holes made in the ovaries can reduce the levels of androgens being produced.
Oophorectomy: Surgery removes one or both ovaries.
Hysterectomy: This involves removal of all or part of the uterus.
Cyst aspiration: Fluid is removed from the cyst.
Home remedies
There is no cure for PCOS, but some home and lifestyle interventions can make a difference and relieve some symptoms.
These include:
eating a healthy, well-balanced diet including plenty of fruits and vegetables
participating in regular physical activity
maintaining a healthy weight, to reduce androgen levels and reduce the risk of diseases such as diabetes and heart disease
not smoking, as this increases levels of androgens and the risk of heart disease.
0 200


No Comments