ACC (Aplasia Cutis Congenita)
Aplasia cutis congenita (ACC) is a heterogenous group of disorders characterized by the absence of a portion of skin in a localized or widespread area at birth. First reported by Cordon in 1767, aplasia cutis congenita manifests as a solitary defect on the scalp in 70% of cases, but it may sometimes occur as multiple lesions. Although most commonly seen on the scalp, aplasia cutis congenita can affect any part of the body, including the trunk and limbs.
Most lesions of aplasia cutis congenita occur on the scalp vertex just lateral to the midline, but defects may also occur on the face, trunk, or limbs, sometimes symmetrically. The defect may involve only the epidermis and upper dermis, resulting in minimal alopecic scarring, or it may extend into the deep dermis, subcutaneous tissue, or rarely periosteum, skull, and dura. Extension to deeper structures should be suspected in large, irregular lesions of aplasia cutis.
Aplasia cutis congenita is a rare malformation characterized by localized congenital absence of the skin. It rarely occurs on the trunk and limbs, and can occur in isolation or as part of a heterogeneous group of syndromes. We report a case of a 4-day-old boy with a 5.6-cm- diameter tumor, with a central crust, non-indurate and no inflammatory rim; localized on the scalp and a small, atrophic hairless scar appeared 6 months later (approximately 5cm in length) at the site of the previous tumor.
The exact etiology of ACC is still unclear but intrauterine infection by varicella or herpes virus, drugs such as methimazole, misoprostol, valproate, cocaine, marijuana etc., fetus papyraceus, feto-fetal transfusion, vascular coagulation defects, amniotic membrane adherence, abnormal elastic fiber biomechanical forces and trauma are implicated.[
Dermatological examination revealed a 5.6-cmdiameter tumor, with a central crust, non-indurate and no inflammatory rim; localized on the scalp, 1.5cm left of the midline. The newborn was otherwise healthy, with APGAR 10 at birth, young parents with no consanguinity or known medical problems. No visible or palpable scalp defect was found at the first examination. The parents did not agree to a skin biopsy or complete removal of the tumor despite the recommendation from pediatricians, while pediatricians from the Neonatology Department did not approve an MRI.
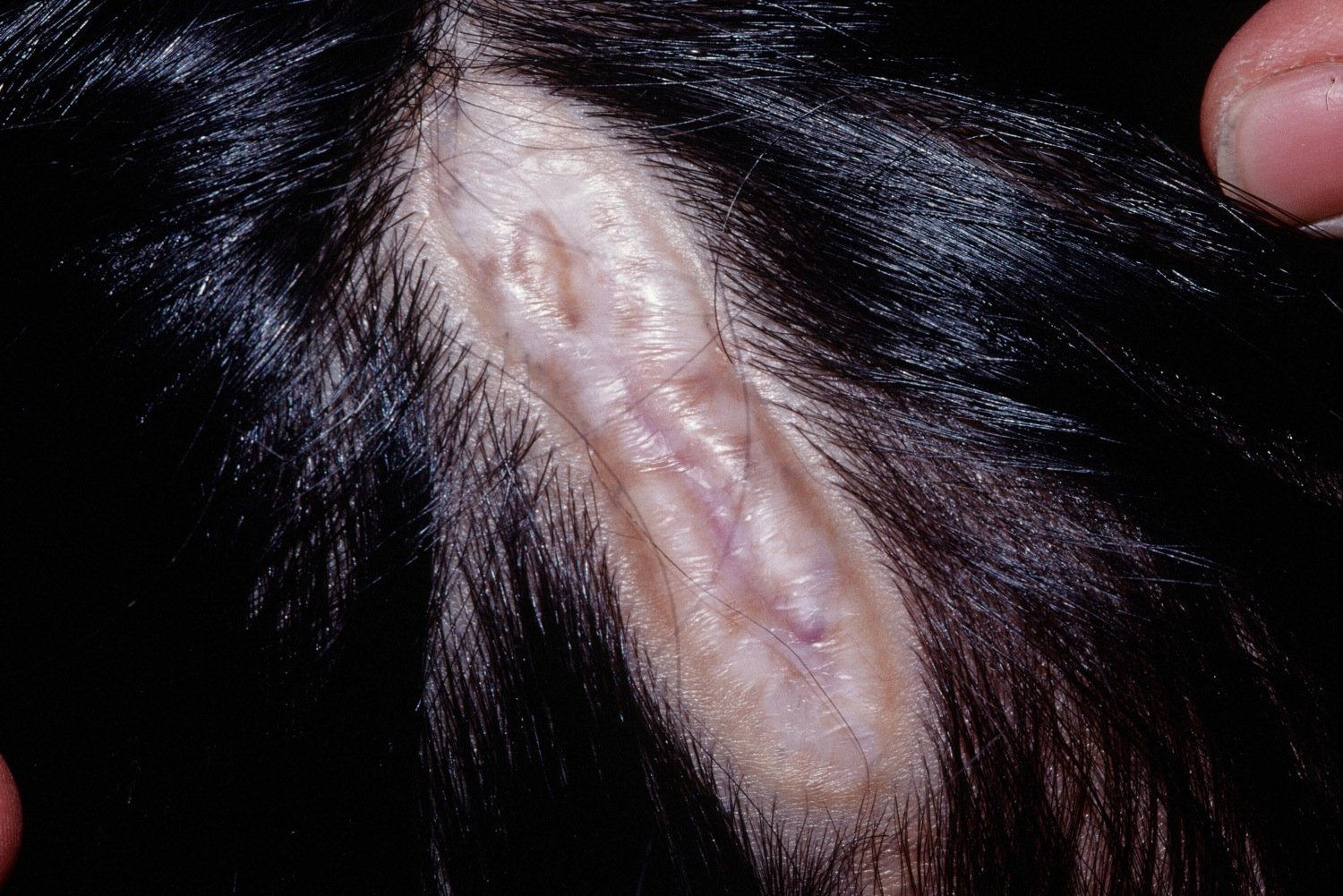
Aplasia Cutis Congenita
A reexamination was done 6 months later, revealing only a small, atrophic hairless scar of approximately 5cm in length, at the site of the previous tumor.
Local wound care was done with simple povidine iodine. The clinical diagnosis was aplasia cutis congenital and the main task (a difficult one) was to reassure the parents and medical staff from the Neonatology Department, instructing them simply to wait and observe the evolution of the skin lesion. There were no signs of infections and/or hemorrhages; no skull defects or other abnormalities.
In some cases, deeper defects can be observed: ulcerations that go through the dermis, subcutis, periosteum, even the skull and dura, with severe complications.
Pathogenesis
There exact pathogenesis of ACC is unknown. Various theories have been proposed, including the incomplete closure of the neural tube or embryonic fusion lines, intrauterine trauma, vascular compromise from placental insufficiency, ischemic or thrombotic event from fetus papyraceus (the demise of a twin fetus in the late first or early second trimester of pregnancy), amniotic membrane adhesions.
Synonyms of Aplasia Cutis Congenita
- ACC
- Congenital Defect of the Skull and Scalp
- Congenital ulcer of the newborn
- Scalp Defect Congenital
Signs & Symptoms
Most individuals with Aplasia Cutis Congenita exhibit no other abnormalities. However, in some rare cases, they may experience other physical characteristics including abnormalities of the ears, a form of paralysis (palsy) affecting one side of the face, an abnormally large head (macrocephaly), and/or congenital heart anomalies.
Aplasia Cutis Congenita may also occur as a physical condition characteristic of several other disorders, including Adams-Oliver Syndrome, Aplasia Cutis Congenita-Gastrointestinal, and Johanson-Blizzard Syndrome.
Individuals born with Aplasia Cutis Congenita lack skin (and therefore hair), in localized areas of the body, usually, but not always, on the scalp (70 percent of cases).
The vast majority of cases of ACC are small, isolated skin defects occurring on the scalp. It is reported that only 15 to 20% of cases of scalp ACC are associated with an underlying bony defect (2). ACC affecting large portions of the scalp (>3 × 5 cm) are very rare. In the cases of extensive scalp ACC it was reported that 75% had skull defects.
CNS malformations with ACC are rare. Non-scalp lesions may involve the trunk and/or extremities, and may be associated with epidermolysis bullosa or other congenital anomalies (3).
Complications of large scalp ACC with bony defect include sagittal sinus hemorrhage or thrombosis, site infection or meningitis. Mortality has been estimated to be as high as 25 to 55%, clinical manifestation of intractable seizures and developmental delay were reported (4). Our patient presented with an extensive area of scalp ACC (8*9cm), large underlying bone defect without CNS malformation. No family history of similar condition and no history of medications (lcohol or drugs) or disease during pregnancy could be elicited in our patient.
The patient’s skin and bone defects were treated with conservative dressing, with gradual epithelialization, no complications of infection or thrombosis were noted. By 1.5 year of age, the area of ACC was well-healed and the underlying parietal bone partially ossified.
Clinical examination at 18 months revealed normal growth and development, neurologically, the infant had no obvious deficit. Most lesions of ACC heal spontaneously with conservative dressing, small areas of ACC usually heal well with alopecic scars and with no residual problems, but large lesions may necessitate surgical interference with skin grafts or local skin flaps.
Full term male newborn, born by normal delivery after an uncomplicated pregnancy presented with extensive tissue defect of the scalp (measuring 8*9cm) and large underlying bony defect, the affected area consisted of a membranous and crusts cover over the entire posterior-parietal region (Figure 1). He showed no signs of acute distress or neurological impairment, MRI of brain revealed no abnormalities. There were no other organ abnormalities, routine laboratory data, infection, metabolic and hematological laboratory panels were normal. Karyotype was 46, XY.
Complete aplasia involving bone defects occurs in approximately 20% of cases. ACC can occur as an isolated defect or can be associated with a number of other congenital anomalies such as limb anomalies or embryologic malformations. In patients with large scalp and skull defects, there is increased risk of infection and bleeding along with increased mortality and therefore prompt and effective management is advised.
Case Description:
We describe two cases of ACC, involving a 4 × 3 cm defect managed conservatively and a larger 10 × 5 cm defect managed surgically with the use of a temporo-occipital scalp flap. Both cases had an excellent outcome.
Laboratory testing and brain MRI of the patient revealed no significant results. This case may present a new group of ACC classification, or a new neurocutaneous syndrome.
Thirteen patients were managed conservatively and 4 had primary surgical intervention. Of the cases that were managed with primary surgery, 2 had complications. None of the conservatively managed patients had complications in the acute setting. Conclusions: At the WCH, we advocate adopting a conservative approach to management of ACC of the scalp. Defects can be successfully managed with a combination of regular dressings and systemic antibiotics. Regular wound monitoring is essential to detect any complications early to instigate appropriate treatment and determine the need for emergency surgical management
Our case was a newborn infant with a large full thickness skin and skull defect on the scalp at birth. He also had hypoplasia on the fingers, omphalocele, ectopic anus, cleft lip and palate anomalies and multiple cardiac anomalies. We planned further evaluation but he died 23 hours after birth because of cardiac problems.
Ribosome biogenesis defects are known to often cause nucleolar stress and cell cycle arrest via p53-dependent or -independent means. Consistent with this, fibroblasts obtained from patients with mutations in BMS1 exhibited a p53-dependent, p21-upregulated slowing of the cell cycle at G1/S.
Collectively, the results imply that aplasia cutis congenita may be one among the ever growing list of human diseases classified as ribosomopathies (arising as a consequence of defects in ribosome biogenesis).
Highlights
- Laser therapy for fetal reduction could be associate with Aplasia Cutis Congenita.
- Despite of size of lesion conservative treatment could be an effective option.
- Extreme prematurity did not affected degree of spontaneous epithelization.
- Patient was followed up to 5 years and no complications were detected.
Background
Aplasia Cutis Congenita (ACC) is not a common condition. It occurs with an incidence rate of 1–3 cases per 10 000 live births, regardless of sex or race. Most of the lesions present on the scalp, and congenital skin aplasia on the lower limb is a rare finding. The cause of ACC lesions is heterogeneous. Cases of familial ACC have been described, as well as association with genetic disorders such as Adams-Oliver syndrome or Bart syndrome. The common mechanisms of ACC include vascular disruption, trauma, teratogens, or certain maternal medications during pregnancy (methimazole, azathioprine, valproic acid).
Monochorionic (MC) twin pregnancies are known to carry a high risk of twin-to-twin transfusion syndrome (TTTS) that could lead to miscarriage and perinatal death. Demise of one fetus is associated with co-fetal death in 12–25% of cases. Fetal reduction is the only procedure that could prevent these outcomes. Interstitial laser therapy is commonly used, and considered an effective and safe procedure but it still carries risks for both mother and fetus. O’Donoghue et al. reported that interstitial laser therapy may be associated with Aplasia Cutis Congenita (ACC) in up to 8% of fetuse.
For more information visit us our website: https://www.healthinfi.com
2 500
No Comments