What Is An Ileostomy?
An ileostomy is a stoma created from the small bowel, also called the ileum. The surgeon will bring the bowel through a small incision to the surface of the abdomen where it will be sutured to the skin. An ileostomy is usually situated on the right-hand side of the body and may be temporary or permanent.
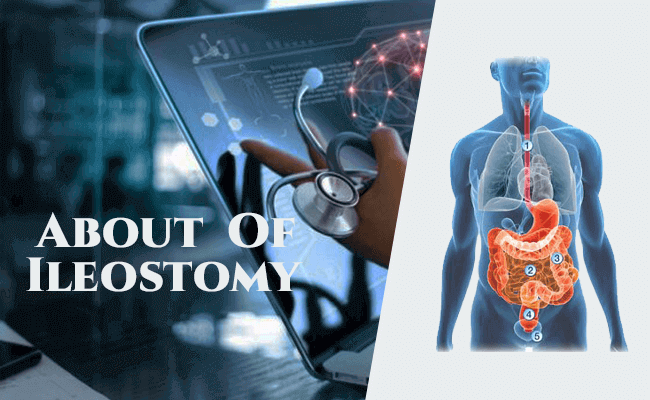
An ileostomy is a procedure used when there is a need to stop digestive waste from passing through the entirety of the colon or small intestine. Ileostomy surgery mainly concerns the colon and the rectum, which are the organs labeled as 3 and 4 on our post picture this diagram.
An ileostomy is used to move waste out of the body. This surgery is done when the colon or rectum is not working properly.
The word “ileostomy” comes from the words “ileum” and “stoma.” Your ileum is the lowest part of your small intestine. “Stoma” means “opening.” To make an ileostomy, the surgeon makes an opening in your belly wall and brings the end of the ileum through the opening. The ileum is then attached to the skin.
An ileostomy involves bypassing or removing the colon3 and sometimes the rectum4. Waste matter can no longer leave the body so it instead comes out of the stoma and collects in a stoma bag that is attached around it. This waste matter will be runny and will be passed quite frequently – this is because the waste material will not have passed through the colon, which is where most of the water in the waste is normally absorbed into the body.
Ileostomies are normally performed in very serious cases of inflammatory bowel disease (such as Ulcerative Colitis and Crohn’s disease). Temporary ileostomies can also be used to give the intestine a chance to rest and heal, or if you need to have a tumor removed.
There are two main types of ileostomy, dependent on the condition you are facing and the level of functionality or recovery period required by your digestive system. During a loop ileostomy procedure, a loop of the small intestine2 (also known as the ileum) is taken to the surface of the abdomen – the end of the ileum is the stoma.
This is usually a temporary procedure that can be reversed during a second operation. Alternatively, an end ileostomy may be used. This is where the end of the small intestine is separated from the large intestine and brought to the surface of your abdomen. These are more often seen as permanent procedures.
Ileostomy
An ileostomy is a surgery that makes a temporary or permanent opening called a stoma. A stoma is a pathway from the lowest part of the small intestine, called the ileum, to the outside of your abdomen. This helps solid waste and gas exit the body without passing through the colon or the rectum. The waste is collected in a pouch worn on the outside of your body.
An ileostomy is a stoma (surgical opening) constructed by bringing the end or loop of the small intestine (the ileum) out onto the surface of the skin or the surgical procedure which creates this opening. Intestinal waste passes out of the ileostomy and is collected in an external ostomy system which is placed next to the opening. Ileostomies are usually sited above the groin on the right-hand side of the abdomen.
An ileostomy is a surgically made opening that connects your ileum to your abdominal wall. The ileum is the lower end of your small intestine. Through the abdominal wall opening or stoma, the lower intestine is stitched into place. You may be given a pouch that you’ll wear externally. This pouch will collect all of your digested food.
The most common diseases resulting in an ileostomy are:
- Ulcerative colitis: – this causes inflammation and ulceration of the lining of the rectum and large bowel, which leads to symptoms including diarrhea with blood and mucus, cramping pain, fatigue, weight loss, and anemia
- Crohn’s disease: – this is an inflammatory bowel disease, which can affect any part of the gastrointestinal system and can cause symptoms including pain, diarrhea with blood and mucus, fatigue, mouth ulcers, weight loss, and anemia
- Cancerous growths affecting the colon
- Familial adenomatous polyposis (FAP): – this is an inherited condition, which affects the colon and rectum. People with FAP develop polyps (adenomas) inside the large bowel, which may become cancerous if left untreated
Waste from an ileostomy
The function of the colon is to absorb water and salt which results in well-formed feces. The waste from an ileostomy is quite loose because it is expelled before reaching the colon. Output may vary between a porridge and watery consistency which may also differ throughout the day, depending on how much fluid and food is consumed. The average output of an ileostomy is 500 -700 MLS per day therefore a drainable stoma bag will be worn which will need emptying several times per day. The bag will be changed every few days according to personal preference.
Procedure
If your ileostomy is temporary, your intestinal tract will be reattached inside your body once healing occurs.
Doctors will usually ask a person not to eat or drink for a period before surgery to ensure that the bowels are empty of stool.
Before the procedure begins, the surgeon and ostomy nurse will mark the location for the stoma.
The individual will receive general anesthesia and be unconscious throughout the procedure.
The surgeon will make an incision in the abdomen and identify the main areas of the bowel, including the colon, rectum, and ileum. They will then make an incision in the ileum and attach it to an opening in the abdominal wall.
The surgeon will sew around the ileum so that it stays attached to the opening.
Depending on the person’s condition, the surgeon may then remove the colon. Alternatively, they will sew the colon in such a way that it can rest and heal before then reattach it to the ileum in a later procedure.
For a permanent ileostomy, your surgeon removes or bypasses your rectum, colon, and anus. In this case, you’ll have a pouch that permanently collects your waste products. It may be internal or external.
Uses
Ileostomies are necessary where injury or a surgical response to the disease has meant the large intestine cannot safely process waste, typically because the colon and rectum have been partially or wholly removed.
Diseases of the large intestine which may require surgical removal include Crohn’s disease, ulcerative colitis, familial adenomatous polyposis, and total colonic Hirschsprung’s disease. An ileostomy may also be necessary in the treatment of colorectal cancer or ovarian cancer. One example is a situation where the cancer tumor is causing a blockage(obstruction).
In such a case the ileostomy may be temporary, as the common surgical procedure for colorectal cancer is to reconnect the remaining sections of the colon or rectum following removal of the tumor provided that enough of the rectum remains intact to preserve internal/external anal sphincter function.
In an end ileostomy, the end of the ileum is everted (turned inside out) to create a spout and the edges are sutured under the skin to anchor the ileum in place. Permanent ileostomies are usually done this way. An end ileostomy may be temporary, notably if some of the large intestines were removed and the bowel or overall health is not considered amenable to tolerating further surgery, such as an anastomosis to rejoin the small and large intestines.
How does an Ileostomy bag work?
An ileostomy bag collects waste material from your stoma, which generally has a fluid, porridge-like consistency. Most often, ileostomy bags are drainable so they can be emptied several times per day when they become full.
Ileostomy bags are fitted to a stoma in two parts, a flange that fits directly to the stoma and keeps the bag secure to avoid leakage, and the bag. The bag itself can either be permanently attached, in a complete, one-piece ileostomy bag system, or the flange and bag can be de-coupled so the ileostomy bag can be replaced more regularly than the flange – this is known as a two-piece system.
What is the small intestine?
The small intestine, or small bowel, runs between the stomach and the large intestine. The large intestine is made up of the colon and the rectum. The small intestine digests nutrients and absorbs them into blood vessels. Such nutrients include proteins, fats, and carbohydrates. Remaining food that cannot be digested moves from the small intestine to the colon. The colon absorbs water from the waste and stores the waste until the next bowel movement.
Ileostomy facts
Ileostomy: A surgically created opening in the abdomen in which a piece of the ileum (lowest part of the small intestine) is brought outside the abdominal wall to create a stoma through which digested food passes into an external pouching system.
Temporary ileostomy: May be required when a surgical site lower in the digestive tract needs time to heal. Examples include colorectal cancer surgeries, diverticulitis surgery, j-pouch surgery for ulcerative colitis or familial polyposis. A temporary ileostomy is usually constructed with a “loop” stoma.
Permanent ileostomy: May be required when the large intestine is removed and reconnection to the anus isn’t feasible. Possible causes include Crohn’s disease, some cancers, colonic dysmotility, some cases of ulcerative colitis or familial polyposis. A permanent ileostomy is usually constructed with an “end” stoma.
Care of ileostomy
A pouching system is worn. Pouches are odor-free and different manufacturers have disposable or reusable varieties to fit your lifestyle. Ostomy supplies are available at medical supply stores and through the mail and are covered by most health insurance plans.
Living with an ileostomy
Work
With the possible exception of jobs requiring very heavy lifting, an ileostomy should not interfere with work. People with ileostomies are successful business people, teachers, carpenters, welders, etc.
S**x and Social Life
Physically, the creation of an ileostomy usually does not affect sexual function. If there is a problem, it is almost always related to the removal of the rectum. The ileostomy itself should not interfere with normal sexual activity or pregnancy. It should not prevent one from dating and continuing relationships and friendships. UOAA Affiliated Support Groups are available for emotional support to couples.
Clothing: Depending on stoma location usually he is able to wear similar clothing as before surgery, including swimwear.
Sports and activities
With a securely attached pouch, one can swim and participate in practically all types of sports. Caution is advised in heavy body contact sports and a guard or belt can be worn for protection. Travel is not restricted in any way. Bathing and showering may be done with or without the pouch in place.
Diet
For guidance, follow your nurse or doctor’s orders at each stage of your post-op adjustment. Individual sensitivity to certain foods varies greatly. You must determine, by trial, what is best for you. See our guide for special considerations for those with an ileostomy including absorption and blockages. A good practice for all is to chew your food thoroughly and always hydrate properly.
Short bowel syndrome (sbs, short gut)
SBS is a rare but severe malabsorption issue. Short bowel syndrome generally occurs when a large portion of the small intestine has been removed by surgery or as a result of disease or injury. Know the symptoms and talk to a doctor to see if you are at risk.
Why do I need an ileostomy?
A doctor may perform an ileostomy to bypass or remove part of the intestine. This may be because:
- The large intestine is blocked or damaged
- A part of the large intestine is surgically removed
- A ruptured colon causes an abdominal infection
People with certain types of cancer, such as colorectal cancer, may need an ileostomy. Sometimes women being treated for ovarian cancer need an ileostomy. People with Crohn’s disease, ulcerative colitis, or familial adenomatous polyposis, which is a pre-cancerous condition, may also need an ileostomy.
How long will I need an ileostomy?
Most people who need a cancer-related ileostomy only need it for a few months while the colon or rectum heals. However, some people may need a permanent ileostomy.
Types of ileostomy (Ileostomy types)
There are 3 types of ileostomy:
- Standard ileostomy. This is also called a Brooke ileostomy. It is the most common type. The end of the small intestine is pulled through the right lower part of the abdomen and secured to the outside skin. You then wear a pouch at all times to collect stool that moves through the opening.
- Continent ileostomy. This ileostomy does not require you to wear a collection bag. The surgeon creates a pocket and valve in the end of the small intestine. You then insert a catheter several times a day into the pocket to drain the waste.
- Ileo-anal reservoir. This is also called a J-pouch or pelvic pouch. The surgeon creates a pouch from the small intestine and rectum. He or she connects the pouch to the anus to store waste. Stool can then be passed from the pouch through the anus.
What should I expect during surgery?
You will receive general anesthesia before the surgery. The procedure may be done with:
- A surgical incision, which is a large cut in the abdomen
- Laparoscopic surgery, which involves less invasive small incisions. This method reduces pain and recovery time.
Surgery may include the following risks:
- Bleeding inside the small intestine or from the stoma
- Damage to nearby organs
- Infection
- Not being able to absorb enough nutrients from food
- Intestinal blockage caused by scar tissue
How long will it take to recover from surgery?
Most patients stay in the hospital for up to 1 week after the procedure. Complete recovery from an ileostomy may take up to 2 months. During this time, you will have limits on what you can eat while the small intestine heals.
If the ileostomy is temporary, you may need a reversal, or closure, surgery after the small intestine has healed. This surgery usually takes place about 12 weeks later.
Ileostomy care
Emptying your ileostomy bag
Once you have recovered from surgery, you will need to empty the ileostomy bag several times per day. You will not be able to control when stool and gas move into the pouch. It is best to empty it when the bag is less than half full.
Ileostomy pouches come in many sizes and shapes, but there are 2 main types:
- One-piece pouches attach directly to the skin barrier.
- Two-piece pouches include a skin barrier and a pouch that can detach from the body.
Most pouches are drained through an opening in the bottom. Ask your health care team about which type of ileostomy pouch you will receive and instructions on how to empty it.
Draining waste with a catheter
If you have a continent ileostomy, the surgeon will leave a tube in the pouch so the waste can drain continuously, called an indwelling catheter. This will last for about 3 to 4 weeks. Once the indwelling catheter is removed, you will need to drain the pouch several times a day. This frequency will decrease over time.
Caring for your skin
The skin surrounding the stoma is called peristomal skin. It will always look red and may bleed occasionally, which is normal. However, bleeding should not continue for long.
It is important to make sure your pouch is correctly connected to your stoma. A pouch that fits poorly can irritate your skin. You should also keep this area clean and dry. If this skin appears wet, weepy, bumpy, itchy, or painful, it may be infected. Contact your healthcare team.
Ileostomy concerns
High stool output
During the first few days after surgery, you may have a larger than normal stool output. As your body gets used to the stoma and ileostomy, this amount will decrease. If it does not decrease after a few days, call your health care team. Passing large amounts of stool means you may be losing too many fluids. This could lead to an imbalance in your electrolyte levels. Electrolytes are minerals that help regulate the body.
Managing gas
Just like with stool, you will also need to release gas from your ileostomy pouch. The way you do this depends on the type of pouch. Some pouches have a filter that deodorizes and vents gas. This prevents the bag from becoming too stretched, coming off of the abdomen, or bursting.
Amounts of gas deposited into the pouch will vary based on the type of ileostomy and your diet. Foods and drinks such as beans, onions, milk, and alcohol can cause excess gas. Swallowing air can also increase the amount of gas in your small intestine. This happens when you chew gum or drink through a straw. You may have a lot of gas right after surgery. But this should decrease as your body heals. Your health care team can provide information on food and lifestyle choices to help reduce gas.
Whole pills or capsules in stool
Coated pills and extended-release capsules may come out intact in your pouch. This can mean that the medication was not fully absorbed in your body. Tell your health care team if this happens. They may be able to prescribe liquid or gel medications for you to take instead.
Stoma obstruction
Sometimes your stoma may become blocked by a piece of undigested food and scar tissue. This means that stool and gas cannot pass through into the pouch. An obstruction may cause abdominal pain or swelling or nausea or vomiting.
You may be able to remove the blockage at home. This can be done by avoiding solid foods and drinking more fluids, including warm drinks like tea. You can also try massaging your abdomen around the stoma or drawing your knees to your chest and rocking side to side. If these tips do not work, call your health care team right away.
How to prepare
Having an ileostomy will be a significant change in a person’s life. A person may experience fewer symptoms associated with bowel damage, but an ileostomy requires regular care.
It is essential to prepare for the changes to physical and mental health that can result from an ostomy. A doctor is likely to mention the following considerations among others:
- nutrition
- physical activity
- sexual health
- relationships
Before surgery, a person will usually meet with the surgeon and an ostomy nurse. The ostomy nurse, or enterostomal therapist, will present different pouch options and advise on preparing for life after surgery. They can also help a person order supplies.
If a surgeon needs to perform an ileostomy as part of an emergency procedure, the individual should receive education during recovery.
Recovery
Following surgery, the individual will typically stay in the hospital for several days. They will receive pain medication and instructions about diet and caring for the ileostomy.
Doctors and nurses also check patients carefully for postoperative complications, such as infection, bleeding, and intestinal blockage.
Even with lots of counseling before surgery, there are always challenges to navigate and questions to ask. There is no single best way to manage an ileostomy. Over time, a person has to learn what works best for them.
Immediately after surgery, the skin around the stoma may be itchy, red, or generally uncomfortable.
An infection, sometimes called pouchitis, can cause irritation and inflammation in the intestinal lining and require treatment with antibiotics.
In the first month or two following surgery, a person is likely to have strong gas.
People with an ileostomy should seek immediate medical attention if they notice sudden, significant changes in the stoma’s color or shape. For example, if the opening appears blue or dark, this can indicate that the skin is not getting enough oxygen.
A person should also seek urgent medical care if they experience one or more of the following signs and symptoms:
- excessive bleeding from the stoma
- nausea
- no output of stool for 4–6 hours
- severe diarrhea
- vomiting
These signs and symptoms indicate complications of the surgery, and a doctor will need to treat them immediately.
Lifestyle adjustments
Share on PinterestA person should drink plenty of water throughout the day to minimize diet-related ostomy complications.
Having an ileostomy can change many of a person’s habits, from their dietary choices to how they bathe. It is important to use doctors and ostomy nurses as a source of information.
Nutrition is an important consideration after surgery. Initially, a doctor usually recommends a low-fiber diet to give the bowel time to heal.
A person can usually minimize diet-related ostomy complications by:
- drinking plenty of water throughout the day
- limiting the consumption of potentially dehydrating beverages, such as those that contain alcohol or caffeine
- restricting foods that cause gas, such as cabbage and broccoli
- avoiding chewing gum, which can also cause gas
- chewing food thoroughly
- introducing new foods one at a time
- eating small meals at regular intervals
It is vital that people with an ileostomy discuss any diet-related challenges with a dietitian or doctor.
Adjusting to an ileostomy can be difficult, and support groups exist for people with ostomies. The United Ostomy Association of America, for example, has compiled a searchable database of online and in-person support groups.
Talking openly about fears, concerns, and challenges relating to an ileostomy can help a person manage and overcome them.
Outlook
An ileostomy can be life-saving. It is a surgical intervention that allows stool to exit the body without passing through damaged portions of the bowel.
Caring for an ileostomy can represent a significant lifestyle change. It can take weeks, months, or even longer for a person to adjust to their ostomy appliance.
Counseling before and after surgery can help. Doctors, ostomy nurses, and support groups can provide information and assistance.
Complications
These can be classified as immediate, early, or late or as procedure-specific and general complications. It is important to note that complications following the creation of an intestinal stoma are experienced by 20% of the patients. General complications vary depending on the type of operation being undertaken for an ileostomy to be necessary. Procedure-specific complications include the following:
- Stenosis
- Ischemia/Necrosis
- Hemorrhage
- Infection/Abscess
- A parastomal hernia
- Retraction/Prolapse
- Electrolyte imbalance due to the high output of the effluent from the ileostomy
- Dehydration
- Renal impairment
- Hematoma/Seroma
- Obstruction
- Fistula formation
- Skin irritation
When is an ileostomy needed?
Ileostomies are formed to either temporarily or permanently stop digestive waste passing through the full length of the small intestine or colon.
There are a number of reasons why this may be necessary, including:
- to allow the small intestine or colon to heal after it’s been operated on – for example, if a section of bowel has been removed to treat bowel cancer
- to relieve inflammation of the colon in people with Crohn’s disease or ulcerative colitis
- to allow for complex surgery to be carried out on the anus or rectum
The ileostomy procedure
Before an ileostomy is formed, you’ll normally see a specialist stoma nurse to discuss exactly where you’d like your stoma to be (usually somewhere on the right-hand side of the abdomen) and to talk about living with a stoma.
There are 2 main types of ileostomy:
- loop ileostomy – where a loop of small intestine is pulled out through a cut (incision) in your abdomen, before being opened up and stitched to the skin to form a stoma
- end ileostomy – where the ileum is separated from the colon and is brought out through the abdomen to form a stoma
Alternatively, it’s sometimes possible for an internal pouch to be created that’s connected to your anus (ileo-anal pouch).
This means there’s no stoma and stools are passed out of your back passage in a similar way to normal.
End ileostomies and ileo-anal pouches are usually permanent. Loop ileostomies are usually intended to be temporary and can be reversed during an operation at a later date.
Before Your Surgery
The information in this section will help you get ready for your surgery. Read through this section when your surgery is scheduled and refer to it as your surgery date gets closer. It has important information about what you need to do before your surgery.
Write down your questions and be sure to ask your healthcare provider.
Getting ready for your surgery
You and your healthcare team will work together to get ready for your surgery. Help us keep you safe during your surgery by telling us if any of the following statements apply to you, even if you aren’t sure.
- I take a blood thinner. Some examples are aspirin, heparin, warfarin (Jantoven, Coumadin), clopidogrel (Plavix), enoxaparin (Lovenox), dabigatran (Pradaxa), apixaban (Eliquis), and rivaroxaban (Xarelto). There are others, so be sure your healthcare provider knows all the medications you’re taking.
- I take prescription medications (medications prescribed by a healthcare provider), including patches and creams.
- I take over-the-counter medications (medications I buy without a prescription), including patches and creams.
- I take dietary supplements, such as herbs, vitamins, minerals, or natural or home remedies.
- I have a pacemaker, automatic implantable cardioverter-defibrillator (AICD), or other heart devices.
- I have sleep apnea.
- I have had a problem with anesthesia (medication to make you sleep during surgery) in the past.
- I’m allergic to certain medication(s) or materials, including latex.
- I’m not willing to receive a blood transfusion.
- I drink alcohol.
- I smoke.
- I use recreational drugs.
About drinking alcohol
The amount of alcohol you drink can affect you during and after your surgery. It’s important to talk with your healthcare providers about how much alcohol you drink. This will help us plan your care.
- If you stop drinking alcohol suddenly, it can cause seizures, delirium, and death. If we know you’re at risk for these complications, we can prescribe medications to help keep them from happening.
- If you drink alcohol regularly, you may be at risk for other complications during and after your surgery. These include bleeding, infections, heart problems, and a longer hospital stay.
Here are things you can do before your surgery to keep from having problems:
- Be honest with your healthcare providers about how much alcohol you drink.
- Try to stop drinking alcohol once your surgery is planned. If you develop a headache, nausea (feeling like you’re going to throw up), increased anxiety, or can’t sleep after you stop drinking, tell your healthcare provider right away. These are early signs of alcohol withdrawal and can be treated.
- Tell your healthcare provider if you can’t stop drinking.
- Ask your healthcare provider questions about drinking and surgery. As always, all of your medical information will be kept confidential.
About smoking
If you smoke, you can have breathing problems when you have surgery. Stopping even for a few days before surgery can help. If you smoke, your healthcare provider will refer you to our Tobacco Treatment Program.
About sleep apnea
Sleep apnea is a common breathing disorder that causes you to stop breathing for short periods of time while sleeping. The most common type is obstructive sleep apnea (OSA). With OSA, your airway becomes completely blocked during sleep. OSA can cause serious problems during and after surgery.
Please tell us if you have sleep apnea or if you think you might have it. If you use a breathing device (such as a CPAP device) for sleep apnea, bring it with you the day of your surgery.
7 days before your surgery
Follow your healthcare provider’s instructions for taking aspirin
If you take aspirin or medication that contains aspirin, you may need to change your dose or stop taking it 7 days before your surgery. Aspirin can cause bleeding.
Follow your healthcare provider’s instructions. Don’t stop taking the aspirin unless they tell you to. For more information, read the resource Common Medications Containing Aspirin, Other Nonsteroidal Anti-inflammatory Drugs (NSAIDs), or Vitamin E.
Stop taking vitamin E, multivitamins, herbal remedies, and other dietary supplements
Stop taking vitamin E, multivitamins, herbal remedies, and other dietary supplements 7 days before your surgery. These things can cause bleeding. For more information, read the resource Herbal Remedies and Cancer Treatment.
Buy clear liquids
You’ll need to follow a clear liquid diet before your surgery. It’s helpful to buy clear liquids ahead of time. For a list of clear liquids, you can drink, read the section “Follow a Clear Liquid Diet.”
2 days before your surgery
Stop taking no steroidal anti-inflammatory drugs (NSAIDs)
Stop taking NSAIDs, such as ibuprofen (Advil®, Motrin®) and naproxen (Aleve®), 2 days before your surgery. These medications can cause bleeding. For more information, read the resource Common Medications Containing Aspirin, Other Nonsteroidal Anti-inflammatory Drugs (NSAIDs), or Vitamin E.
1 day before your surgery
Follow a clear liquid diet
You’ll need to follow a clear liquid diet the day before your surgery. A clear liquid diet includes only liquids you can see through. Examples are listed in the “Clear Liquid Diet” table.
While you’re following this diet:
- Don’t eat any solid foods.
- Try to drink at least 1 (8-ounce) glass of clear liquid every hour while you’re awake.
- Drink different types of clear liquids. Don’t just drink water, coffee, and tea.
- Don’t drink sugar-free liquids unless you have diabetes and a member of your healthcare team tells you to.
For people with diabetes
If you have diabetes, ask the healthcare provider who manages your diabetes what you should do while you’re following a clear liquid diet.
- If you take insulin or another medication for diabetes, ask if you need to change the dose.
- Ask if you should drink sugar-free clear liquids.
While you’re following a clear liquid diet, make sure to check your blood sugar level often. If you have any questions, talk with your healthcare provider.
After surgery
You may need to stay in hospital for up to 2 weeks after an ileostomy operation.
During this time you’ll be taught how to look after your stoma by a specialist stoma nurse.
Recovering from the procedure can be challenging. Many people experience short-term physical and psychological problems, ranging from skin irritation around the stoma to feelings of anxiety and self-consciousness.
But with practice and support from a nurse with training in stoma care, many people adjust and often find their quality of life improves after surgery.
This is especially true if they have been living with a condition like Crohn’s disease for years.
Read more about recovering from an ileostomy procedure and living with an ileostomy.
Complications
As with any surgical procedure, having an ileostomy carries a risk of complications.
Some of the problems people with an ileostomy experience include:
- a bowel obstruction – where the output of digestive waste is blocked
- vitamin B12 deficiency – caused by the removal of part of the intestine that absorbs vitamin B12
- stoma problems – such as a change in the size of the stoma making it difficult to attach the external bag
Choosing a pouching system
Deciding what pouching system or appliance is best for you is a very personal matter. When you’re trying out your first pouching system, it’s best to talk with an ostomy nurse or someone who has experience in this area. There should be someone in the hospital who can get you started with equipment and instructions after surgery.
As you’re getting ready to leave the hospital, be sure you are referred to a Wound Ostomy Continence nurse (WOCN or WOC nurse, also called an ostomy nurse), a clinic, an ostomy manufacturer, or a chapter of the United Ostomy Associations of America. Even if you must go out of town to get such help, it’s worthwhile, as you want to get a good start and avoid mistakes. Even with help, you may have to try different types or brands of pouching systems to find the one that best suits you.
There are many things to think about when trying to find the pouching system that will work best for you. The length of the stoma, abdominal firmness and shape, the location of the stoma, scars and folds near the stoma, and your height and weight all must be considered. Special changes may have to be made for stomas near the hipbone, waistline, groin, or scars. Some companies have custom-made products to fit unusual situations.
A good pouching system should:
- Stay secure, with a good leak-proof seal that lasts for up to 3 days
- Be odor-resistant
- Protect the skin around the stoma
- Be nearly invisible under clothing
- Be easy to put on and take off
- Allow you to shower or bathe with the pouch on if you wish to do so
Reasons for having an ileostomy
If you have a large intestine problem that can’t be treated with medications, you might need an ileostomy. One of the most common reasons for an ileostomy is inflammatory bowel disease (IBD). The two types of inflammatory bowel disease are Crohn’s disease and ulcerative colitis.
Crohn’s disease can involve any part of the digestive tract, from the mouth to the anus, causing inflammation of the lining with sores and scarring.
Ulcerative colitis also has inflammation, sores, and scarring but involves the large intestine and rectum.
People with IBD will often find blood and mucus in their stool, and experience weight loss, poor nutrition, and abdominal pain.
Other problems that might require an ileostomy include:
- rectal or colon cancer
- an inherited condition called familial polyposis, in which polyps form in the colon that can lead to cancer
- intestinal birth defects
- injuries or accidents that involve the intestines
- Hirschsprung’s disease
Preparing for ileostomy
Getting an ileostomy will result in many changes to your life. However, you’ll be given training that will make this transition easier. You can talk with your doctor about how this procedure will affect your:
- sex life
- work
- physical activities
- future pregnancies
Make sure your doctor knows which supplements, medications, and herbs you’re taking. Many drugs affect the function of the intestine by slowing it down. This applies to over-the-counter as well as prescription medications. Your doctor may tell you to stop taking certain drugs two weeks before your surgery. Tell your doctor about conditions that you have, such as:
- the flu
- a cold
- a herpes breakout
- a fever
Smoking cigarettes makes it harder for your body to heal after surgery. If you’re a smoker, try to quit.
Drink lots of water and maintain a healthy diet in the weeks leading up to your surgery.
Follow your surgeon’s instructions regarding diet in the days prior to surgery. At some designated time, they may advise you to switch to clear liquids only. You’ll be advised not to consume anything, including water, for about 12 hours before surgery.
Your surgeon may also prescribe laxatives or enemas to empty your intestines.
Procedure
An ileostomy is done in a hospital under general anesthesia.
After you’re unconscious, your surgeon will either make a cut down your midline or perform a laparoscopic procedure using smaller cuts and lighted instruments. You will know prior to the surgery which method is recommended for your condition. Depending on your condition, your surgeon may need to remove your rectum and colon.
There are several different types of permanent ileostomies.
For a standard ileostomy, the surgeon makes a small incision that will be the site of your ileostomy. They’ll pull a loop of your ileum through the incision. This part of your intestine is turned inside out, exposing the inner surface. It’s soft and pink, like the inside of a cheek. The part that sticks out is called a stoma. It may protrude up to 2 inches.
People with this type of ileostomy also called a Brooke ileostomy, won’t have control of when their fecal waste flows into the external plastic pouch.
Another type of ileostomy is the continent, or Kock, ileostomy. Your surgeon uses part of your small intestine to form an internal pouch with an external stoma that serves as a valve. These are stitched to your abdominal wall. A few times per day you insert a flexible tube through the stoma and into the pouch. You expel your waste through this tube.
The advantages of the Kock ileostomy are that there’s no external pouch and you can control when you empty your waste. This procedure is known as a K-pouch procedure. It’s often the preferred method of ileostomy because it eliminates the need for an external pouch.
A different procedure, known as the J-pouch procedure, may be performed if you’ve had your entire colon and rectum removed. In this procedure, the doctor creates an internal pouch from the ileum that is then connected to the anal canal, allowing you to expel your waste through the usual route with no need for a stoma.
Recovery from ileostomy
You’ll typically need to stay in the hospital for at least three days. It’s not uncommon to remain hospitalized for a week or even longer, especially if your ileostomy was done under emergency circumstances.
Your food and water intake will be limited for a while. On the day of your surgery, you may only get ice chips. Clear liquids will probably be allowed on the second day. Slowly, you’ll be able to eat more solid foods as your bowels adjust to the changes.
In the early days after surgery, you may have excessive intestinal gas. This will decrease as your intestines heal. Some people have found that digesting four to five small meals per day is better than three larger meals. Your doctor may suggest that you avoid certain foods for a while.
During your recovery, whether you have an internal or external pouch, you’ll start to learn how to manage the pouch that will collect your waste. You’ll also learn to care for your stoma and the skin around it. Enzymes in the discharge from your ileostomy can irritate your skin. You’ll need to keep the stoma area clean and dry.
If you have an ileostomy, you may find that you need to make big adjustments to your lifestyle. Some people seek help from an ostomy support group. Meeting other people who’ve adjusted their lifestyles after this surgery and have managed to return to their regular activities can ease any anxieties you have.
You can also find nurses who are specially trained in ileostomy management. They’ll ensure that you have a manageable lifestyle with your ileostomy.
Long-term outlook
Once you learn to take care of your new elimination system, you’ll be able to participate in most of your regular activities. People with ileostomies:
- swim
- hike
- play sports
- eat in restaurants
- camp
- travel
- work in most occupations
Heavy lifting can be a problem because it can aggravate your ileostomy. Talk to your doctor if your job requires heavy lifting.
Having an ileostomy doesn’t usually interfere with sexual function or the ability to have children. It might require you to educate your sexual partners, who might be unfamiliar with ileostomies. You should discuss your ostomy with your partner before progressing to intimacy.
What are the risks of having an ileostomy?
You may have trouble with your stoma. If the skin around it is irritated or moist, you’ll have a hard time getting a seal with your ostomy pouch. This can result in a leakage. Your doctor can prescribe a medicated topical spray or powder to heal this irritating skin.
Some people hold their external pouch in place with a belt. If you wear the belt too tightly, it can lead to pressure ulcers.
You’ll have times in which no discharge comes through your stoma. However, if this continues for more than four to six hours and you feel nauseous or have cramps, call your doctor. You might have an intestinal blockage.
People who’ve had ileostomies may also get electrolyte imbalances. This happens when you lack the correct amount of important substances in your blood, especially sodium and potassium. This risk increases if you lose a lot of fluids through vomiting, perspiration, or diarrhea. Be sure to replenish lost water, potassium, and sodium.
There are risks and side effects related to having an ileostomy. Risks and side effects may be:
- Infection.
- Bleeding.
- Blood clots.
- heart attack
- stroke
- difficulty breathing
- Damage or injury to nearby organs.
- Adhesion/scar tissue formation (An adhesion is scar tissue that joins 2 pieces of tissue that should not be joined. They are often painless and do not need treatment. Serious cases can cause a blockage in the bowel or limit blood flow).
- Bowel obstruction (This is a blockage in the bowel that can limit digestion or the removal of stool).
- Wound separation or issues with healing.
- Electrolyte changes in the body, most commonly with sodium and potassium.
- Diarrhea.
- Issues with the stoma, such as skin irritation, infection and leaking.
- The feeling of the need to have a bowel movement called “phantom rectum.”
- Short bowel syndrome, which may lead to vitamin and nutrient absorption problems.
Risks that are specific to ileostomies include:
- damage to the surrounding organs
- internal bleeding
- an inability to absorb enough nutrients from food
- urinary tract, abdominal, or lung infections
- an intestinal blockage due to scar tissue
- wounds that break open or take a long time to heal
What is recovery like?
Recovery from an ileostomy will depend on the extent of the procedure you have had. How long you stay in the hospital will depend on the procedure you had and how well you are recovering.
You will be told how to care for your surgical incisions/stoma and will be given any other instructions before leaving the hospital. Full instructions on caring for your stoma will be given to you by a specially trained stoma nurse/therapist.
Your care team will discuss with you the medications you will be taking, such as those for pain, blood clots, infection, and constipation prevention, management of diarrhea, and/or other conditions. They will also discuss with you the need and type of follow-up care you will need, such as checking your blood electrolyte levels.
Your provider will tell you what you should and should not do when you go home. This will often include:
- Changes in activity level such as bending, lifting, and exercising.
- Not driving while taking pain medication.
- Returning to work in 2-4 weeks, depending on your job and work duties.
- Details about showering, submerging your surgical incisions in water, diet recommendations, sexual activity, and stoma care.
What will I need at home?
- Thermometer to check for fever (101°F, 38.3°C), which can be a sign of infection.
- Incision and stoma care supplies, often supplied by the hospital, your healthcare team or the stoma nurse/therapist.
When should I call my provider?
- Signs of infection, including fever and redness, odor or drainage at the incision.
- Nausea, vomiting, bloating, or cramps lasting more than 2 hours.
- No ileostomy output for 4-6 hours with cramping and nausea.
- Leg swelling and/or sudden shortness of breath.
- No new or worsening pain.
- A decrease in peeing.
- Blood in the ostomy pouch.
- Changes to the stoma, including retraction (pulling inward), changes in size or color, stoma blockage or bulging, bleeding, wounds, injury to the stoma, skin irritation/sores, and/or watery stool for 5 or more hours.
How can I care for myself?
You may need a family member or friend to help you with your daily tasks until you are feeling better. It may take some time before your team tells you that it is ok to go back to your normal activity.
Be sure to take your prescribed medications as directed to prevent pain, infection, and/or constipation. Call your team with any new or worsening symptoms.
There are ways to manage constipation after your surgery. You can change your diet, drink more fluids, and take over-the-counter medications. Talk with your care team before taking any medications for constipation.
Taking deep breaths and resting can help manage pain, keep your lungs healthy after anesthesia, and promote good drainage of lymphatic fluid. Try to do deep breathing and relaxation exercises a few times a day in the first week, or when you notice you are extra tense.
- Example of a relaxation exercise: While sitting, close your eyes and take 5-10 slow deep breaths. Relax your muscles. Slowly roll your head and shoulders.
“This article contains general information. Please be sure to talk to your care team about your specific plan and recovery”
Types of pouching systems
Pouches come in many styles and sizes, and an ostomy nurse can help you choose the best one for your situation and lifestyle. They all have a collection pouch to collect stool drainage that comes out of the stoma and an adhesive barrier (called a flange, skin barrier, or wafer) that protects the surrounding skin. There are 2 main types of systems available:
- One-piece pouches have both a pouch and skin barrier attached together in the same unit. When the pouch is removed, the barrier also comes off.
- Two-piece systems have a pouch and a separate skin barrier. When the pouch is taken off, the barrier stays in place.
Depending on the design of your pouch’s skin barrier, you may need to cut a hole out for your stoma, or it may be sized and pre-cut. It’s designed to protect the skin from the stoma output and be as gentle to the skin as possible.
Some pouching systems can be opened at the bottom for easy emptying. Others are closed and are taken off when they are full. Still, others allow the adhesive skin barrier to staying on the body while the pouch may be taken off, washed out, and reused. Pouches are made from odor-resistant materials and vary in cost. They can be either clear or opaque and come in different lengths.
After surgery, the stoma may be swollen for about 6 to 8 weeks. During this time the stoma should be measured about once a week. A measuring card may be included in boxes of pouches, or you can make your own template to match your stoma shape. The opening on the skin barrier should be no more than 1/8 inch larger than the stoma.
Belts and tape
Wearing a belt to help hold the pouch in place is a personal choice. Some people with ileostomies wear a belt because it makes them feel more secure and it supports the pouching system. Others find a belt awkward and use tape instead. Tape can be put around the outside edge of the skin barrier like a frame.
If you choose to wear a belt, adjust it so that you can get 2 fingers between the belt and your waist. This helps to keep you from getting a deep groove or cut in the skin around the stoma which can cause serious damage to the stoma and sores (pressure ulcers) on the nearby skin. If a belt is used, it shouldn’t ride above or below the level of the belt tabs on the pouching system. People in wheelchairs may need special belts. Supply companies often carry these special belts or an ostomy nurse can talk to you about making one yourself.
0 200



No Comments