The change of life. The end of fertility. The beginning of freedom. Whatever people call it, menopause is a unique and personal experience for every woman. It’s a natural event that marks the end of fertility and childbearing years. Technically, menopause results when the ovaries no longer release eggs and decrease production of the sex hormones estrogen, progesterone and, to a lesser extent,androgen. Menopause is said to have occurred when a woman has not had a period for 12 months.
Menopause & the Reproductive Cycle
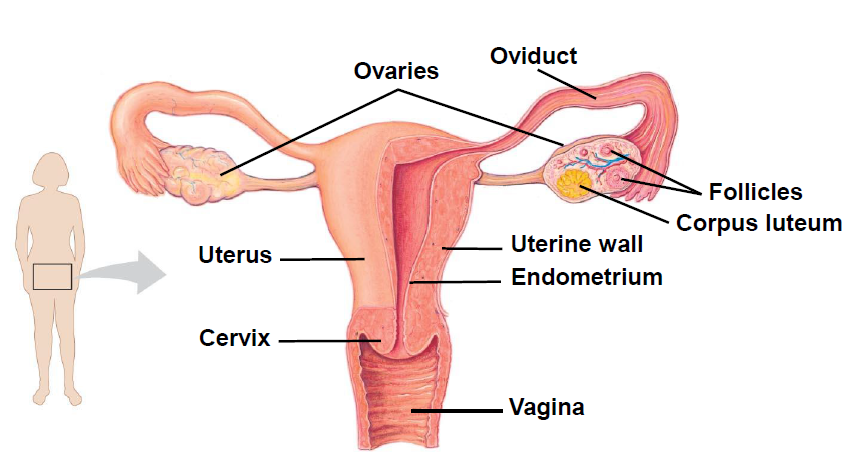
Reproduction
During the reproductive years, a gland in the brain generates hormones that cause an egg from the ovaries to be released from its follicle each month. As the follicle develops, it produces the sex hormones estrogen and, after ovulation, progesterone, which results in a thickened uterine lining. This enriched lining is prepared to receive and nourish a fertilized egg, which could develop into a fetus. If fertilization does not occur, estrogen and progesterone levels drop, the lining of the uterus breaks down and menstruation occurs.
Perimenopause
For reasons unknown, your ovaries gradually begin to function less efficiently during your mid-to-late 30s. In your late 40s, the process accelerates along with greater hormone fluctuations. This affects ovulation and levels of the hormones estrogen and progesterone. During this transition period, called perimenopause, you may experience irregular menstrual cycles and unpredictable episodes of menstrual bleeding. By your early to mid-50s, your periods will likely end.
Most women can tell if they are approaching menopause because their menstrual periods start changing. The “menopause transition” is a term used to describe this time, as is perimenopause.
Menopause
But menopause itself—as defined by health care professionals—is a woman’s final menstrual period, which can be confirmed after she goes 12 consecutive months with no period, and no other biological or physiological cause can be identified; it also may occur when both ovaries are surgically removed or damaged. Until that time, a woman in her late 40s or 50s may still be able to get pregnant, despite irregular periods.
Medical Intervention
Although the majority of women experience “natural” or spontaneous menopause, some women may experience menopause due to a medical intervention. Surgically removing both ovaries, a procedure known as bilateral oophorectomy, triggers menopause at any age. Induced menopause can also occur if the ovaries are damaged by radiation, chemotherapy or certain drugs. Some medical conditions also may cause menopause to occur earlier.
Naturally Occurring
Just as every woman’s body is unique, each woman’s menopause experience will be highly personal. In fact, some women experience no physical symptoms at all, except the end of their menstrual periods.
Menopause can occur as early as your 30s and, rarely, as late as your 60s. However, there is no correlation between the time of a woman’s first period and her age at menopause. In addition, age at menopause is not influenced by race, height, the number of children a woman has had or whether she took oral contraceptives for birth control.
Early Menopause
Although the average age for menopause in the United States is 51, some women experience it later or earlier. Early menopause is defined as occurring at any age younger than age 45. Menopause that occurs in women younger than 40 is called premature menopause or premature ovarian failure. and can occur naturally.; But symptoms of premature menopause, such as irregular periods, may signal an underlying condition, so it is important to discuss any symptoms with your health care professional.
What influences the time of menopause? Genetics are a key factor. The age at which your mother stopped her periods may be similar to when you stop your menstrual periods. And women who smoke cigarettes experience menopause two years earlier, on average, than nonsmoking women.
Symptoms of Menopause
- Irregular Periods: About four to eight years prior to natural menopause, typically in a woman’s late 40s, menopause-related changes may begin. One of the most common and annoying symptoms you may notice during your 40s is that your periods become irregular. They may be heavy one month and very light the next. They may get shorter or last longer. You may even begin to skip your period every few months or lose track of when your periods should start and end. These symptoms are caused by irregular estrogen and progesterone levels.
- Changes in Hormone Levels: Levels of hormones vary erratically and may be higher or lower than normal during any cycle. For example, if you don’t ovulate one month—which is common for women in their late 40s—progesterone isn’t produced to stimulate menstruation, and estrogen levels continue to rise. This can cause spotting throughout your cycle or heavy bleeding when menstruation does start.One note of caution: although irregular menstrual periods are common as you get closer to menopause, they can also be a symptom of uterine abnormalities or uterine cancer.
- See your health care professional as soon as possible if your periods stop for several months and then start again with spotting or heavy bleeding; if you have irregular spotting; if you have bleeding after intercourse; or if you start bleeding after menopause. Be sure to mention any menstrual irregularities during regular checkups. Uterine biopsy and vaginal ultrasound are the only ways to evaluate these symptoms and determine whether they are caused by abnormalities in the uterus. Irregular spotting can also be a symptom of cervical cancer, which may be picked up by a Pap test (see screening in Treatment section).
Other changes and signs of menopause include:
- Hot flashes (sudden warm feeling, sometimes with blushing)
- Night sweats (hot flashes that occur at night, often disrupting sleep)
- Fatigue (probably from disrupted sleep patterns)
- Mood swings
- Vaginal dryness
- Fluctuations in sexual desire or response
- Difficulty sleeping
Menopause-Related Health Conditions
Although there is a wide range of possible menopause-related conditions, most women experiencing natural menopause only have mild disturbances during the perimenopausal years. However, you should be aware that there are at least two major health conditions that can develop in the post-menopausal years: coronary artery disease and osteoporosis.
- Coronary Artery Disease: Your body’s estrogen helps protect against plaque buildup in your arteries. It does this by helping to raise HDL cholesterol (good cholesterol), which helps remove LDL cholesterol (the type that contributes to the accumulation of fat deposits called plaque along artery walls). As you age, your risk for developing coronary artery disease (CAD)—a condition in which the veins and arteries that take blood to the heart become narrowed or blocked by plaque—increases steadily. Heart attack and stroke are caused by atherosclerotic disease, in most cases.
- Osteoporosis: Your body’s own estrogen helps prevent bone loss and works together with calcium and other hormones and minerals to build bones. Your body constantly builds and remodels bone through a process called resorption and deposition. Up until around age 30, the body makes more new bone than it breaks down. But once estrogen levels start to decline, this process slows down.
By menopause, your body breaks down more bone than it rebuilds. In the years immediately after menopause, some women may lose as much as 20 percent of their bone mass in the first five to seven years following menopause. Although loss of bone density eventually levels out, in the years ahead, keeping bone structures strong and healthy to prevent osteoporosis becomes more of a challenge. Osteoporosis occurs when bones become too weak and brittle to support normal activities.
Preventing Menopause-Related Health Condition with Exercise
Not all women develop heart disease or osteoporosis. Many more things affect your heart and your bones than estrogen alone. For example, exercise improves your cardiovascular system—your heart, lungs and blood vessels—at any age. It can help decrease high blood pressure, a concern for half of women over age 60, and can help maintain bone mass. It can also help reduce weight gain, a major risk factor for heart disease, diabetes and many other health conditions common to older women.
You are never too old to begin or continue exercising. A simple walking routine for 30 minutes four to five days a week can provide health benefits. There are other exercise options. Talk to your health care professional about which ones fit your lifestyle and medical needs.
If your bones are strong and healthy as you enter menopause, you’ll have better bone structure to sustain you as you age. Bone loss varies from woman to woman. You can improve bone strength as you age by exercising regularly and making sure you get enough calcium in your diet or from supplements. Exercise also helps improve balance, muscle tone and flexibility, which can diminish with aging. Weakness in these areas can lead to more frequent falls, broken bones and longer healing periods.
Women today can expect to live as much as one-third of their lives beyond menopause. The years following menopause can be healthy years, depending on how you take care of yourself.
Diagnosis
Menopause is diagnosed when a woman who has a uterus has not had a menstrual period for one year.
Some of the more common signs of the menopause transition (a term that refers to the five or more years around the time of menopause) that may prompt a woman to seek consultation with a qualified health care professional include:
- Hot flashes
- Vaginal dryness
- Urinary tract infections or painful urination
- Stress incontinence (leaking of urine)
- Night sweats
- Insomnia
- Headaches
- Heart palpitations
- Forgetfulness
- Mood changes
- Anxiety and irritability
- Diminished concentration
- Decreased sexual desire
Ask your health care professional about any changes you notice. And remember, menopause is not a disease; it is another life stage. (The changes listed above have not all been scientifically proven to be related to menopause.)
As part of the evaluation of symptoms that may be caused by menopause, your health care professional will carefully assess your symptoms and administer a thorough physical examination. You will also be asked to provide a complete medical history; be sure to include information about your family medical history, as well.
Laboratory tests may include baseline serum chemistry studies, lipid evaluation and hormonal evaluation.
Other tests may include:
- Pap test
- Mammography
- Bone density screening
- Assessment of the uterine lining, when indicated
- Pelvic ultrasound screening, when indicated
Menopause is associated with consistently increased follicle stimulating hormone (FSH) levels. In perimenopausal women, elevated FSH levels are sometimes detected; however, this FSH elevation is often intermittent (and therefore unreliable), so the ultimate determining factor in knowing whether you have experienced menopause is if you have not had a period for 12 consecutive months.
Treatment
Menopause Management
Many women pay close attention to their gynecological health during their younger years and start to ignore it after menopause. Your wellness plan after menopause should include, at minimum, annual visits to a health care professional.
These visits should include:
- An annual breast examination by a health care professional
- A mammogram every one to two years
- An annual gynecologic exam
- A Pap test every three years or a Pap test combined with an HPV (human papillomavirus) test every five years.The American Congress of Obstetricians and Gynecologists (ACOG) recommends that beginning at age 30, women who have had three normal test results in a row get screened every three years with either the standard Pap test or liquid-based test.Women who have certain risk factors such as diethylstilbestrol (DES) exposure before birth, HIV infection, a history of cervical cancer or moderate to severe cervical dysplasia or a weakened immune system due to organ transplant, chemotherapy or chronic steroid use may need more frequent Pap tests.Women who are age 65 or older and who have had adequate prior screening with normal results and who are not at high risk for cervical cancer may stop getting Pap tests.
- One of the following tests—fecal occult blood test (FOTB), fecal immunochemical test (FIT) or stool DNA test (sDNA), all of which check for colon cancer—is recommended annually beginning at age 50. Talk to your doctor about which of the three tests is best for you.
- Colon cancer screening with colonoscopy every 10 years beginning at age 50 unless you or someone in your family has had benign colon polyps or colorectal cancer or an inflammatory bowel disease, such as ulcerative colitis, irritable bowel syndrome or Crohn’s disease, in which case you should start screening earlier. African Americans are at higher risk than other groups for getting colon cancer and dying from the disease. The American College of Gastroenterology recommends that African Americans begin screening for colon cancer at age 45.
- Blood pressure check at least every two years (more often if it’s chronically high), and blood cholesterol screening every five years (more often if it’s chronically high or you have other risk factors for heart disease or stroke); ask your health care professional for guidance.
- Bone density screenings, such as a dual-energy X-ray absorptiometry (DEXA or DXA) if you are over age 65, or at a younger age if you are at risk for developing osteoporosis; ask your health care professional about how often you should have this test; in some parts of the country, peripheral screening for bone density is available using peripheral dual-energy X-ray absorptiometry (pDXA) or ultrasound of the calcaneus (heel bone), however the results of these tests are not equivalent to the results of a DXA scan and should not be used to diagnose or manage osteoporosis.
- Annual screenings for diabetes (again, your health care professional may tell you this test is needed less frequently, depending on your risk factors).
- Thyroid function testing every five years, if recommended by your health care professional.
- Age-appropriate flu shots and other immunizations.
Discuss any unusual or uncomfortable symptoms with your health care professional. Keep track of medications that you take and ask your health care professional or pharmacist about potential drug interactions, if you are told to take a new medication. Be sure to discuss with your health care professional any alternative medical treatments or herbal products you use or may wish to use.
The Menopause Transition
As your body transitions into menopause (a process that typically lasts about four to eight years) you may notice some physical and emotional changes.
The most common include:
- Irregular menstrual periods
- Hot flashes
- Vaginal dryness
- Urinary tract infections
- Stress incontinence
- Night sweats
- Insomnia
- Headaches
- Heart palpitations
- Forgetfulness
- Mood changes
- Anxiety and irritability
- Diminished concentration
There are a variety of options available to relieve these symptoms, if you find they interfere with your lifestyle. Discuss your symptoms and your concerns with your health care professional to determine which options make the most sense for you.
The following tips may be recommended to relieve the most common menopausal symptoms:
Hot flashes
Although no one knows for sure what causes hot flashes, they’re believed to be the result of a narrowing of the temperature range that normally tells the brain to adjust your internal temperature. The pituitary gland in your brain increases the amount of follicle stimulating hormone (FSH) and luteinizing hormone (LH) aimed at the ovaries. Falling estrogen levels and the increase in FSH and LH levels disturb your body’s internal temperature. This creates instability in your vasomotor balance and results in a hot flash.
About 75 of every 100 women approaching or going through menopause have hot flashes, which usually last for about three to five years. Hot flashes may get more intense and more frequent around your last menstrual period and then taper off, usually stopping altogether after one to five years. Some women continue to have hot flashes past age 70, however.
During a hot flash, you may experience a sudden sensation of heat in your face, neck and chest. You may sweat profusely and your pulse may become more rapid. Some women get dizzy or nauseous. A hot flash typically lasts about two to four minutes—which can seem like an eternity. For some women hot flashes are intolerable, occurring at inconvenient moments or at night, disrupting sleep.
There are a variety of strategies for coping with hot flashes, ranging from short-term hormone therapy (estrogen alone or estrogen plus progesterone for approximately two to three years and no more than five years) and other medical options to herbal remedies, but lifestyle strategies may be the easiest and quickest changes to try first:
- Dress in layers that may be removed if you find you’re getting too warm.
- Sleep in a cool room.
- Drink plenty of water.
- Avoid hot foods such as soups, spicy foods, caffeinated foods and beverages and alcohol, which can trigger hot flashes.
- Try to decrease stress.
- Exercise regularly.
- Breathe deeply and slowly, if you feel a hot flash starting; rhythmic breathing may help to “turn down” the heat of a hot flash or prevent it from starting altogether.
- Use a hand-held fan.
Insomnia.
Sleep is often a casualty of menopause, whether it is interrupted by hot flashes (called night sweats when they occur at night) or difficulty falling or staying asleep. Hormonal ups and downs are partly responsible. Plus, as you age, your sleep patterns may change. Older people may sleep less, awaken earlier and go to sleep sooner or later than they did at younger ages.
Lifestyle changes for coping with insomnia include:
- Sleep in a cool room to help relieve hot flashes that may be disturbing your sleep. In hot weather, you may want to lower your bedroom thermostat at night and use a small fan to keep air circulating.
- Exercise regularly.
- Set and keep a regular routine and hour for going to sleep.
- Drink a glass of warm milk right before bedtime but avoid other foods.
- Avoid alcoholic beverages or smoking before sleep.
- Avoid watching TV in bed (some programs are anything but relaxing!).
- Practice relaxation techniques like deep breathing.
- Review any medications you are taking to see if they may cause sleeplessness.
Mood swings
For reasons still not well understood, declining and fluctuating estrogen levels during the menopausal transition can cause emotional highs and lows and irritability. Lack of sleep due to night sweats may also contribute to feeling irritable and depressed. Though your periods are coming to an end, you may continue to experience the symptoms of premenstrual syndrome (PMS). In fact, emotional symptoms may become worse for some women as they approach menopause. You may also notice that you’ve lost interest in sex. Declining estrogen and changes in estrogen/testosterone ratios in women at this time may lower your sex drive.
Lifestyle strategies for coping with mood swings and sexuality concerns include:
- Make physical activity part of your schedule; exercise can improve mood and make you feel better about yourself.
- Try relaxation techniques such as meditation or massage, which can be calming and reduce irritability.
- Discuss your symptoms and what may be causing them with your partner; try different approaches to intimacy.
Vaginal dryness and frequent urinary tract infections.
Estrogen, a natural hormone produced by the body, helps keep the vagina lubricated and supple. Following menopause, as estrogen levels decline, the vagina becomes drier and the vaginal wall thins. Sex may become painful. The wall of the urethra becomes thinner, too, as estrogen levels fall, and increases the risk of more frequent urinary tract infections. Urine leakage may become a problem as muscle support for the bladder and urethra weakens. (This may also occur from strain on tissues as a result of childbirth).
Strategies for coping with vaginal dryness and frequent urinary infections include:
- Use nonhormonal vaginal creams or gels (prescription or nonprescription).
- If moisturizers and lubricants are not enough, vaginal estrogen (a prescription medication) is available as creams, rings or tablets.
- Drink plenty of water to help your body stay hydrated.
- Use long-lasting vaginal moisturizers.
- Exercising to maintain muscle tone.Practice Kegel techniques to strengthen the pelvic floor muscles that support the bladder and urethra. Kegel exercises help firm the vaginal canal, control urine flow and enhance orgasm. To make sure you know how to contract your pelvic floor muscles correctly, try to stop the flow of urine while you’re going to the bathroom. If you can do this, you’ve found the right muscles.To do Kegel exercises, empty your bladder and sit or lie down. Contract your pelvic floor muscles for three seconds, then relax for three seconds. Repeat 10 times. Once you’ve perfected the three-second contractions, try doing the exercise for four seconds at a time and then resting for four seconds, repeating 10 times. Gradually work up to keeping your pelvic floor muscles contracted for 10 seconds at a time, relaxing for 10 seconds in between. Aim to complete a set of 10 exercises, three times a day.
- Tell your health care professional about any medications you’re taking. Some may worsen vaginal dryness. Also, if you have a urinary tract infection, you may need antibiotics.
Heart palpitations.
Some women in their late 40s are frightened by their hearts beating fast in their chests for no apparent reason. This symptom, called a heart palpitation, is caused by the heart beating irregularly or missing one or two beats. Though this symptom can be associated with several types of serious heart-related conditions, it is also common during the transition to menopause and typically is not related to heart disease. For example, a woman’s heart rate can increase seven to 15 beats during a hot flash.
If you think you are experiencing heart palpitations:
- See your health care professional immediately if you have shortness of breath; pounding or irregular heartbeat; dizziness; nausea; pain in the neck, jaw, arm or chest that comes and goes; or tightness in the chest. Any could be a sign of a serious heart condition.
- Ask your health care professional to rule out conditions that may cause heart palpitations, such as thyroid disorders.
- Ask your health care professional about appropriate options for relieving heart palpitations, such as decreasing caffeine, and whether any medications are needed.
Forgetfulness or difficulty concentrating.
During and after the menopause transition, many women are troubled to find they have difficulty remembering things, experience mental blocks or have trouble concentrating. Not getting enough sleep or having sleep disrupted can contribute to memory and concentration problems. Stress associated with major life changes—such as caring for aging parents or having your children leave home—can also interfere with sleep. And recently, the Study of Women’s Health Across the Nation (SWAN), funded by the National Institute on Aging and published in the May 2009 issue of the journal Neurology, confirmed that there are real cognitive changes that take place in perimenopausal women, especially in the area of learning.
Researchers at the University of California Los Angeles looked at 2,362 women aged 42 to 52 and gave them tests of verbal memory, working memory and processing speeds at four different points in their menopause transitions: premenopause, early perimenopause, late perimenopause and postmenopause. They found that women do not learn as well in early or late perimenopause but regain their capacities to learn once menopause has been reached.
The study also uncovered a possible explanation. Researchers concluded that women taking hormones before their last period improved their cognitive skills, but for women who started hormones long after menopause, hormone therapy had a detrimental effect. However, you should still discuss the risks and benefits of hormone therapy with your health care professional. And keep in mind that although they can be upsetting, these memory-related issues are rarely associated with serious medical conditions such as Alzheimer’s disease.
Other strategies for coping with memory problems and lack of concentration include:
- Recognize that these symptoms may be caused by menopausal changes and aging and don’t put pressure on yourself.
- Rely on strategies for remembering things, such as developing daily reminder lists or messages to help get you through periods of forgetfulness.
- Practicestress-reduction techniques, such as deep breathing exercises, yoga and meditation, and try to be physically active on a regular basis.
If you find the strategies you’ve tried don’t relieve your discomfort, ask your health care professional about medical options. Medical strategies to relieve various menopausal symptoms include:
Oral contraceptives
Oral contraceptives can help ease symptoms associated with menopause, including irregular periods and mood swings, among others. Typically, oral contraceptives are recommended to women who are still having periods. For many women in their 40s, oral contraceptives provide the added benefit of preventing pregnancy.
Still, taking oral contraceptivess close to menopause can make it difficult to determine when you have stopped menstruating. Women who smoke, have high blood pressure, experience migraines associated with aura or have diabetes, a history of gall bladder disease or blood clotting disorders should not use oral contraceptives. Discuss your health history with your health care professional and ask for guidance on this treatment option.
If you’re considering taking hormones other than oral contraceptives to manage menopausal symptoms, be aware that the doses of estrogen and progesterone typically taken to manage menopausal symptoms are not adequate to provide protection against an unwanted pregnancy. A woman who is still fertile must use contraceptives containing higher levels of hormones or use additional birth control methods in addition to hormone replacement.
Antidepressant medication
The antidepressants venlafaxine (Effexor), fluoxetine (Prozac) and paroxetine (Paxil) may offer some relief for hot flashes. Antidepressants are not FDA-approved for the treatment of hot flashes, however.
Cardiovascular medication
Low doses of the blood pressure drugs clonidine (Catapres) or methyldopa (Aldomet) may also help ease hot flashes in some women. These drugs are not FDA-approved for hot flashes, however, and unpleasant side effects are common.
Menopausal Hormone Therapy
Menopausal hormone or estrogen therapy. Once prescribed as the first choice for the long-term prevention of osteoporosis and heart disease as well as for the short-term relief of menopausal symptoms such as hot flashes, hormone therapy is now only prescribed on a short-term basis (up to five years) for the management of menopausal symptoms in women without certain risk factors, such as a history of breast cancer, coronary artery disease and a previous blood clot or stroke.
Hormone therapy comes in several forms: synthetic or bioidentical estrogen, either alone or combined with progesterone or with a synthetic progestin. When combined with progestin, it is called hormone therapy (HT). It is given only to women who still have their uterus because progesterone reduces the risk of uterine cancer that comes with supplemental estrogen.
When given as estrogen alone, hormone therapy is called estrogen therapy (ET). It is typically given to women who no longer have a uterus.
Postmenopausal hormone therapy comes in a variety of forms: pills, creams, skin patches, vaginal rings and injections.
Some hormones are called “bioidentical,” meaning they are chemically, i.e., molecularly, identical to the substance as it occurs in your body. These hormones, however, don’t come from your body (or another woman’s body). Most bioidentical estrogens and progesterone come from soy (estrogen) or yams (progesterone).
They are also not “natural,” or in their natural state, when you take them. To create a hormone women can use, the plant or animal-based hormones are synthesized, or processed, through a several-step process in a laboratory.
While all hormonal supplements, including bioidenticals, are made in a laboratory, the difference between a bioidentical hormone and a synthetic hormone is that the synthetic hormone is a patented molecular compound created in the laboratory to mimic the action of naturally occurring hormones and mass produced. Prempro, for instance, is a combination of two synthetic hormones.
Synthetic and bioidentical hormones work in the same way: by binding in a kind of lock-and-key process to special proteins on cell surfaces called receptors. Once a hormone—whether synthetic or bioidentical—locks onto these receptors, the messages from that hormone can be transferred to the cell.
There are two main types of bioidentical hormones: those that are FDA-approved and commercially available with a prescription, such as Estrace, Climara, Vivelle, EstroGel, Divigel and Estrasorb, and those that are produced on an individual basis for women, in compounding pharmacies.
Estrogen products produced via compounding are typically called “bi-estrogen” or “tri-estrogen,” since they contain varying amounts of the two or three types of estrogen. The individual prescription is typically created based on a saliva test that identifies the forms of estrogen in which a woman may be deficient. Keep in mind that saliva tests do not accurately reflect the amount of circulating estrogen, as women’s estrogen levels vary day by day and at different times of the day and are not clinically useful for determining estrogen dosing.
A woman should not take any form of HT until she has weighed the pros and cons and discussed these risks and benefits with her doctor. Because of the potential risks that go along with HT, the U.S. Food and Drug Administration (FDA) now advises health care professionals to prescribe postmenopausal hormone therapies at the lowest possible dose and for the shortest possible length of time to achieve treatment goals.
This recommendation was made after findings from major studies of postmenopausal women with and without heart disease, conducted as part of the landmark federal Women’s Health Initiative (WHI), indicated that while estrogen and progestin are effective for short-term relief from hot flashes and night sweats, they have no significant impact on general health or quality of life factors, such as energy, mental health, symptoms of depression or sexual satisfaction.
Among other findings:
The National Cancer Institute found a significant drop in the rate of hormone-dependent breast cancers among women, the most common breast cancer, in 2003. In a study published in the New England Journal of Medicine in April 2007, researchers speculated that the drop was directly related to the fact that millions of women stopped taking hormone therapy in 2002 after the results of a major government study found the treatment slightly increased a woman’s risk for breast cancer, heart disease and stroke.
The researchers found that the decrease in breast cancer began in mid-2002 and leveled off after 2003. The decrease occurred in women over 50 and was marked in women with tumors that were estrogen receptor (ER) positive—cancers that require estrogen to grow. The researchers speculate that stopping the treatment prevented very tiny ER-positive cancers from growing (and in some cases, possibly helped them to regress) because they didn’t have the additional estrogen required to fuel their growth.
Results from the Women’s Health Initiative (WHI) published in 2002 showed that daily use of combined HT increases a woman’s chance of developing breast cancer by about 5 to 6 percent with each year of use. In other words, if 10,000 women took combined HT for a year, there would be about eight more cases of breast cancer per year than if they had not taken HT. The longer HT is used, the more the risk increases. In the same study, women who took HT also had a higher risk of breast cancer detected at a more advanced stage, and they were more likely to have breast changes seen on mammograms.
An update of the WHI study, published in October 2010, with 11 years of follow-up on the participants, showed that breast cancer had spread to the lymph nodes at a significantly higher rate in women taking combined estrogen-progestin than in nonusers. There was no difference in the rate of estrogen-receptor positive tumors between hormone users and nonusers.
However, researchers still have questions about the link between combined HT and breast cancer risk. Some experts theorize that part of the risk from combined HT may be due to the progestin. Researchers are currently looking into whether the progestin dose can be lowered to decrease the risk of breast cancer but still protect the endometrium.
Women who no longer have a uterus should take ET instead of HT because they don’t need a progestin to protect against uterine cancer, so there is no reason for them to increase their breast cancer risk by taking a progestin.
One piece of good news is that the risks associated with HT apply only to women who are currently taking or who have recently taken combined HT. Once a woman stops taking HT, her breast cancer risk drops to that of the general population (if she has no other risk factors).
The WHI also looked at women who had had a hysterectomy and whose ovaries had either stopped working or had been removed. Those who were taking ET only did not have an increased risk of breast cancer.
However, the “Million Women Study,” conducted in Britain, and numerous other similar studies have shown a slightly increased risk of breast cancer—about 1 to 3 percent with each year of use—in women who took ET. This is lower than the risk seen in women who took HT in the WHI study.
In addition:
- HT does not appear to help women with heart disease and may even make existing heart conditions worse. However, some research shows that ET may decrease the risk of heart disease when taken early in the postmenopausal years. A randomized, controlled clinical trial—called the Kronos Early Estrogen Prevention Study (KEEPS)—is currently exploring estrogen use in younger postmenopausal women.
- Research shows that HT can prevent bone loss after menopause, decreasing the risk of hip fractures related to osteoporosis.
- Older women taking HT have a higher risk of developing dementia, including Alzheimer’s disease, and, therefore, HT is not recommended after age 65.
Discuss the individual risks and benefits of hormone therapy with your health care professional. If you are considering hormone therapy, you may want to consider one of many low-dose HT preparations now available.
Alternatives to Hormone Therapy
For heart protection
Lifestyle strategies for cardiovascular health include exercise, not smoking, maintaining a healthy weight and limiting salt and alcohol. A balanced diet rich in vegetables, fruits and fish, and low in saturated fat can also provide some heart-health benefits.
Your health care professional may prescribe medication to reduce cholesterol and blood pressure levels and reduce your risk of heart disease.
For reduced sex drive.
Testosterone is a hormone that plays an important role in women’s bodies. Often thought of incorrectly as exclusively a male sex hormone, testosterone is secreted by the ovaries and adrenal gland and is natural to the female body. Surgical menopause (removal of the ovaries) may have a negative effect on sex drive, and testosterone therapy is sometimes prescribed to help.
Testosterone is not FDA approved for the treatment of low libido, however, and we don’t know what doses are appropriate for women. Too much testosterone may not help with sexual desire but may, instead, make you feel agitated, overly aggressive and/or depressed. Higher doses can cause masculinizing side effects that may not go away after stopping therapy, such as facial and body hair growth, acne, an enlarged clitoris, a lowered voice and muscle weight gain.
Testosterone may also be associated with adverse heart-related conditions, such as increased risk for atherosclerosis. There are currently no FDA-approved testosterone-alone preparations for women, although it is often prescribed “off-label” for women. There’s a specific prescription combination estrogen (esterified estrogens) and testosterone (oral methyltestosterone) pill called Syntest DS that may help combat testosterone deficiency.
Do not use Syntest if you have liver disease; a recent history of heart attack, stroke or circulation problems; a hormone-related cancer such as breast or uterine cancer; abnormal vaginal bleeding; or if you are pregnant or breast-feeding. It also increases your risk of endometrial hyperplasia, which may lead to cancer of the uterus.
Since the safety of taking testosterone for extended periods has not been established, women should be very cautious when considering this type of hormone treatment. Discuss the risks and benefits with your health care professional.
Osteoporosis.
Lifestyle changes shown to improve bone density in young women and prevent fractures in older women include dietary calcium and avoiding smoking and excessive alcohol consumption.
Additionally, several prescription drugs are available to treat and/or prevent osteoporosis.
Herbal Remedies
Some women report that vitamin and herbal supplements are helpful in managing menopausal symptoms. For instance, phytoestrogens—naturally occurring compounds in certain plants, herbs and seeds—are similar in chemical structure to estrogen and produce estrogen-like effects.
Soy products (tofu, tempeh, soy milk, soy burgers and roasted soy nuts), certain herbs (red clover) and legumes (chickpeas, lentils and various kinds of beans) contain specific types of phytoestrogens called isoflavones. These are healthy foods that are excellent sources of protein and calcium and can be added to your diet.
Some studies show that the isoflavones (weak, plant-derived estrogens) in soy foods and dietary supplements can reduce mild hot flashes. But most studies show they are no more effective than a placebo. Talk to your doctor before taking any form of isoflavones.
Black cohosh has been widely used in Europe for the treatment of hot flashes, and it has become more popular among U.S. women who want something to curb their hot flashes. The supplement’s safety record is good, but there is no real good research supporting its effectiveness in treating menopausal symptoms. Talk to your doctor about black cohosh before taking any form of the supplement.
There is also no scientific evidence to support the effectiveness of evening primrose oil, ginseng, kava, licorice, sage and dong quai root. Discuss any herbal or vitamin supplements you are considering taking with your health care professional. Bear in mind that studies related to their effectiveness are sparse, and the FDA doesn’t oversee the production of supplements and does not require manufacturers to prove their products are safe.
Also be aware that high doses of certain vitamins and herbal supplements can be dangerous. For example ephedra used in some weight-loss products has potentially serious side effects. Mixing herbal supplements with some prescription drugs can also be dangerous. So again, be sure to tell your health care professional everything you take.
Prevention
You can’t stop menopause, but you can prepare for its arrival. These strategies can help make your transition to menopause and your postmenopausal years healthy:
- Be prepared for how and why your body will change.
- Be informed about health issues after age 50.
- Develop a wellness plan that includes regular health screenings, regular exercise and a healthy diet throughout the years ahead.
- To improve your cardiovascular health and decrease your risk for osteoporosis, avoid smoking, weight gain, and excessive alcohol consumption. (Moderate drinking for women is defined as one drink per day equaling one 12-ounce bottle of beer or wine cooler; one 5-ounce glass of wine; or 1.5 ounces of 80 proof distilled spirits, according to the National Institute on Alcohol Abuse and Alcoholism. Anything beyond that is considered excessive.)
- Eat a balanced diet.
- Consider strength-training exercises and other weight-bearing exercises to increase your bone strength to prevent fractures as you age. Also consider taking dietary calcium and vitamin D, particularly if you’re over 65.
Women today don’t have to surrender to old age. Life after menopause can be as healthy, independent and fulfilling as any of the younger stages of a woman’s life; many postmenopausal women find their lives more satisfying.
Facts to Know
- After age 55, more than half of all deaths in women are caused by heart disease. And despite being thought of as a man’s disease, more women die from heart disease than men. Women can protect themselves against heart disease by not smoking, eating a healthy diet and getting regular exercise.
- There is a direct relationship between osteoporosis—a disease in which bones lose calcium and become brittle and more likely to fracture—and the lack of estrogen after menopause. Early menopause (before age 45) and any other extended period during which hormone levels are low and menstrual periods are absent can cause a decrease in bone mass.
- About 6,000 women in the United States reach menopause every day for a total of more than 2 million per year.
- In one study, 80 percent of women in menopause reported no decrease in quality of life, and 75 percent felt they had no loss in their attractiveness.
- According to the North American Menopause Society, most women—about 62 percent—report positive attitudes toward menopause.
- Some women continue to experience premenstrual syndrome (PMS) symptoms as they approach menopause. These symptoms can include swollen or tender breasts, bloating, nausea and moodiness.
- Fertility decreases gradually as menopause approaches. However, you can still get pregnant, even if your periods are irregular. A significant number of unintended pregnancies occur in women aged 40 to 44. Thus the need for reliable contraception remains important.
- As estrogen levels decline, vaginal tissue and tissue in the lower urinary tract become thinner, drier and less supple, causing painful intercourse and more frequent urinary tract infections in some women. Osteoporosis and heart disease are other consequences of declining estrogen levels in the decades following menopause.
- As you approach menopause, you may notice that you feel more irritable and moodier than usual. Some researchers believe this moodiness is due to the changes in your estrogen levels, but others think it may be more the result of the other symptoms that accompany menopause, such as hot flashes and fatigue, coupled with other stressors that often plague women in middle age. Severe depression, however, is not a symptom of menopause.
Key Q&A
- Will these menopause symptoms last for the rest of my life?For most women, menopause symptoms last for a relatively short time. However, a woman’s level of estrogen naturally remains low after menopause. This can affect many parts of the body, including the sexual and urinary organs, the heart and bones. So in that sense, the changes of menopause will be lifelong. But eating right, exercising and making other positive lifestyle changes can help you feel great and live a long, healthy life after menopause.
- What can be done to relieve pain during sex?Sexual penetration may be painful when there is not enough moisture in the vagina or when the tissue lining the vagina becomes fragile because of lower estrogen levels. The vaginal canal may actually shorten, and the opening may become more closed. Several methods are available to help. One of the most effective is frequent sexual activity. Other remedies include short-acting, water-based lubricants, such as Astroglide or K-Y lubricants, that supply moisture immediately before intercourse. Long-acting vaginal moisturizers are also available, while prescription estrogen-based vaginal creams, rings or tablets may also help. Lubricants described as “warming” or “stimulating” may cause vaginal or vulvar irritation.
- Since I began menopause, I’ve had an embarrassing problem—urine leaks when I laugh or cough. What can be done to prevent this?Some women have problems with bladder control after menopause begins. This happens because the muscles that surround the bladder and hold the urine inside become weaker as a woman ages. It may also be a result of strain during childbirth. Fortunately, simple exercises—known as Kegel exercises—can strengthen these muscles. To do Kegel exercises, empty your bladder and sit or lie down. Contract your pelvic floor muscles for three seconds, then relax for three seconds. Repeat 10 times. Once you’ve perfected the three-second contractions, try doing the exercise for four seconds at a time and then resting for four seconds, repeating 10 times. Gradually work up to keeping your pelvic floor muscles contracted for 10 seconds at a time, relaxing for 10 seconds in between. Aim to complete a set of 10 exercises, three times a day.Doing regular Kegels can markedly improve bladder control—and may even enhance sexual pleasure. Declining estrogen has been associated with worsening prolapse and incontinence.
- My health care professional has recommended hormone therapy, but I’ve heard that I’ll have menstrual periods again if I take it. Is that true? Is hormone therapy safe?Hormone therapy is only recommended for short-term use for women whose menopausal symptoms have become disruptive to their lives and cannot be controlled using nonhormonal approaches. Newer hormone therapy dosing schedules, which include both estrogen and progestogen daily, may cause some uterine bleeding or spotting for the first six months, but this bleeding eventually tapers off. If you experience bleeding while taking hormone therapy, talk to your health care professional; he or she may want to rule out other causes or change your dose to eliminate bleeding.Hormone therapy has been associated with some serious risks, especially in women with certain risk factors like a history of breast cancer or blood clots. Therefore, hormone therapy should always be used at the lowest effective dose and for the shortest amount of time to achieve treatment goals.
- Even though my eating habits have not changed, I’ve gained weight recently. Is that linked to menopause?It may be. Everyone’s metabolism begins to slow during the early to mid-30s. This change occurs gradually, so it may take a while for the impact of eating habits to affect weight. Also, many women notice a thickening around the waist after menopause. It is important to make a sensible, nutritious diet and healthy behaviors, such as getting enough exercise, goals for life. There is some evidence that eating a diet that includes lean protein, is low in fat and low in carbohydrates may help. The only reliable way to lose weight is to reduce caloric intake and increase caloric expenditure by exercising daily.
- I seem to be very forgetful lately and I’m worried. What’s happening?Many postmenopausal women have problems with short-term memory like forgetting the location of keys or eyeglasses, skipping appointments they didn’t remember or losing the end of a thought when speaking or writing. These may be due to a busy lifestyle and/or stress at home or work, aging and possibly, hormonal changes. Several medical studies have shown distinct differences in memory in women who have active ovaries producing estrogen or are taking estrogen therapy compared to women with low levels of estrogen due to menopause. These cognitive differences seem to be most pronounced in the years leading up to menopause, according results of a study published in the May 2009 issue of Neurology. The Study of Women’s Health Across the Nation (SWAN), funded by the National Institute on Aging, found a noticeable decline in cognitive skills in perimenopausal women, particularly in the area of learning. The women improved once they hit post-menopause, however, indicating that there is a time limit to the decline. The study also revealed that women who were taking hormones before their last period showed improvements in their ability to learn, suggesting that when taken in the years leading up to menopause, hormones may help prevent problems in learning and memory. After perimenopause, the hormones had a detrimental effect, however. If you notice a serious memory deficit, or are unable to remember what a common item is used for, consult your doctor, and if you are perimenopausal, discuss with him or her the possibility of hormone therapy.
- How will menopause affect my daily activities and lifestyle?That all depends on you. Menopause is a natural part of life, not a disease or a health crisis. However, menopause may occur when many other changes are happening in your life. For instance, your children may be marrying or leaving home, your parents may be ill or dying or you may be wondering what you’ll do when you retire. That’s why it is probably more helpful to think of how your daily activities and lifestyle could affect your postmenopausal years.For instance, making sure that you exercise and eat right can make a real difference in how you feel and can even help prevent some of the long-term effects that are linked to estrogen deficiency (like osteoporosis).Physical changes do occur with menopause and with aging. But the changes that happen during this period can be minimized by healthy living and a sense of purpose in life. If your symptoms are severe enough to interfere with your life, consult your doctor to go over your options for treatment.
For more information visit us our website: https://www.healthinfi.com
0 200


No Comments