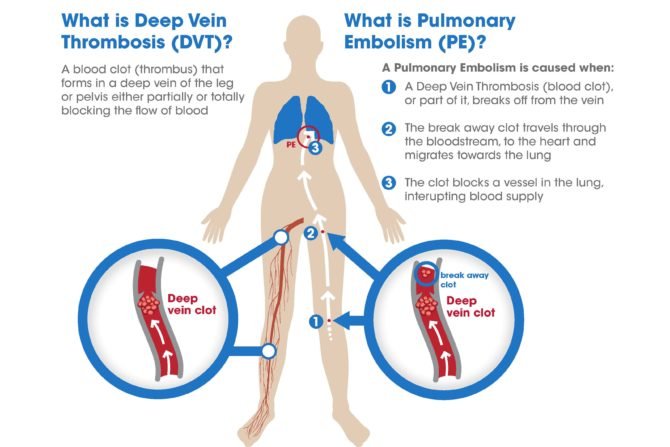
A deep vein thrombosis (DVT) involves the formation of a clot in the deep veins of the lower calf. The clot generally begins very low in the leg and grows in an upward direction to extend up to and past the knee. Some DVTs can rise to the level of the upper thigh, pelvis and even the lower abdomen. DVTs are considered dangerous because a piece of the clot can break off, travel up the patient’s vena cava and enter the patient’s lungs, resulting in a pulmonary embolism (PE).
A pulmonary embolism (PE) is dangerous because it can cut off the circulation to the lung vasculature, resulting in sudden cardiovascular collapse and often, sudden death within minutes. Of the 80 out of 100,000 people in the US who have a DVT each year, fifteen percent will develop a DVT. Of cases of sudden death, 3 percent are due to a PE.
In essence, the DVT generally comes first. People prone to a DVT include travelers who travel long distances and times without the ability to get up and move one’s legs. The moving of the legs triggers increased circulation in the legs, reducing the chance of a DVT. Travelers on long haul airline flights also get dehydrated from the dry air and lack of fluid intake, and are at an even higher risk than those traveling by other mechanisms.
Individuals who are obese, pregnant or elderly put themselves at higher risk for a DVT. Women who take birth control pills or estrogen replacement therapy are also at greater risk. In addition, those who have certain types of cancer secrete prothrombic agents that increase the chances of clotting within the body.
When a person develops a DVT, he or she might be asymptomatic. Alternatively, he or she may have symptoms, including redness or discoloration of the calf, pain in the back portion of the calf and an increase in swelling of the affected lower leg. Doctors can elicit a positive Homan’s sign by dorsiflexion (tipping upward toward the head) of the foot and asking the patient if they have increased pain in the posterior calf.
Furthermore, the doctor can check a d-dimer blood test—a test that determines the breakdown products of the clotting process. This can tell the doctor if there is clotting within the body. Imaging studies that prove the clotting is coming from a DVT include a Doppler ultrasound of the legs and a deep vein venogram, which employs the use of intravenous contrast dye and x-rays to determine the contour of the deep veins.
In treating a DVT, the doctor may order an IV infusion of TPA, also called tissue plasminogen activator. It is able to break up clots effectively and efficiently. It is reserved for severe cases of DVT. Lesser cases include treating the patient with intravenous heparin and pills consisting of Coumadin. The IV heparin works immediately to thin the blood. The clot breaks up through natural processes.
Coumadin takes longer to work effectively but, when it does work within a few days, the heparin can be stopped and the patient remains on Coumadin at home for a minimum of three months. Patients who have had multiple DVTs or a PE, may have to remain on Coumadin for longer periods of time and perhaps indefinitely.
As mentioned, when a blood clot from a DVT breaks off and travels to the lungs, it is called a PE. Doctors can prevent a DVT from becoming a PE by inserting a vena cava filter into the abdominal vena cava, thus preventing the clot from traveling past the filter.
When a PE does occur, the results can be catastrophic. If a clot straddles the opening to the pulmonary vessels of the lungs, it is called a “saddle embolism” and almost always results in death. Smaller clots will break off and settle in the smaller portions of the lungs.
The patient with a smaller PE will exhibit shortness of breath, anxiety, and chest pain that worsens with breathing deeply. Furthermore, the doctor will notice extra breath sounds heard with the stethoscope and will find low oxygen levels in the bloodstream. He can order a d-dimer test that can show if clotting is happening inside the body.
Imaging studies for proving a PE include a CT scan of the abdomen with IV contrast dye or an MRI of the chest. These tests can actually prove or disprove the presence or absence of a PE. A PE is considered a medical emergency and quick treatment is recommended.
Treatment includes eliciting the services of a vascular surgeon to perform a pulmonary embolectomy. The pulmonary embolectomy involves going into the vascular system and removing the clot directly. This can be a lifesaving procedure.
In addition, the doctor may order TPA in order to break up the clot. It works within minutes to dissolve any clot that is blocking the lung vasculature. If a person with a PE is completely stable, the doctor may order a trial of IV heparin and oral Coumadin, both of which are powerful blood thinners. They help the blood remain thin enough so the body can produce the enzymes necessary to dissolve the clot in a more natural way.
Coumadin, as mentioned, takes several days with which to work so it is taken along with the IV heparin until it can successfully thin the blood on its own. At that point, if the patient is otherwise healthy, the Coumadin is taken alone for at least three months.
A pulmonary embolism (PE) usually happens when a blood clot called a deep vein thrombosis(DVT), often in your leg, travels to your lungs and blocks a bloodvessel. That leads to low oxygen levels in your blood. It can damage the lung and other organs and cause heart failure, too.
A PE can be life-threatening, so if you’ve been diagnosed with DVT, you should be aware of this risk. Follow the treatment plan for your DVT to stop the clot from getting bigger and to keep new clots from forming.
Symptoms and Diagnosis
PE won’t always cause symptoms. You might have:
- Chest pain, which may get worse with a deep breath
- Sudden shortness of breath or rapid breathing
- Fast heartbeat
- Sudden cough
- Coughing up blood
- Lightheadedness or fainting
- Anxiety
Call 911 if you notice these symptoms. They could also be symptoms of a heart attack, pneumonia, or other serious problems.
Your doctor may want to check different types of X-rays and lung tests to find a PE.
Treatment and Prevention
Depending on your symptoms, your doctor may give you a drug called a thrombolytic to dissolve the clot. These medicines can save your life, but they can also cause bleeding that’s hard to stop. You’ll have to be in the hospital, and the staff will watch you carefully.
For some very serious cases, a specialist may need to do surgery to break up and remove the clot.
If your symptoms aren’t life-threatening, or if using a thrombolytic would be too dangerous, your doctor will give you medication that interrupts the clotting process or stops platelets in your blood from sticking together. They don’t break down the clot, but they’ll keep it from getting bigger while your body works on dissolving it.
Afterward, you’ll probably take a blood thinner pill for at least 3 months. If your doctor prescribes warfarin (Coumadin), you’ll need to get your blood tested often to make sure you have the right amount of the drug in your system. You won’t need blood tests if you take a newer blood thinner, such as apixaban (Eliquis), dabigatran (Pradaxa), edoxaban (Savaysa), or rivaroxaban (Xarelto).
You and your doctor should figure out what may have caused your DVT, so you can take steps to avoid getting more clots.
The heart pumps oxygenated blood through the aorta to smaller arteries. After the blood supplies nutrients to vital organs, it returns through veins for reoxygenation in the lungs. Blood clots called deep vein thrombi (DVT) often develop in the deep leg veins. Pulmonary embolism (PE) occurs when clots break off from vein walls and travel through the heart to the pulmonary arteries. The broader term venous thromboembolism (VTE) refers to DVT, PE, or to a combination of both.
The arterial (red) and venous systems (blue) are depicted. The left ventricle (LV) ejects oxygenated blood into the aorta, which circulates blood to vital organs. Deoxygenated blood travels through the venous system to the right atrium, right ventricle, and pulmonary artery. Adapted with permission from MediClip, Clinical Cardiopulmonary Images 1997, CCP01026.TIF, Williams & Wilkins, Baltimore, Md.
What Is the Epidemiology?
VTE poses a public health threat with an estimated incidence in the United States of 250 000 to 2 million cases per year. Predisposition to VTE arises from acquired conditions, inherited disorders, or both. Many of the acquired risk factors can be modified, thus lessening the likelihood of PE or DVT.
What Are the Acquired Risk Factors?
Long-haul air travel is the most talked-about risk factor for PE. Other acquired risk factors include obesity, cigarette smoking, hypertension, immobilization, surgery, and trauma. Chronic medical illnesses such as congestive heart failure, chronic obstructive pulmonary disease, and cancer also predispose to PE. PE is also a prominent women’s health issue. Risk factors include oral contraceptives, pregnancy, and hormone replacement therapy.
What Are the Inherited Disorders?
Heredity plays an important role in a patient’s susceptibility to PE. We are just beginning to develop genetic tests (such as factor V Leiden and the prothrombin gene mutation) that can identify those who are predisposed. The presence of these risk factors is sometimes called a prothrombotic or thrombophilic state.
How Is the Diagnosis Established?
DVT most often originates in the calf, with a persistent cramping or “charley horse” that intensifies over several days. Leg swelling and discoloration may accompany the increase in discomfort. Upper-extremity DVT may cause otherwise unexplained upper arm or neck swelling. The most frequently used diagnostic imaging test is the noninvasive venous ultrasound examination.
Many patients with PE have a vague sense that something is wrong but have difficulty defining or describing the problem. Consequently, they often delay seeking medical attention. At times, because symptoms are so vague and nonspecific, medical professionals will diagnose anxiety rather than PE. To establish the diagnosis of PE, the most frequently used noninvasive imaging test is the rapid-speed chest computed tomography (CT) scan.
What Are the Warning Signals of PE?
- Unexplained shortness of breath (the most common symptom of PE)
- Chest discomfort, usually worse with a deep breath or coughing
- A general sense of anxiety or nervousness
- Lightheadedness or blacking out
What Should I Expect at the Hospital?
Definitely Expect:
- Questions about symptoms of chest or leg discomfort, breathing difficulties, or lightheadedness
- Questions about whether you or your family members have suffered prior VTE
- A check of your blood pressure, pulse rate, breathing rate, heart, lungs, and legs
- An ECG and chest x-ray
Possibly Expect:
- A blood test (D-dimer) that screens for PE (If results are normal, PE is extremely unlikely.)
- A chest CT scan, which directly images blood clots causing blockages in the pulmonary arteries
- A lung scan, which indirectly identifies areas of decreased blood flow in the lung tissue as a consequence of PE
- Blood tests to detect a prothrombotic state, especially in relatively young and otherwise healthy patients with PE or DVT
What Treatment Will I Receive?
PE can range from mild to severe. Mild PE is managed with blood thinners (anticoagulation). Severe PE requires additional measures, such as clot busters (thrombolytic therapy) or embolectomy, a procedure in which the clot is removed with either a catheter or surgery.
Anticoagulation begins with a combination of 2 blood thinners: (1) heparin, administered intravenously or by injection, and (2) warfarin, an oral blood thinner. Heparin comes in 2 principal forms. The traditional unfractionated form ordinarily requires intravenous administration. There is no fixed dose for this type of heparin. Instead, the dose is titrated to a blood test called the partial thromboplastin time. This blood test is usually performed several times daily for the first few days and then once daily thereafter. More recently, low-molecular-weight heparins have begun replac-ing unfractionated heparin. Low-molecular-weight heparins are ordinarily prescribed in proportion to the patient’s weight, require no blood testing, and necessitate injection once or twice daily.
We overlap heparin treatment with warfarin until the oral blood thinner becomes effective, usually after 5 to 10 days of combined therapy. We determine the proper dose of warfarin by a blood test reported as the International Normalized Ratio (INR). The target INR range is usually between 2.0 and 3.0. Interactions with food, alcohol, and other drugs can dramatically alter the INR. Sometimes, major fluctuations in the INR occur for no apparent reason. Too high an INR may result in bleeding as a side effect. Too low an INR may result in recurrent clotting. Patients may need their INR checked every few weeks or months, according to the stability of the readings. It is important for patients to keep a record of their values over time.
PE is usually treated in the hospital with intravenous unfractionated heparin as a bridge to warfarin. In contrast, DVT can often be managed successfully on an outpatient basis with low-molecular-weight heparin injections as a bridge to oral anticoagulation with warfarin. The most controversial area in VTE therapy is the optimal duration of warfarin anticoagulation. The current recommendation is usually at least 6 months of anticoagulation, but it can sometimes be longer, according to individual patient circumstances.
In patients who cannot tolerate anticoagulation or those for whom anticoagulation fails, a permanent metal filter is inserted into the inferior vena cava, the largest vein below the heart, to prevent large blood clots from reaching the pulmonary arteries and causing PE. Unfortunately, the filter devices do not halt the clotting process. Their presence predisposes to future venous clots on or below the filter.
Prevention
Maintaining ideal body weight with a healthy nutritional program and exercise regimen will generally reduce the likelihood of venous thrombosis. Specific other measures are shown below:
- To prevent immobility or inactivity: Walk, jog, bicycle, or swim.
- To prevent obesity: Limit caloric intake, exercise, and avoid saturated fats.
- To prevent VTE during air travel: Drink extra water, walk if feasible, wear vascular compression stockings, and avoid alcohol.
- To quit cigarette smoking: Use nicotine patch, gum, or spray, or consider the prescription drug bupropion.
- To control hypertension: Self-check blood pressure, and report elevated readings to primary care provider.
- To deal with a known genetic predisposition to VTE: Alert your healthcare provider about the family history and any abnormal blood tests related to a clotting tendency.
- To prevent VTE after trauma or surgery: Discuss with the treating physician the implementation of measures such as mechanical compression boots for the legs and/or blood thinners given either intravenously or as injections.
- To prevent VTE during a hospitalization precipitated by a medical condition: Discuss with the treating physician measures such as mechanical compression boots for the legs and/or blood thinners given either intravenously or as injections.
- To prevent VTE when planning birth control: Discuss VTE risks, and consider alternatives to oral contraceptives.
- To prevent VTE during pregnancy: Consider daily self-injected heparin if considered at high risk of VTE.
- To prevent VTE during hormone replacement therapy: Keep in mind that VTE risks with hormone replacement therapy are similar to those of oral contraceptives.
For more information visit us our website: https://www.healthinfi.com
0 200


1 Comment