What is E. Coli and Coli bacteria?
What is the medical definition of E. coli?
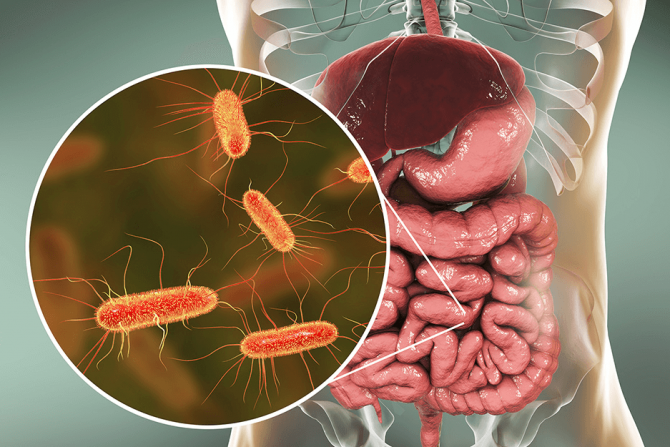
Colitis gram-negative bacteria found worldwide. Many subtypes of this bacterial species cause a wide variety of diseases in humans. The bacteria can be transmitted person-to-person and by contaminated food and water.
Escherichia coli (E. coli) bacteria normally live in the intestines of healthy people and animals. Most varieties of E. coli are harmless or cause relatively brief diarrhea. But a few particularly nasty strains, such as E. coli O157: H7, can cause severe abdominal cramps, bloody diarrhea, and vomiting.
You may be exposed to E. coli from contaminated water or food — especially raw vegetables and undercooked ground beef. Healthy adults usually recover from infection with E. coli O157: H7 within a week, but young children and older adults have a greater risk of developing a life-threatening form of kidney failure called hemolytic uremic syndrome.
E Coli Infection: Symptoms, Causes, and Treatment
Symptoms
Coli infects the intestine and causes symptoms that range from non-presenting to severe.
Symptoms of infection with E. coli 0157 typically appear 3 to 4 days after being exposed to the bacteria. However, symptoms may appear as early as 24 hours or as late as 1 week later.
These can include:
- abdominal pain or severe abdominal cramping, often starting suddenly
- watery diarrhea, beginning a few hours after the pain begins
- bright red bloody stools around a day later, resulting from the toxin’s damage to the intestines
- nausea and, in some cases, vomiting
- in some cases, fever, usually below 101 degrees Fahrenheit
- fatigue, resulting from dehydration and the loss of fluids and electrolytes
Signs and symptoms of E. coli O157: H7 infection typically begin three or four days after exposure to the bacteria, though you may become ill as soon as one day after to more than a week later. Signs and symptoms include:
- Diarrhea, which may range from mild and watery to severe and bloody
- Abdominal cramping, pain or tenderness
- Nausea and vomiting, in some people
Some people have no noticeable symptoms, but they can spread the infection to others.
Causes
Among the many strains of E. coli, only a few trigger diarrhea. One group of E. coli — which includes O157: H7 — produces a powerful toxin that damages the lining of the small intestine, which can cause bloody diarrhea. You develop an E. coli infection when you ingest this strain of bacteria.
Unlike many other disease-causing bacteria, E. coli can cause an infection even if you ingest only small amounts. Because of this, you can be sickened by E. coli from eating a slightly undercooked hamburger or from swallowing a mouthful of contaminated pool water.
Potential sources of exposure include contaminated food or water and person-to-person contact.
The most common cause of an E. coli infection is contact with human or animal feces (the bacteria is found in stools). This contact can come about in several different ways, including the following:
- Working with animals such as cows, goats, and sheep
- Eating undercooked meat or raw vegetables (Meat can become contaminated with E. coli during the slaughtering process.)
- Drinking unpasteurized milk or contaminated water (for example, drinking lake water while swimming)
- Contact with the feces of infected people (for example, while changing a diaper)
- Unsafe and improper food preparation (not washing hands before cooking food, unclean work surfaces in the kitchen)
In addition, E. coli infections can be spread from person to person in settings such as a daycare center or a nursing home.
Contaminated food
The most common way to acquire an E. coli infection is by eating contaminated food, such as:
- Ground beef. When cattle are slaughtered and processed, E. coli bacteria in their intestines can get on the meat. Ground beef combines meat from many different cattle, increasing the risk of contamination.
- Unpasteurized milk. E. coli bacteria on a cow’s udder or on milking equipment can get into raw milk.
- Fresh produce. Runoff from cattle farms can contaminate fields where fresh produce is grown. Certain vegetables, such as spinach and lettuce, are particularly vulnerable to this type of contamination.
Contaminated water
Human and animal feces may pollute ground and surface water, including streams, rivers, lakes and water used to irrigate crops. Although public water systems use chlorine, ultraviolet light or ozone to kill E. coli, some outbreaks have been linked to contaminated municipal water supplies.
Private wells are a greater cause for concern because they don’t often have any disinfecting system. Rural water supplies are the most likely to be contaminated. Some people also have been infected after swimming in pools or lakes contaminated with feces.
Personal contact
Coli bacteria can easily travel from person to person, especially when infected adults and children don’t wash their hands properly. Family members of young children with E. coli infection are especially likely to acquire it themselves. Outbreaks have also occurred among children visiting petting zoos and in animal barns at county fairs.
Risk factors
Some people who are more likely to be affected by E. coli– related illness.
People with a weakened immune system are more prone to complications. This includes patients with AIDS, those taking immunosuppressive medications, and people receiving chemotherapy.
Patients with decreased stomach acid, either due to stomach surgery or medicines that lower stomach acid, have a higher risk of infection.
Young children and older people have a higher risk of developing serious illness and complications.
coli can affect anyone who is exposed to the bacteria. But some people are more likely to develop problems than are others. Risk factors include:
- Age. Young children and older adults are at higher risk of experiencing illness caused by E. coli and more-serious complications from the infection.
- Weakened immune systems. People who have weakened immune systems — from AIDS or drugs to treat cancer or prevent the rejection of organ transplants — are more likely to become ill from ingesting E. coli.
- Eating certain types of food. Riskier foods include undercooked hamburger; unpasteurized milk, apple juice or cider; and soft cheeses made from raw milk.
- Time of year. Though it’s not clear why, the majority of E. coli infections in the U.S. occur from June through September.
- Decreased stomach acid levels. Stomach acid offers some protection against E. coli. If you take medications to reduce your levels of stomach acid, such as esomeprazole (Nexium), pantoprazole (Protonix), lansoprazole (Prevacid) and omeprazole (Prilosec), you may increase your risk of an E. coli infection.
Risky foods
- Cook hamburgers until they’re 160 F. Hamburgers should be well-done, with no pink showing anywhere in the meat. But color isn’t a reliable indicator of whether or not meat is done cooking. Meat — especially if grilled — can brown before it’s completely cooked.
That’s why it’s important to use a meat thermometer to ensure that meat is heated to at least 160 F (71 C) at its thickest point.
- Drink pasteurized milk, juice and cider. Any boxed or bottled juice kept at room temperature is likely to be pasteurized, even if the label doesn’t say so.
- Wash raw produce thoroughly. Washing produce won’t necessarily get rid of all E. coli — especially in leafy greens, which provide many spots for the bacteria to attach themselves to. Careful rinsing can remove dirt and reduce the amount of bacteria that may be clinging to the produce.
Avoid Cross-Contamination
- Wash utensils. Use hot soapy water on knives, countertops and cutting boards before and after they come into contact with fresh produce or raw meat.
- Keep raw foods separate. This includes using separate cutting boards for raw meat and foods, such as vegetables and fruits. Never put cooked hamburgers on the same plate you used for raw patties.
- Wash your hands. Wash your hands after preparing or eating food, using the toilet, or changing diapers. Make sure that children also wash their hands before eating, after using the bathroom and after contact with animals.
Complications
Most healthy adults recover from E. coli illness within a week. Some people — particularly young children and older adults — may develop a life-threatening form of kidney failure called hemolytic uremic syndrome.
Complications
Most people make a full recovery within a week.
However, around 10 percent of people are at risk of developing hemolytic uremic syndrome (HUS). These are mostly young children and older people.
HUS is characterized by hemolysis, or a breakup of red blood cells. This can cause anemia, a low platelet count, and kidney failure.
Platelets, the blood cells responsible for blood clotting, clump together within the small blood vessels of the kidneys, resulting in reduced blood flow, or ischemia.
This can eventually lead to kidney failure. Decreased platelets increase the risk of bleeding problems.
Patients with these clots can also develop central nervous system (CNS) problems that affect the brain and spinal cord.
This can lead to seizures, paralysis, brain swelling, and coma. It is fatal in 3 to 5 percent of cases.
Acute kidney failure among infants and young children is usually caused by HUS.
HUS usually starts about 5 to 8 days after the onset of diarrhea. It is a medical emergency and requires hospital treatment.
Prevention
No vaccine or medication can protect you from E. coli-based illness, though researchers are investigating potential vaccines. To reduce your chance of being exposed to E. coli, avoid risky foods and watch out for cross-contamination. Top of form bottom of Form
Escherichia coli (E. coli) is a bacterium commonly found in the gut of warm-blooded organisms.
Most strains of E. coli are not harmful but are part of the healthful bacterial flora in the human gut. However, some types can cause illness in humans, including diarrhea, abdominal pain, fever, and sometimes vomiting.
coliO157: H7 is one of the strains, and produces a toxin known as Shiga. It is one of the most powerful toxins, and it can cause an intestinal infection.
Some 265,000 Shiga toxin-producing E. coli (STEC) infections occur each year in the United States (U.S.). Around 36 percent of these are probably caused by E. coli O157: H7. When a foodborne outbreak occurs, it usually involves a Shiga toxin-producing E. coli.
Most people recover within 6 to 8 days, but it can be life-threatening in infants and people with a weakened immune system.
Some other types of E. coli infection can lead to urinary tract infections, respiratory illness, pneumonia, and other illnesses like meningitis.
Fast facts on E. coli
Treatment
There is no cure for E. coli O157: H7. It has to resolve itself. Antibiotics are not advised. They may increase the risk of HUS.
Patients should get plenty of rest and drink a lot of water to prevent dehydration.
Over-the-counter (OTC) medications for diarrhea are not recommended, as they can slow down the digestive system, undermining the body’s ability to eliminate the toxins efficiently.
The only way your doctor can know for sure if you have an E. coli infection is to send a sample of your stool to a lab to be analyzed.
Fortunately, the infection usually goes away on its own.
For some types of E.coli associated with diarrhea, such as the watery travelers’ diarrhea, antibiotics can shorten the length of time you have symptoms and might be used in moderately severe cases.
But if you have fever or bloody diarrhea or if your doctor suspects Shiga toxin-producing E. coli, antibiotics should not be taken. They can actually increase the production of Shiga toxin and worsen your symptoms.
It’s important to rest and get plenty of fluids to replace what your body is losing through vomiting or diarrhea.
Don’t take over-the-counter medications that fight diarrhea. You don’t want to slow down your digestive system, because that will delay your body’s shedding of the infection.
When you start to feel better, stick to low-fiber foods at first such as:
- Crackers
- Toast
- Eggs
- Rice
Dairy products and foods that are high in fat or fiber can make your symptoms worse.
Urine infection
Coli bacteria are a common cause of urine infections, for example, cystitis. The exit of the urinary tract is near the anus, and so the bacteria can spread from the GI tract to the urinary tract.
Wiping from front to back can help reduce the risk.
Causes
Most strains of E. coli are harmless, but some produce a toxin that makes humans sick.
The group of E. coli that includes 0157:H7 produces a potent toxin called Shiga. This toxin can harm the lining of the small intestine.
Humans can become infected by:
Swallowing contaminated water: Tap water in the US is treated and contains chlorine, but some E. coli outbreaks have been caused by contaminated municipal water supplies.
Private wells can be a source of infection, as can some lakes and swimming pools.
Travelers to places where water may be untreated should be careful when drinking water, using ice or eating vegetables washed in water of uncertain origin.
Swallowing contaminated food: Possible sources include undercooked ground beef, unpasteurized milk, juice, cider, or cheese, alfalfa sprouts or raw vegetables.
Infected people who work in restaurants and do not wash their hands properly after going to the toilet can spread the infection to customers and other members of staff.
Person-to-person contact: Good hand hygiene is important in stopping the spread of infection.
Contact with animals: Bacteria can spread in farms, petting zoos, and fairs.
Diagnosis
Drinking plenty of water to avoid dehydration is crucial during an E. coli infection
The doctor will identify the signs, ask about symptoms, and send a stool sample to a lab for analysis.
The sample must be taken within 48 hours after the bloody diarrhea starts.
Prevention
Some tips can help prevent infection with E. Coli and other pathogens.
These include:
- cooking meat well, especially ground meat
- drinking pasteurized milk, apple juice, and cider, rather than unpasteurized
- washing vegetables, especially leafy green ones
- ensuring that cutlery and crockery are thoroughly washed with warm, soapy water
- storing meat and non-meat foods separately, and using separate cutting boards
- following good hand-hygiene practices
Good hand hygiene involves washing hands thoroughly with warm water and soap regularly, and especially after using the bathroom, after changing diapers, before and after preparing foods, and after touching animals.
0 200

No Comments