About Ectopic Pregnancy
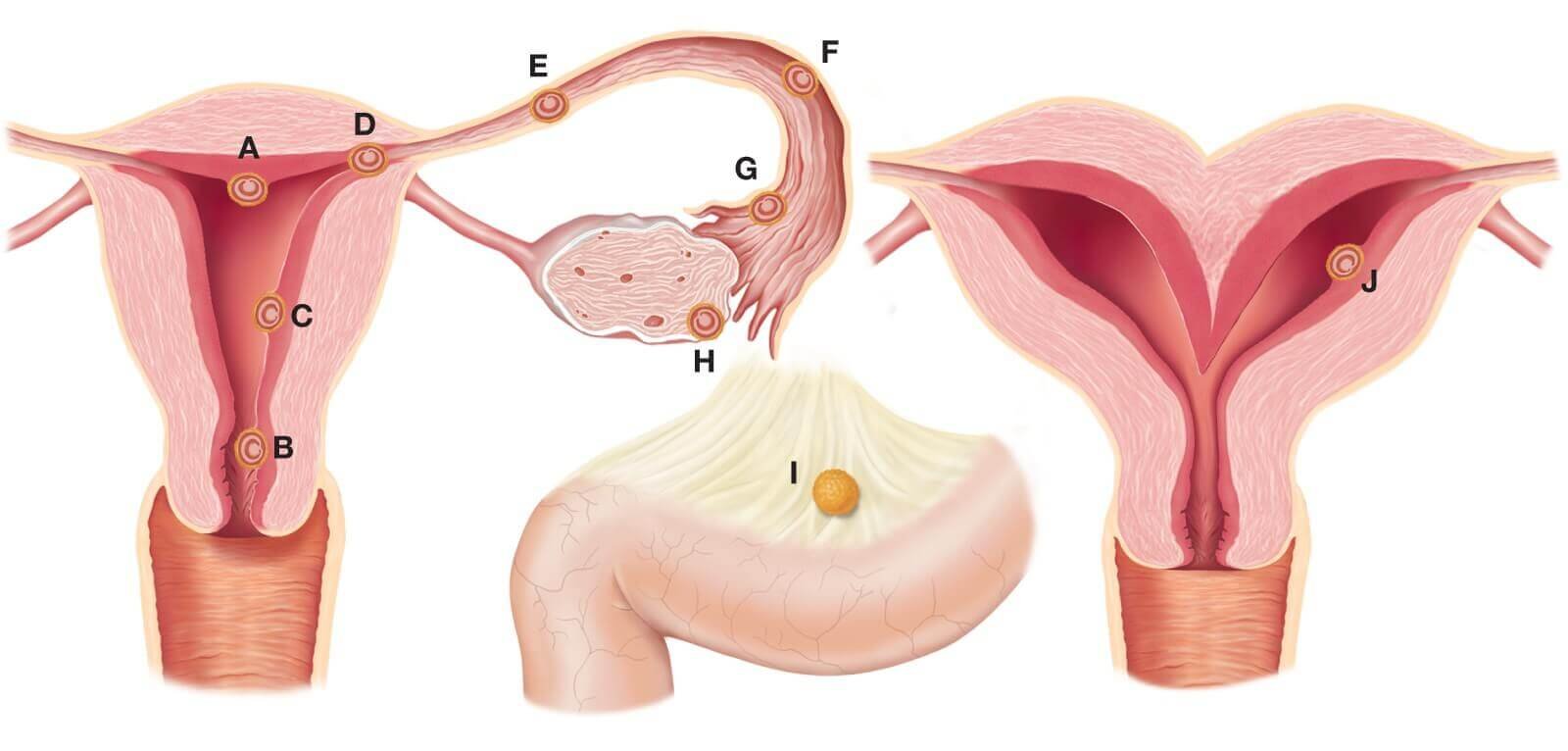
In a normal pregnancy, the fertilized egg implants and develops in the uterus. In most ectopic pregnancies, the egg settles in the fallopian tubes. This is why ectopic pregnancies are commonly called “tubal pregnancies.” The egg also can implant in the ovary, abdomen, or the cervix, so you also might hear these referred to as cervical or abdominal pregnancies.
None of these areas has as much space or nurturing tissue as a uterus for a pregnancy to develop. As the fetus grows, it will eventually burst the organ that contains it. This can cause severe bleeding and endanger the mother’s life. A classical ectopic pregnancy does not develop into a live birth.
For pregnancy to happen, the ovary has to release an egg into the fallopian tube, where it stays for about 24 hours. There it has to come in contact with a sperm to be fertilized. The fertilized egg stays in the fallopian tube for 3 or 4 days before it heads to the uterus. There it attaches to the lining and continues to grow until a baby is born.
But if the fertilized egg implants in your fallopian tube or somewhere else in your abdomen, you end up with what’s called an ectopic pregnancy. In these cases, the pregnancy can’t continue normally, and it requires emergency treatment.
Symptoms
Ectopic pregnancy can be difficult to diagnose because symptoms often are like those of a normal early pregnancy. These can include missed periods, breast tenderness, nausea, vomiting, fatigue, or frequent urination (peeing).
Often, the first warning signs of an ectopic pregnancy are pain or vaginal bleeding. There might be pain in the pelvis, abdomen, or even the shoulder or neck (if blood from a ruptured ectopic pregnancy builds up and irritates certain nerves). The pain can range from mild and dull to severe and sharp. It might be felt on just one side of the pelvis or all over.
Any of these symptoms also might happen with an ectopic pregnancy:
- vaginal spotting
- dizziness or fainting (caused by blood loss)
- low blood pressure (also caused by blood loss)
- lower back pain
Most of the time, an ectopic pregnancy happens within the first few weeks of pregnancy. You might not even know you’re pregnant and may not have signs of a problem.
Light vaginal bleeding and pelvic pain are usually the first symptoms, but others could include:
- Nausea and vomiting with pain
- Sharp abdominal cramps
- Pain on one side of your body
- Dizziness or weakness
- Pain in your shoulder, neck, or rectum
Nausea and breast soreness are common symptoms in both ectopic and uterine pregnancies. The following symptoms are more common in an ectopic pregnancy and can indicate a medical emergency:
- sharp waves of pain in the abdomen, pelvis, shoulder, or neck
- severe pain that occurs on one side of the abdomen
- light to heavy vaginal spotting or bleeding
- dizziness or fainting
- rectal pressure
You should contact your doctor or seek immediate treatment if you know that you’re pregnant and have any of these symptoms.
Ectopic pregnancy can lead to fallopian tube rupture. If that happens, you could have major pain with or without severe bleeding. Or the bleeding could be internal. Call your doctor immediately if you have heavy vaginal bleeding that causes lightheadedness, fainting, or shoulder pain, or if you have any severe abdominal pain, especially if it is on one side of the belly.
Emergency symptoms
If the fertilized egg continues to grow in the fallopian tube, it can cause the tube to rupture. Heavy bleeding inside the abdomen is likely. Symptoms of this life-threatening event include extreme lightheadedness, fainting, severe abdominal pain, and shock.
Causes
An ectopic pregnancy usually happens because a fertilized egg wasn’t able to quickly move down the fallopian tube into the uterus. An infection or inflammation of the tube might have partially or entirely blocked it. Pelvic inflammatory disease (PID), which can be caused by gonorrhea or chlamydia, is a common cause of fallopian tube blockage.
A tubal pregnancy — the most common type of ectopic pregnancy — happens when a fertilized egg gets stuck on its way to the uterus, often because the fallopian tube is damaged by inflammation or is misshapen. Hormonal imbalances or abnormal development of the fertilized egg also might play a role.
You may never know why you have an ectopic pregnancy. One cause could be a damaged fallopian tube. It could prevent the fertilized egg from getting into your uterus, leaving it to implant in the fallopian tube or somewhere else.
Endometriosis (when cells from the lining of the uterus implant and grow elsewhere in the body) or scar tissue from previous abdominal or fallopian surgeries also can cause blockages. More rarely, birth defects can change the shape of the tube and hurt the egg’s progress.
But you are more likely to have an ectopic pregnancy if you have any of the following:
- Pelvic inflammatory disease (PID)
- Sexually-transmitted diseases
- Scarring from previous pelvic surgeries
- History of ectopic pregnancy
- Unsuccessful tubal ligation or tubal ligation reversal
- Use of fertility drugs
- Infertility treatments such as in vitro fertilization (IVF)
It could also happen if you become pregnant with an intrauterine device (IUD) in place.
The cause of an ectopic pregnancy isn’t always clear. In some cases, the following conditions have been linked with an ectopic pregnancy:
- inflammation and scarring of the fallopian tubes from a previous medical condition, infection, or surgery
- hormonal factors
- genetic abnormalities
- birth defects
- medical conditions that affect the shape and condition of the fallopian tubes and reproductive organs
Your doctor may be able to give you more specific information about your condition.
Diagnosis
If your doctor thinks you have an ectopic pregnancy, she will probably perform some tests, including a pregnancy test and a pelvic exam. An ultrasound test may be performed to view the uterus’ and fallopian tubes’ condition.
If she confirms you have an ectopic pregnancy, she will talk to you about the best treatment based on your medical condition and your future plans for pregnancy.
If you go to the emergency department because of abdominal pain, you’ll probably be given a urine pregnancy test. Although these tests aren’t sophisticated, they are fast — and speed can be crucial in treating ectopic pregnancy.
If you already know you’re pregnant, or if the urine test comes back positive, you may have a quantitative HCG test. This blood test measures levels of the hormone human chorionic gonadotropin (HCG), which is made by the placenta.
You also may have an ultrasound to look for a developing fetus in the uterus or elsewhere. Early in pregnancy, the ultrasound may be done using a wand-like device in your vagina. The doctor might give you a pelvic exam to locate the areas causing pain; to check for an enlarged, pregnant uterus; or to find any masses outside of the uterus.
Even with the best equipment, it’s hard to see a pregnancy less than 5 weeks after the last menstrual period. If your doctor can’t diagnose ectopic pregnancy but can’t rule it out, he or she may ask you to return every few days for blood work and an ultrasound until it is clear whether or not there is an ectopic pregnancy.
A pelvic exam can help your doctor identify areas of pain, tenderness, or a mass in the fallopian tube or ovary. However, your doctor can’t diagnose an ectopic pregnancy by examining you. You’ll need blood tests and an ultrasound.
Pregnancy test
Your doctor will order the human chorionic gonadotropin (HCG) blood test to confirm that you’re pregnant. Levels of this hormone increase during pregnancy. This blood test may be repeated every few days until ultrasound testing can confirm or rule out an ectopic pregnancy — usually about five to six weeks after conception.
Ultrasound
Transvaginal ultrasound
A transvaginal ultrasound allows your doctor to see the exact location of your pregnancy. For this test, a wandlike device is placed into your vagina. It uses sound waves to create images of your uterus, ovaries and fallopian tubes, and sends the pictures to a nearby monitor.
Abdominal ultrasound, in which an ultrasound wand is moved over your belly, also may be used to confirm your pregnancy or evaluate for internal bleeding.
Other blood tests
A complete blood count will be done to check for anemia or other signs of blood loss. If you’re diagnosed with an ectopic pregnancy, your doctor may also order tests to check your blood type in case you need a transfusion.
Treatment
A fertilized egg can’t develop normally outside the uterus. To prevent life-threatening complications, the ectopic tissue needs to be removed. Depending on your symptoms and when the ectopic pregnancy is discovered, this may be done using medication, laparoscopic surgery or abdominal surgery.
Medication
An early ectopic pregnancy without unstable bleeding is most often treated with a medication called methotrexate, which stops cell growth and dissolves existing cells. The medication is given by injection. It’s very important that the diagnosis of ectopic pregnancy is certain before receiving this treatment.
After the injection, your doctor will order another HCG test to determine how well treatment is working, and if you need more medication.
Laparoscopic procedure
In other cases, an ectopic pregnancy can be treated with laparoscopic surgery. In this procedure, a small incision is made in the abdomen, near or in the navel. Next, your doctor uses a thin tube equipped with a camera lens and light (laparoscope) to view the tubal area.
The ectopic pregnancy is removed and the tube is either repaired (salpingostomy) or removed (salpingectomy).
Which procedure you have depends on the amount of bleeding and damage and whether the tube has ruptured.
How is methotrexate given?
Methotrexate often is given by injection in one dose. Before you take methotrexate, blood tests will be done to measure the level of HCG and the functions of certain organs. If HCG levels have not decreased enough after the first dose, another dose of methotrexate may be recommended. You will have careful follow-up over time until HCG is no longer found in your blood.
Side effects
Taking methotrexate can have some side effects. Most women have some abdominal pain. Vaginal bleeding or spotting also may occur. Other side effects may include
- nausea
- vomiting
- diarrhea
- dizziness
It is important to follow up with your ob-gyn or other health care professional until your treatment with methotrexate is complete. The risk of a fallopian tube rupture does not go away until your treatment is over. Seek care right away if you have symptoms of a rupture, including sudden abdominal pain, shoulder pain, or weakness.
Treatments
Because a fertilized egg can’t survive outside of the uterus, the tissue has to be removed to keep you from having serious complications. Two methods are used to treat it: medication and surgery.
Medication. If your fallopian tube hasn’t ruptured and your pregnancy hasn’t progressed very far, your doctor can give you an injection of methotrexate (Trexall). It stops the cells from growing, and your body will simply absorb them. Most ectopic pregnancies can be treated with methotrexate if they’re caught early.
Surgery. In other cases, surgery is required. The most common is laparoscopy. Your doctor will make very small incisions in your lower abdomen and insert a thin, flexible instrument (laparoscope) to remove the ectopic pregnancy. If your fallopian tube is damaged, she may have to remove it as well.If you’re bleeding heavily or your doctor suspects your fallopian tube is ruptured, you might need emergency surgery with a larger incision. This is called laparotomy.
After an Ectopic Pregnancy
There is a good chance you can have a normal pregnancy again, but it might be hard. You should consider talking to a fertility specialist early, especially if you had a fallopian tube removed.
And talk to your doctor about how long to wait before trying again. Some doctors suggest at least 3 to 6 months. If you’ve already had an ectopic pregnancy, your chances of having another one go up.
What About Future Pregnancies?
Many women who have had an ectopic pregnancy will go on to have normal pregnancies in the future, but some will have difficulty becoming pregnant again. This difficulty is more common in women who also had fertility problems before the ectopic pregnancy. It depends on a woman’s fertility before the ectopic pregnancy, as well as the extent of any damage that happened.
A woman who has had one ectopic pregnancy has about a 15% chance of having another.
Risk for an Ectopic Pregnancy?
While any woman can have an ectopic pregnancy, the risk is higher for women who are older than 35 and those who have had:
- PID
- a previous ectopic pregnancy
- surgery on a fallopian tube
- infertility problems or medication to stimulate ovulation
Some things that make you more likely to have an ectopic pregnancy are:
- Previous ectopic pregnancy. If you’ve had this type of pregnancy before, you’re more likely to have another.
- Inflammation or infection. Sexually transmitted infections, such as gonorrhea or chlamydia, can cause inflammation in the tubes and other nearby organs, and increase your risk of an ectopic pregnancy.
- Fertility treatments. Some research suggests that women who have in vitro fertilization (IVF) or similar treatments are more likely to have an ectopic pregnancy. Infertility itself may also raise your risk.
- Tubal surgery. Surgery to correct a closed or damaged fallopian tube can increase the risk of an ectopic pregnancy.
- Choice of birth control. The chance of getting pregnant while using an intrauterine device (IUD) is rare. However, if you do get pregnant with an IUD in place, it’s more likely to be ectopic. Tubal ligation, a permanent method of birth control commonly known as “having your tubes tied,” also raises your risk, if you become pregnant after this procedure.
- Smoking. Cigarette smoking just before you get pregnant can increase the risk of an ectopic pregnancy. The more you smoke, the greater the risk.
Some birth control methods also can affect a woman’s risk of ectopic pregnancy. Those who become pregnant while using an intrauterine device (IUD) might be more likely to have an ectopic pregnancy. Smoking and having multiple sexual partners also increase the risk of an ectopic pregnancy.
When to Call Your Doctor
If you believe you’re at risk for an ectopic pregnancy, meet with your doctor to discuss your options before you become pregnant. You can help protect yourself against a future ectopic pregnancy by not smoking and by always using condoms when you’re having sex but not trying to get pregnant. Condoms can protect against sexually transmitted infections (STDs) that can cause PID.
If you are pregnant and have any concerns about the pregnancy being ectopic, talk to your doctor — it’s important to make sure it’s detected early. You and your doctor might want to plan on checking your hormone levels or scheduling an early ultrasound to ensure that your pregnancy is developing normally.
Call your doctor immediately if you’re pregnant and experiencing any pain, bleeding, or other symptoms of ectopic pregnancy. When it comes to detecting an ectopic pregnancy, the sooner it is found, the better.
Seek emergency medical help if you have any signs or symptoms of an ectopic pregnancy, including:
- Severe abdominal or pelvic pain during pregnancy
- Abnormal vaginal bleeding
- Extreme lightheadedness or fainting
- Other concerning symptoms, especially if you have risk factors for an ectopic pregnancy
Warning
Often, the first warning sign of an ectopic pregnancy is pelvic pain. Light vaginal bleeding may also occur.
If blood leaks from the fallopian tube, you may feel increasing abdominal pain, an urge to have a bowel movement or pelvic discomfort. If heavy bleeding (hemorrhaging) occurs, you may feel shoulder pain as blood fills your pelvis and abdomen. Your specific symptoms depend on where the blood collects and which nerves are irritated.
Complications
An ectopic pregnancy can cause your fallopian tube to burst open. Without treatment, the ruptured tube can lead to life-threatening bleeding.
Prevention
There’s no way to prevent an ectopic pregnancy, but here are some ways to decrease your risk:
- Limit your number of sexual partners.
- Always use a condom during sex to help prevent sexually transmitted infections and reduce your risk of pelvic inflammatory disease.
- Don’t smoke. If you do, quit before you try to get pregnant.
Glossary
Assisted Reproductive Technology: A group of infertility treatments in which an egg is fertilized with a sperm outside the body; the fertilized egg then is transferred to the uterus.
Endometriosis: A condition in which tissue that lines the uterus is found outside of the uterus, usually on the ovaries, fallopian tubes, and other pelvic structures.
Fallopian Tube: Tube through which an egg travels from the ovary to the uterus.
General Anesthesia: The use of drugs that produce a sleep-like state to prevent pain during surgery.
Hormone: A substance made in the body by cells or organs that controls the function of cells or organs.
In Vitro Fertilization (IVF): A procedure in which an egg is removed from a woman’s ovary, fertilized in a laboratory with the man’s sperm, and then transferred to the woman’s uterus to achieve a pregnancy.
Laparoscopy: A surgical procedure in which an instrument called a laparoscope is inserted into the pelvic cavity through a small incision. The laparoscope is used to view the pelvic organs. Other instruments can be used with it to perform surgery.
Obstetrician-Gynecologist (Ob-Gyn): A physician with special skills, training, and education in women’s health.
Pelvic Inflammatory Disease: An infection of the uterus, fallopian tubes, and nearby pelvic structures.
Sexually Transmitted Infections (STIs): Infections that are spread by sexual contact, including chlamydia, gonorrhea, human papillomavirus (HPV), herpes, syphilis, and human immunodeficiency virus (HIV, the cause of acquired immunodeficiency syndrome [AIDS]).
Ultrasound Exam: A test in which sound waves are used to examine internal structures. During pregnancy, it can be used to examine the fetus.
Uterus: A muscular organ located in the female pelvis that contains and nourishes the developing fetus during pregnancy.
0 200



No Comments