Hepatitis is a very broad term describing the liver inflammation. This can be cause be several different mechanisms. Hepatitis is caused by a viral infection of the liver. Depending of the type of the virus, we know of Hepatitis A, B, C, D and E, with Hepatitis C being the most problematic.
Hepatitis C is an infectious disease caused by Hepatitis C Virus (HCV). HCV is a small virus consisting of viral RNA found in the core of the virus, as seen from the picture, and an envelope that protects the virus. Hepatitis C is a disease caused by a virus that infects the liver. In time, it can lead to cirrhosis, liver cancer, and liver failure.
When HCV enters human bloodstream it floats into the liver where it starts to replicate by using human liver cells to create new viruses. This causes liver inflammation that is in turn followed by liver cirrhosis. In short, what Hepatitis C is doing to the liver is scarring them and slowly disabling the function the liver performs. This action can in the end lead to liver cancer that can only be treated by surgically replacing the liver via liver transplant.
On the upside, there are viable treatments for Hepatitis C, based on interferon medication. However, the medications are becoming more and more evolved which lead to the invention of Sofosbuvir – the first all-oral Hep C therapy.
What is hepatitis C is hence best described as a virus infection that causes liver damage and eventually liver failure. The disease is commonly asymptomatic – that means that there are no apparent symptoms such as pain or fever. However, if patient is closely observed there are some symptoms that can suggest Hepatitis C infection.
With more than 170 million estimated patient around the world, the New Sofosbuvir treatment of Hep C is very important. If Hep C is rapidly treated, the following problems with liver surgery can be effectively avoided.Many people don’t know that they have hepatitis C until they already have some liver damage. This can take many years. Some people who get hepatitis C have it for a short time and then get better. This is called acute hepatitis C. But most people who are infected with the virus go on to develop long-term, or chronic, hepatitis C.
Although hepatitis C can be very serious, most people can manage the disease and lead active, full lives.
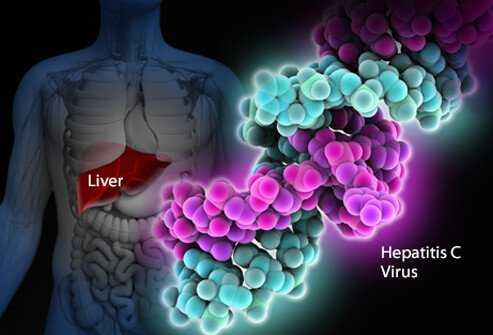
What causes hepatitis C infection?
Hepatitis C is caused by the hepatitis C virus. It is spread by contact with an infected person’s blood.
- You share needles and other equipment used to inject illegal drugs. This is the most common way to get hepatitis C in the United States.
- You had a blood transfusion or organ transplant before 1992. As of 1992 in the United States, all donated blood and organs are screened for hepatitis C.
- You get a shot with a needle that has infected blood on it. This happens in some developing countries where they use needles more than once when giving shots.
- You get a tattoo or a piercing with a needle that has infected blood on it. This can happen if equipment isn’t cleaned properly after it is used.
In rare cases, a mother with hepatitis C spreads the virus to her baby at birth, or a health care worker is accidentally exposed to blood that is infected with hepatitis C.
The risk of getting hepatitis C through sexual contact is very small.1 The risk is higher if you have many sex partners.You cannot get hepatitis C from casual contact such as hugging, kissing, sneezing, coughing, or sharing food or drink.
What are the symptoms?
Most people have no symptoms when they are first infected with the hepatitis C virus. If you do develop symptoms, they may include:
- Feeling very tired.
- Joint pain.
- Belly pain.
- Itchy skin.
- Sore muscles.
- Dark urine.
- Yellowish eyesand skin (jaundice). Jaundice usually appears only after other symptoms have started to go away.
Most people go on to develop chronic hepatitis C but still don’t have symptoms. This makes it common for people to have hepatitis C for 15 years or longer before it is diagnosed.
How is hepatitis C diagnosed?
Many people find out by accident that they have the virus. They find out when their blood is tested before a blood donation or as part of a routine checkup. Often people with hepatitis C have high levels of liver enzymes in their blood.
If your doctor thinks you may have hepatitis C, he or she will talk to you about having a blood test. If the test shows hepatitis C antibodies, then you have had hepatitis C at some point. A second test can tell if you still have hepatitis C.
When blood tests show that you have hepatitis C, you may need a liver biopsy to see how well your liver is working. During a liver biopsy, a doctor will insert a needle between your ribs to collect a small sample of livertissue to look at under a microscope. You may also have imaging tests, such as a CT scan, MRI, or ultrasound, to make sure that you don’t have liver cancer.
Some people prefer to find out on their own if they have been exposed to hepatitis C. You can buy a home test called a Home Access Hepatitis C Check kit at most drugstores. If the test shows that you have been exposed to the virus in the past, be sure to talk to your doctor to find out if you have the virus now.
Getting tested
Early diagnosis can prevent health problems that may result from infection and prevent transmission of the virus. WHO recommends screening for people who may be at increased risk of infection.
Populations at increased risk of HCV infection include:
- people who inject drugs;
- people who use intranasal drugs;
- recipients of infected blood products or invasive procedures in health-care facilities with inadequate infection control practices ;
- children born to mothers infected with HCV ;
- people with sexual partners who are HCV-infected;
- people with HIV infection;
- prisoners or previously incarcerated persons; and
- people who have had tattoos or piercings.
About 2.3 million people of the estimated 36.7 million living with HIV globally have serological evidence of past or present HCV infection. Conversely, among all HIV-infected persons, the prevalence of anti-HCV was 6.2%. Liver diseases represent a major cause of morbidity and mortality among persons living with HIV.
How is it treated?
You and your doctor need to decide if you should take antiviral medicine to treat hepatitis C. It may not be right for everyone.
If you do take medicine, the best treatment is a combination of medicines that fight infection. An example is dasabuvir, ombitasvir, paritaprevir, and ritonavir. How well these medicines work depends on how damaged your liver is, how serious your infection is, and what type of hepatitis C you have.
Taking care of yourself is an important part of the treatment for hepatitis C. Some people with hepatitis C don’t notice a change in the way they feel. Others feel tired, sick, or depressed. You may feel better if you exercise and eat healthy foods. To help prevent further liver damage, avoid alcohol and illegal drugs and certain medicines that can be hard on your liver.
Treatment
Hepatitis C does not always require treatment as the immune response in some people will clear the infection, and some people with chronic infection do not develop liver damage. When treatment is necessary, the goal of hepatitis C treatment is cure. The cure rate depends on several factors including the strain of the virus and the type of treatment given.
The standard of care for hepatitis C is changing rapidly. Sofosbuvir, daclatasvir and the sofosbuvir/ledipasvir combination are part of the preferred regimens in the WHO guidelines, and can achieve cure rates above 95%. These medicines are much more effective, safer and better-tolerated than the older therapies. Therapy with DAAs can cure most persons with HCV infection and treatment is shorter (usually 12 weeks). Meanwhile, there remains a limited role for pegylated interferon and ribavirin in certain scenarios where currently data are limited in supporting DAA-only therapies. Although the production cost of DAAs is low, these medicines remain very expensive in many high- and middle-income countries. Prices have dropped dramatically in some countries (primarily low-income) due to the introduction of generic versions of these medicines.
Access to HCV treatment is improving, but remains limited. In 2015, of the 71 million persons living with HCV infection globally, 20% (14 million) knew their diagnosis. 7.4% of those diagnosed (1.1 million) were started on treatment in 2015. Much needs to be done to ensure that these advances lead to greater access to treatment globally.
Prevention
There is no vaccine for hepatitis C, therefore prevention of HCV infection depends upon reducing the risk of exposure to the virus in health-care settings and in higher risk populations, for example, people who inject drugs, and through sexual contact.
The following list provides a limited example of primary prevention interventions recommended by WHO:
- hand hygiene: including surgical hand preparation, hand washing and use of gloves;
- safe and appropriate use of health care injections;
- safe handling and disposal of sharps and waste;
- provision of comprehensive harm-reduction services to people who inject drugs including sterile injecting equipment;
- testing of donated blood for hepatitis B and C (as well as HIV and syphilis);
- training of health personnel; and
- promotion of correct and consistent use of condoms.
Secondary and tertiary prevention
For people infected with the hepatitis C virus, WHO recommends:
- education and counselling on options for care and treatment;
- immunization with the hepatitis A and B vaccines to prevent coinfection from these hepatitis viruses and to protect their liver;
- early and appropriate medical management including antiviral therapy if appropriate; and
- regular monitoring for early diagnosis of chronic liver disease.
Screening, care and treatment of persons with hepatitis C infection
In April 2016, WHO updated its “Guidelines for the screening, care and treatment of persons with chronic hepatitis C”. These guidelines complement existing WHO guidance on the prevention of transmission of bloodborne viruses, including HCV.
They are intended for policy-makers, government officials, and others working in low- and middle-income countries who are developing programmes for the screening, care and treatment of people with HCV infection. These guidelines will help expand of treatment services to patients with HCV infection, as they provide key recommendations in these areas and discuss considerations for implementation.
Transmission
The hepatitis C virus is a bloodborne virus. It is most commonly transmitted through:
- injecting drug use through the sharing of injection equipment;
- the reuse or inadequate sterilization of medical equipment, especially syringes and needles in healthcare settings; and
- the transfusion of unscreened blood and blood products.
HCV can also be transmitted sexually and can be passed from an infected mother to her baby; however these modes of transmission are much less common.
Hepatitis C is not spread through breast milk, food, water or by casual contact such as hugging, kissing and sharing food or drinks with an infected person.
Estimates obtained from modelling suggest that worldwide, in 2015, there were 1.75 million new HCV infections (globally, 23.7 new HCV infections per 100 000 people).
For more information visit us our website: https://www.healthinfi.com
3 500


No Comments