What is Fabry Disease?
Fabry disease is a rare genetic disorder that prevents the body from making an enzyme called alpha-galactosidase A.
This enzyme is responsible for breaking down a type of fat called globotriaosylceramide (Gb3 or GL-3) into building blocks that the body’s cells can use.
Fabry disease is an inherited disorder that results from the buildup of a particular type of fat, called globotriaosylceramide, in the body’s cells. Beginning in childhood, this buildup causes signs and symptoms that affect many parts of the body.
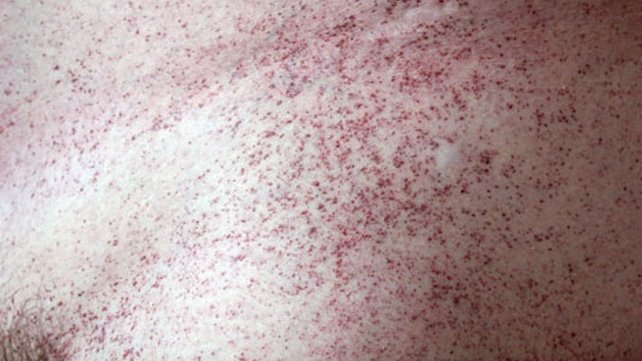
Characteristic features of Fabry disease include episodes of pain, particularly in the hands and feet (acroparesthesias); clusters of small, dark red spots on the skin called angiokeratomas; a decreased ability to sweat (hypohidrosis); cloudiness or streaks in the front part of the eye (corneal opacity or corneal verticillata); problems with the gastrointestinal system; ringing in the ears (tinnitus); and hearing loss.
Fabry disease also involves potentially life-threatening complications such as progressive kidney damage, heart attack, and stroke. Some affected individuals have milder forms of the disorder that appear later in life and affect only the heart or kidneys.
When these fat molecules are not broken down due to lack of alpha-galactosidase, they build up inside the cells and cause damage. The disease has a wide range of symptoms, including life-threatening ones such as heart attack, stroke, and kidney disease. But children with Fabry disease often live into adulthood and can have a good quality of life with the proper care.
Symptoms of Fabry disease
Symptoms are typically first experienced in early childhood and can be very difficult to understand; the rarity of Fabry disease to many clinicians sometimes leads to misdiagnoses. Manifestations of the disease usually increase in number and severity as individual ages.
Pain
Full body or localized pain to the extremities (known as acroparesthesia) or gastrointestinal (GI) tract is common in patients with Fabry disease. This pain can increase over time. This acroparesthesia is believed to be related to the damage of peripheral nerve fibers that transmit pain. GI tract pain is likely caused by the accumulation of lipids in the small vasculature of the GI tract which obstructs blood flow and causes pain.
Kidney
Kidney complications are a common and serious effect of the disease; chronic kidney disease and kidney failure may worsen throughout life. The presence of protein in the urine (which causes foamy urine) is often the first sign of kidney involvement. End-stage kidney failure in those with Fabry disease typically occurs in the third decade of life and is a common cause of death due to the disease.
Heart
Fabry disease can affect the heart in several ways. The accumulation of sphingolipids within heart muscle cells causes an abnormal thickening of the heart muscle or hypertrophy. This hypertrophy can cause the heart muscle to become abnormally stiff and unable to relax, leading to restrictive cardiomyopathy causing breathlessness.
Fabry disease can also affect the way in which the heart conducts electrical impulses, leading to both abnormally slow heart rhythms such as complete heart block, but also abnormally rapid heart rhythms such as ventricular tachycardia. These abnormal heart rhythms can cause blackouts, palpitations, or even sudden cardiac death.
Sphingolipids can also build up within the heart valves, thickening the valves and affecting the way they open and close. If severe, this can cause the valves to leak (regurgitation) or to restrict the forward flow of blood (stenosis). The aortic and mitral valves are more commonly affected than the valves on the right side of the heart.
Skin
Angiokeratomas (tiny, painless papules that can appear on any region of the body, but are predominant on the thighs, around the belly button, buttocks, lower abdomen, and groin) are common.
Anhidrosis (lack of sweating) is a common symptom, and less commonly hyperhidrosis (excessive sweating).
Additionally, patients can exhibit Raynaud’s disease-like symptoms with neuropathy (in particular, burning extremity pain).
Ocular involvement may be present showing cornea verticillata (also known as vortex keratopathy), i.e. clouding of the corneas.
Keratopathy may be the presenting feature in asymptomatic patients and must be differentiated from other causes of vortex keratopathy (e.g. drug deposition in the cornea). This clouding does not affect vision.
You may notice things like:
- Pain and burning in your hands and feet that get worse with exercise, fever, and hot weather or when you are tired
- Small, dark red spots usually found between your belly button and knees
- Cloudy vision
- Hearing loss
- Ringing in the ears
- Sweating less than normal
- Stomach pain, bowel movements right after eating
Fabry disease can have many symptoms because it affects cells throughout the body. The symptoms include:
- Chronic pain usually a burning or a tingling sensation in the hands and feet. The pain sometimes briefly becomes more intense, requiring medication to bring it down to manageable levels. The pain can go away in adulthood.
- Clusters of small, dark red spots in various locations on the skin.
- Opaque corneas, resulting in cloudy-looking eyes and problems with eyesight.
- Ringing in the ears, and hearing loss.
- Kidney damage, which worsens over time, becoming serious.
- Increased risk of life-threatening heart attacks and stroke.
- A variety of gastrointestinal problems.
- A decreased ability to sweat.
Fabry disease can lead to more serious problems, especially in men. These can include:
- Higher chance of heart attack or stroke
- Serious kidney problems, including kidney failure
- High blood pressure
- Heart failure
- Enlarged heart
- Osteoporosis
These symptoms usually appear in infancy or childhood, though in rarer mild cases they will begin in adulthood and be less severe.
Other ocular findings can include conjunctival and retinal vascular abnormalities and anterior/posterior spoke-like cataracts. Visual reduction from these manifestations is uncommon.
Cause of Fabry disease
You get Fabry disease from your parents. It’s passed down through genes.
The problem is that your body can’t make an enzyme called alpha-galactosidase A, which you need to break down fatty substances like oils, waxes, and fatty acids. When you have Fabry disease, you either were born without that enzyme or it doesn’t work right.
Fabry disease is caused by a mutation of the GLA gene, which encodes for the alpha-galactosidaseA enzyme. The mutation usually makes the enzyme unable to function, although in mild cases, it may function to some degree.
Fabry disease is caused by mutations in the GLA gene. This gene provides instructions for making an enzyme called alpha-galactosidase A. This enzyme is active in lysosomes, which are structures that serve as recycling centers within cells. Alpha-galactosidase A normally breaks down a fatty substance called globotriaosylceramide.
Mutations in the GLA gene alter the structure and function of the enzyme, preventing it from breaking down this substance effectively. As a result, globotriaosylceramide builds up in cells throughout the body, particularly cells lining blood vessels in the skin and cells in the kidneys, heart, and nervous system. The progressive accumulation of this substance damages cells, leading to the varied signs and symptoms of Fabry disease.
GLA gene mutations that result in an absence of alpha-galactosidase activity lead to the classic, severe form of Fabry disease. Mutations that decrease but do not eliminate the enzyme’s activity usually cause the milder, late-onset forms of Fabry disease that typically affect only the heart or kidneys.
The disease is inherited in an X-linked dominant manner, which means that the gene involved is situated on the X chromosome.
Because women have two X chromosomes, they usually have a milder form of the disease or, in rare cases, no symptoms at all. But there is a 50 percent risk of a woman passing a mutated gene onto their children. A son who inherits a mutation will develop the disease since he will not have a second X chromosome that could compensate for the mutation.
In contrast, all of the daughters of a man with Fabry disease will inherit it, while none of his sons will.
Diagnosis of Fabry disease
At first, Fabry disease can resemble normal growing pains or arthritis, but other symptoms start to appear with time.
Fabry disease is suspected based on the individual’s clinical presentation and can be diagnosed by an enzyme assay (usually done on leukocytes) to measure the level of alpha-galactosidase activity. An enzyme assay is not reliable for the diagnosis of disease in females due to the random nature of X-inactivation.
Molecular genetic analysis of the GLA gene is the most accurate method of diagnosis in females, particularly if the mutations have already been identified in male family members. Many disease-causing mutations have been noted. A kidney biopsy may also be suggestive of Fabry disease if excessive lipid buildup is noted.
Pediatricians, as well as internists, commonly misdiagnose Fabry disease. All immediate and extended family members in the same family have the same family mutation, so if one member of a family has a DNA sequence analysis performed, other members of the family can be diagnosed by performing a targeted sequence analysis instead of testing the entire gene.
Targeted sequencing is quicker and less expensive to perform. One study reported that for every first diagnosis in a family, on average 5 more family members (immediate and extended) are also diagnosed.
MRI is accurate in accessing left ventricular mass and thickness and hypertrophy. Late gadolinium enhancement shows an increased signal of the midwall at the inferolateral wall of the base of the left ventricle, usually in the non-hypertrophied ventricle.
T1-weighted imaging can show a low T1 signal due to sphingolipid storage in the heart even without ventricular hypertrophy in 40% of those affected by the disease. Thus MRI is a useful way of diagnosing the disease early. T2 signal is increased in inflammation and edema.
Fabry can be confirmed with a test measuring levels of alpha-galactosidase. If doctors find low levels of the enzyme, they may ask for genetic testing for the mutated GLA gene. Genetic testing may also be recommended for close family members who do not show any symptoms.
Treatment of Fabry disease
There are two options available for treatment. The most common has been enzyme replacement therapy (ERT) which replaces the enzyme that is missing or not working correctly. This allows your body to break down fatty acid substances the way it should.
It will also help ease the pain and other symptoms that Fabry disease causes. You will probably visit an outpatient center every few weeks to get the enzyme injected into a vein.
A newer option is oral medication migalastat (Galafold). It differs from ERT in that it works to stabilize the enzymes which are not working. This also helps ease the effects of the disease on your organs.
For the most part, the treatment of Fabry disease focuses on medications that improve the patient’s quality of life. Pain relievers, including Tegretol and Dilantin, are used to combat episodes of intense pain. Gastrointestinal problems may be remedied with pancrelipase.
Other medications are used to prevent symptoms from becoming life-threatening. Heart and anti-clotting medications may be used along with pacemakers to prevent heart attacks. Angiotensin-converting enzyme (ACE) inhibitors and angiotensin receptor blockers (ARBs) are used to combat kidney disease. In more advanced stages of kidney disease, dialysis or a kidney transplant are options.
Special diets that cut back on fats and salts may also be considered because they can reduce the intensity of some symptoms.
The U.S. Food and Drug Administration has approved enzyme replacement therapies that give patients forms of alpha-galactosidase, the enzyme they are missing. This treatment reduces symptoms and improves patients’ health. Researchers continue to study its long-term effects.
Your doctor may recommend that you also take:
- Drugs to relieve pain (prescription or nonprescription)
- Medicine for stomach problems
- Blood thinners or other drugs for an irregular heartbeat or other heart problems
- Blood pressure medicine, which also helps protect your kidneys
Fabry disease facts
- Fabry disease is a rare genetic disease with a deficiency of an enzyme called alpha-galactosidase A. The disease affects many parts of the body including the skin, eyes, gastrointestinal system, kidney, heart, brain, and nervous system.
- Symptoms of Fabry disease include:
- Episodes of pain and burning sensations
- Dark red spots on the skin
- Decreased ability to sweat
- Cloudiness of the eye
- Gastrointestinal (GI) problems
- Ringing in the ears
- Hearing loss
- Mitral valve prolapse
- Joint pain
- Back pain in the kidney area
- Fabry disease is caused by a defect on the X chromosome. X-linked genetic mutations tend to occur mostly in males, and rarely in females.
- It’s estimated that it affect1 1 in 40,000 males in the US.
- The disease is diagnosed with a test that measures leukocyte alpha-Gal A enzyme activity.
- Treatment for Fabry disease includes enzyme replacement therapy along with medications to treat and prevent other symptoms of the disease. Kidney transplants may be needed in severe cases when renal failure
- The life expectancy of males with Fabry disease is about 58 years, and the life expectancy of females with the disease is just over 75 years.
Signs and symptoms include:
- Episodes of pain and burning sensations in the hands and feet (acroparesthesias) that can be triggered by exercise, stress, fatigue, fever, or changes in weather
- Small, dark red spots on the skin (angiokeratomas), mostly in clusters from the belly button to the knees
- Decreased ability to sweat
- Cloudiness of the front part of the eye
- Problems with the gastrointestinal system
- Ringing in the ears (tinnitus)
- Hearing loss
- Mitral valve prolapse
- Abdominal discomfort
- Frequent bowel movements after eating
- Joint pain
- Back pain in the kidney area
Complications of Fabry disease include kidney damage, heart disease, and heart attack, and strokes.
Complications of Fabry disease
One potential complication of FD is an end-stage renal disease (ESRD). ESRD can be deadly if you aren’t treated with dialysis or a kidney transplant. Almost all males with FD develop ESRD. But only about 10 percent of females with FD develop ESRD.
For people who are treated to control ESRD, heart disease is a major cause of death.
1 250

No Comments