About Bilirubin Encephalopathy
Causes. Expand Section. Bilirubin encephalopathy (BE) is caused by very high levels of bilirubin. Bilirubin is a yellow pigment that is created as the body gets rid of old red blood cells. High levels of bilirubin in the body can cause the skin to look yellow (jaundice),
The toxic effects of bilirubin on the brain are called bilirubin encephalopathy. The various symptoms of bilirubin encephalopathy are a direct consequence of the damage done to particular neural tissues in the developing brain by bilirubin crossing the blood-brain barrier. Bilirubin toxicity is expressed mostly in the deeper areas of the brain, especially the basal ganglia, hippocampus and the cerebellum, as well as the brainstem. The lesions caused by bilirubin have the effect of causing various disorders of movement and hearing.
Laboratory experiments suggest that developing nerve cells are most susceptible to bilirubin poisoning. Thus, the exact state of development when hyperbilirubinemia occurs influences the kind and severity of the effects on the infant affected. In addition, the levels of bilirubin, especially unbound bilirubin, that are reached and for how long will determine the severity of symptoms, both acute and chronic.
Symptoms
The effects seen while the infant is exposed to high levels of bilirubin are termed acute bilirubin encephalopathy (ABE), while the long term effects that persist after the hyperbilirubinemia has resolved, either naturally or as a result of treatment, are called chronic bilirubin encephalopathy (CBE). The latter is also sometimes simply called kernicterus. Bilirubin-Induced Neurological Dysfunction (BIND) is used to describe long lasting abnormalities that are less obviously debilitating than classic kernicterus or CBE.
Causes
Bilirubin encephalopathy (BE) is caused by very high levels of bilirubin. Bilirubin is a yellow pigment that is created as the body gets rid of old red blood cells. High levels of bilirubin in the body can cause the skin to look yellow (jaundice).
While jaundice is often a natural occurrence in newborns and infants, BE is something of an anomaly, and can be caused by non-natural factors. For example, if your newborn exhibits signs of jaundice but his or her doctor does not diagnose it or treat it in a timely manner, it can increase in severity to BE, putting your baby at risk.
Further, if your infant’s healthcare provider does not realize the severity of jaundice or BE, or other conditions that may exacerbate the situation, your infant may be placed at risk for a wide variety of dangerous side effects.
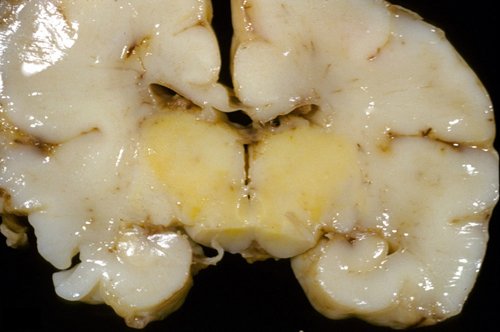
If the level of bilirubin is very high or a baby is very ill, the substance will move out of the blood and collect in the brain tissue if it is not bound to albumin (protein) in the blood. This can lead to problems such as brain damage and hearing loss. The term “kernicterus” refers to the yellow staining caused by bilirubin. This is seen in parts of the brain on autopsy.
This condition most often develops in the first week of life, but may be seen up until the third week. Some newborns with Rh hemolytic disease are at high risk for severe jaundice that can lead to this condition. Rarely, BE can develop in seemingly healthy babies.
Acute Bilirubin Encephalopathy (ABE)
ABE develops progressively in response to the entry of bilirubin into brain tissues. The symptoms at first can be subtle and are not always recognized immediately. The medical literature identifies three phases of ABE, usually termed initial, intermediate and advance.
The initial phase is characterized by the infant not feeding well, being lethargic with a decreased muscle tone (mild hypotonia) and a high pitched cry.
If the hyperbilirubinemia persists, the intermediate phase of ABE shows continued lethargy alternating with irritability and an increase or decrease of muscle tones at different times. Usually there is some arching of the back — the beginnings of retrocollis and/or opisthotonos and the infant has a shrill or high pitched cry and is difficult to console.
The advanced phase is characterized by an intensification of the retrocollis and opisthotonus, producing arching, and inconsolable crying with a shrill cry. If the bilirubin levels are not reduced, the symptoms may progress to seizures or coma and eventually death.
Chronic Bilirubin Encephalopathy (CBE) known as Kernicterus
If bilirubin levels are not reduced in time to prevent neurotoxicity, chronic irreversible encephalopathy is a likely outcome (commonly called kernicterus). The long term effects encompass a range of neuromotor disorders that are referred to as “extrapyramidal” abnormalities because of the particular nerve tracts in the brain that are affected by bilirubin.
These disorders can be severe enough to include a form of cerebral palsy and a paralysis of upward gaze. Disturbances of hearing is very characteristic of bilirubin toxicity and may be one of the most sensitive indicators of it, assessed by a technique called auditory brainstem-evoked response (ABR). The disturbance may take the form of difficulties in locating sounds or understanding speech, but may also include actual hearing loss. Dental enamel dysplasia of the deciduous (baby) teeth is also common.
The issue of intellectual handicaps is a difficult one. The literature contains claims that cognitive deficits are a symptom of CBE, but there are other claims that this is solely due to the difficulty of assessing intellectual capacity in children who suffer severe hearing impairment and have difficulties in controlling muscle movements (dystonia).
Bilirubin-Induced Neurological Dysfunction (BIND)
BIND refers to the more subtle signs of bilirubin induced brain injury that are beginning to be recognized. They include learning disabilities that may be caused by disturbances of auditory and speech processing, as well as visual-motor difficulties leading to problems with coordination, balance and muscle tone.
Complications
Speak immediately with a Cleveland birth injury attorney at the Becker Law Firm if you believe that complications of untreated jaundice caused serious harm to your child. An attorney will evaluate the details of the situation and determine if a doctor or other healthcare provider may be held liable. You may be entitled to compensation to cover damages through a medical malpractice claim.
When jaundice is not treated immediately or properly, it can progress to a dangerous condition called acute bilirubin encephalopathy (ABE). The elevated levels of bilirubin, which is responsible for the yellowing of the skin in jaundice, move from the baby’s bloodstream to the brain.
This may be a precursor to a medical condition called kernicterus, or chronic bilirubin encephalopathy (CBE), which may be present if acute bilirubin encephalopathy is not reduced and causes permanent damage to the patient’s brain. Treating acute bilirubin encephalopathy may help prevent kernicterus.
Doctors and other healthcare professionals should be able to recognize signs that jaundice is present and/or worsening symptoms, which may indicate acute bilirubin encephalopathy.
Symptoms of ABE may include:
- vomiting;
- lethargy;
- fever;
- poor feeding/sucking;
- high-pitched cries;
- arching backwards (especially neck and head).
Treatment can range from phototherapy to more invasive measures such as a blood transfusion. It is vital that medical attention be given immediately, and every effort is made to prevent permanent brain damage.
Newborn baby jaundice is generally not a serious condition and may not require any type of medical treatment. But when it progresses, isn’t detected or is left untreated, there can be devastating consequences. If a healthcare professional did not properly follow a standard of care expected of other, reasonable professionals in similar situations, it may constitute negligence.
Treatment
Treatment depends on how old the baby is (in hours) and whether the baby has any risk factors (such as prematurity). It may include:
- Light therapy (phototherapy)
- Exchange transfusions (removing the child’s blood and replacing it with fresh donor blood or plasma)
Treating BE may include several processes and procedures, and most often depends on the overall health of your child, as well as the severity of the condition. Most commonly, treatment of BE includes:
Light Therapy
Light therapy is a common treatment method for jaundice and BE. Light therapy involves placing the infant under special lights that change bilirubin molecules so the infant can process them and pass them through stool and urine. This prevents bilirubin from attaching itself to surrounding tissue, or migrating to the baby’s brain. Light therapy is painless, and may be completed at the hospital or at home, depending on the severity of jaundice and your child’s overall health.
Intraveneous Immunoglobulin (IVIg)
When jaundice becomes more severe, IVIg may be necessary. IVIg is most commonly used when there are blood type differences between the mother and child, which result in antibodies negatively interacting with the baby’s blood cells. IVIg treatment is comprised of blood proteins that reduce negative antibodies and stabilize bilirubin levels in the infant’s bloodstream.
Exchange Transfusion
For severe cases of jaundice and BE, exchange transfusion may be necessary. Considered one of the most intensive forms of treatment for BE, exchange transfusion includes repeated withdrawal of blood from the infant (in small amounts). Next, the infant’s blood is diluted to remove maternal antibodies and bilirubin, and then is transferred back to the infant. This process is only conducted in the hospital, generally, in the Neonatal Intensive Care Unit (NICU).
Prevention
Treating jaundice or conditions that may lead to it can help prevent this problem. Infants with the first signs of jaundice have bilirubin level measured within 24 hours. If the level is high, the infant should be screened for diseases that involve the destruction of red blood cells (hemolysis).
All newborns have a follow-up appointment within 2 to 3 days after leaving the hospital. This is very important for late preterm or early term babies (born more than 2 to 3 weeks before their due date).
Risks of Bilirubin Encephalopathy?
The primary risks associated with BE are hearing loss, brain damage, or even death. In most cases, BE is treatable with few risks of long-term complications, but if the infant has other medical conditions or a compromised immune system, the effects of BE may be permanent.
0 200

No Comments